5.9 Peripheral Arterial Disease
Overview
Peripheral artery disease (PAD) is caused by atherosclerosis, with narrowed or blocked arteries, causing reduced oxygenated blood flow to the lower extremities. Risk factors for PAD are similar to atherosclerosis and include smoking, hypertension, high cholesterol, and inflammation. Additional risk factors include age and a history of diabetes or previous injuries or trauma to arterial vessels.[1]
See Figure 5.32[2] for an illustration of PAD.
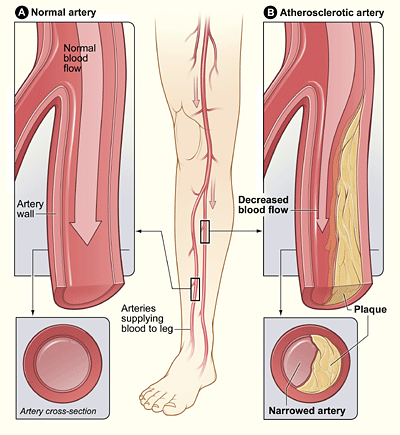
PAD can cause nonhealing wounds in the lower extremities that can become infected and lead to foot or leg amputation. PAD also increases a client’s risk for myocardial infarction and stroke.
The most common symptom of PAD is painful muscle cramping in the hips, thighs, or calves when walking, climbing stairs, or exercising called intermittent claudication. This pain typically resolves when the activity is stopped, although it may take a few minutes. The reason for this pain is working muscles need more oxygenated blood flow, and vessels occluded with atherosclerosis are unable to provide sufficient blood flow. This results in tissue ischemia and pain.
Assessment
Subjective and objective findings on assessment are related to diminished blood flow to the affected extremities and lack of oxygenation of the affected extremities.
Decreased perfusion to an affected limb may result in manifestations known as the 6P’s[3]:
- Pain
- Paralysis
- Paresthesia
- Pulselessness
- Pallor
- Poikilothermia
See Table 5.9 for common clinical manifestations of PAD across body systems.
Table 5.9. Clinical Manifestations of Peripheral Artery Disease[4],[5]
| Body System | Description |
|---|---|
| Musculoskeletal | – Intermittent claudication: Muscle pain, cramping, or fatigue during physical activity (e.g., walking) that resolves with rest and recurs with activity.
– Muscle wasting or atrophy in the affected limb(s) due to chronic reduced blood flow. |
| Cardiovascular | – Reduced or absent peripheral pulses (e.g., dorsalis pedis, posterior tibial) in the affected limb(s) due to reduced blood flow.
– Prolonged capillary refill time greater than three seconds. |
| Integumentary | – Skin may appear pale or blanched when elevated and dusky or red when lowered. It often feels cool to the touch.
– Hair loss on the lower limbs and thickened or brittle nails. – Development of nonhealing ulcers on the toes or feet. |
| Neurological | – Numbness, tingling, or weakness in the extremities due to reduced blood supply to the peripheral nerves. |
Diagnostic Testing
Health care providers may use a combination of noninvasive and invasive tests to evaluate blood flow and identify blockages in the arteries of the limbs, such as the following:
- Doppler Ultrasound: Identifies areas of arterial narrowing or blockage causing reduced blood flow in the extremity.
- Segmental Pressure Measurements: Identifies specific locations of arterial narrowing or blockage resulting in altered blood pressure using blood pressure readings at multiple levels along the leg (i.e., thigh, calf, ankle).
- Ankle-Brachial Index (ABI): Compares blood pressure in the arms (i.e., brachial artery) to the ankles (i.e., dorsalis pedis or posterior tibial arteries). A lower ABI indicates reduced blood flow to the lower extremities and suggests PAD.[6],[7]
Nursing Problems and Diagnoses
Nursing problems and diagnoses for peripheral artery disease (PAD) focus on managing symptoms and reducing the risk of complications.
Common nursing diagnoses for clients with peripheral arterial disease include the following[8]:
- Risk for Impaired Tissue Integrity R/T altered circulation
- Chronic Pain R/T decreased blood flow
- Readiness for Enhanced Health Self-Management
Outcome Identification
Outcome identification involves setting short- and long-term goals and creating expected outcome statements tailored to the client’s specific needs. These outcomes should be measurable and responsive to nursing interventions.
Sample expected outcomes for common nursing diagnoses related to peripheral arterial disease are as follows:
- The client will exhibit improved peripheral perfusion, as evidenced by decreased intermittent claudication, after completing a prescribed walking therapy program.
- The client will demonstrate intact skin with no new ulcers in the lower extremities.
- The client will accurately verbalize how to gradually improve collateral circulation by walking to the point of pain, resting, and then walking again for a prescribed length of time.
Interventions
Medical Interventions
Medical interventions for PAD aim to manage the conditions, reduce the risk of complications, and improve blood flow through the affected arteries. Interventions include lifestyle modifications, medication therapy, and surgical management.[9],[10]
Lifestyle Modifications
Lifestyle modifications for PAD include the following:
- Dietary Changes: A heart-healthy diet low in saturated fats, cholesterol, and sodium can help reduce plaque buildup.
- Regular Exercise: Regular physical activity can improve cardiovascular health. Prescribed walking therapy can promote the development of collateral circulation that reduces or resolves intermittent claudication.
- Smoking Cessation: Quitting smoking is crucial because smoking is a major risk factor for atherosclerosis and arterial injury.
- Weight Management: Achieving and maintaining a healthy weight can help improve blood pressure and reduce the workload on the heart.
- Blood Glucose Management: Tightly controlling blood glucose levels in clients with diabetes diminishes the progression of atherosclerosis.
Medication Therapy
Several medication classes may be prescribed to manage PAD:
- Statins: Lower LDL cholesterol levels and can reduce the risk of plaque buildup.
- Antiplatelet Drugs: Reduce the risk of thrombosis formation in plaques.
- Antihypertensive Medications: Control high blood pressure and reduce strain on the arteries.
- Anticoagulants: Prevent blood clots from forming in narrowed arteries.
- Vasodilators: Relax blood vessels and improve blood flow.
- Cholesterol Absorption Inhibitors: Reduce cholesterol absorption in the intestines.
- Thrombolytic Therapy: Eliminate blood clots in acute situations when blood flow is obstructed.
Read more information about these medication classes in “Cardiovascular & Renal System Medications” in Open RN Nursing Pharmacology, 2e.
Surgical Interventions[11]
- Angioplasty and Stent Placement: Percutaneous Transluminal Angioplasty (PTA) is a minimally invasive procedure in which a catheter is inserted into a narrowed artery and a balloon is inflated to compress the plaque and widen the artery. A stent may be inserted to help keep the artery open.
- Peripheral Bypass Grafting: In cases of severe arterial disease, surgical intervention may be recommended. This procedure involves bypassing blocked or narrowed arteries using grafts (usually veins or arteries from elsewhere in the body) to create new pathways for blood to flow to the skeletal muscle.
- Revascularization Procedures: Aortoiliac or femoropopliteal bypass may be performed to restore blood flow in specific arteries.
- Embolectomy: In cases of acute limb ischemia due to a clot or emboli, the clot is removed to restore blood flow.
Nursing Interventions
Nursing interventions for clients with PAD focus on medication management and health teaching to promote quality of life and reduce the risk of complications.
Medication Management
Nurses safely administer prescribed medications and monitor for side effects. The effectiveness of medications is evaluated and concerns are communicated with the health care provider.
Health Teaching
Nurses provide health teaching about lifestyle modifications, including walking therapy, dietary changes, and smoking cessation. Walking therapy, as prescribed based on the client’s abilities and limitations, is vital for developing collateral circulation. Clients are encouraged to walk to the point of pain, rest, and then resume walking for a specified period of time. A heart-healthy diet is encouraged that is low in saturated fats, cholesterol, and sodium. If the client smokes, resources for quitting smoking are provided. Risk factor modification is encouraged, including controlling blood pressure, cholesterol levels, and blood glucose.
Clients are instructed on limb positioning techniques that can improve blood flow, such as dangling when sitting unless edema is also present, in which case legs may be elevated but not above the level of the heart. Constrictive clothing and crossing the legs are discouraged. Clients are encouraged to closely examine their feet daily and to promptly report injuries or areas of skin breakdown to their health care provider.
Evaluation
During the evaluation stage, nurses determine the effectiveness of nursing interventions for a specific client. The previously identified expected outcomes are reviewed to determine if they were met, partially met, or not met by the time frames indicated. If outcomes are not met or only partially met by the time frame indicated, the nursing care plan is revised. Evaluation should occur every time the nurse implements interventions with a client, reviews updated laboratory or diagnostic test results, or discusses the care plan with other members of the interprofessional team.
View a supplementary YouTube video[12] explaining the differences between peripheral arterial and venous disease: Arterial insufficiency VS Venous insufficiency | William C. Fox Texas Endovascular
- Neschis, D. G., & Golden, M. A. (2022). Clinical features and diagnosis of lower extremity peripheral artery disease. UpToDate. Retrieved August 30, 2023, from https://www.uptodate.com/ ↵
- "Peripheral_Arterial_Disease.gif” by National Heart Lung and Blood Institute is in the Public Domain. ↵
- Natarajan, B., Patel, P., & Mukherjee, A. (2020). Acute lower limb ischemia-etiology, pathology, and management. International Journal Angiology. 29(3). 168-174. https;//doi.org/10.1055/s-0040-1713769 ↵
- Harris, L., & Dryjski, M. (2023). Epidemiology, risk factors, and natural history of lower extremity peripheral artery disease. UpToDate. Retrieved August 30, 2023, from https://www.uptodate.com/ ↵
- Neschis, D. G., & Golden, M. A. (2022). Clinical features and diagnosis of lower extremity peripheral artery disease. UpToDate. Retrieved August 30, 2023, from https://www.uptodate.com/ ↵
- Harris, L., & Dryjski, M. (2023). Epidemiology, risk factors, and natural history of lower extremity peripheral artery disease. UpToDate. Retrieved August 30, 2023, from https://www.uptodate.com/ ↵
- Neschis, D. G., & Golden, M. A. (2022). Clinical features and diagnosis of lower extremity peripheral artery disease. UpToDate. Retrieved August 30, 2023, from https://www.uptodate.com/ ↵
- Flynn Makic, M. B., and Martinez-Kratz, M. R. (2023). Ackley and Ladwig’s Nursing diagnosis handbook: An evidence-based guide to planning care. 13th edition. ↵
- Harris, L., & Dryjski, M. (2023). Epidemiology, risk factors, and natural history of lower extremity peripheral artery disease. UpToDate. Retrieved August 30, 2023, from https://www.uptodate.com/ ↵
- Neschis, D. G., & Golden, M. A. (2022). Clinical features and diagnosis of lower extremity peripheral artery disease. UpToDate. Retrieved August 30, 2023, from https://www.uptodate.com/ ↵
- Neschis, D. G., & Golden, M. A. (2022). Clinical features and diagnosis of lower extremity peripheral artery disease. UpToDate. Retrieved August 30, 2023, from https://www.uptodate.com/ ↵
- Texas Endovascular. (2016, November 20). Arterial insufficiency VS Venous insufficiency | WIlliam C. Fox Texas Endovascular. [Video]. YouTube. All rights reserved. https://www.youtube.com/watch?v=29-7zpOYWiM ↵
Caused by atherosclerosis, with narrowed or blocked arteries, causing reduced oxygenated blood flow to the lower extremities
Coolness in an affected limb.
Muscle pain, cramping, or fatigue during physical activity (e.g., walking) that resolves with rest and recurs with activity.
Identifies specific locations of arterial narrowing or blockage resulting in altered blood pressure using blood pressure readings at multiple levels along the leg
Compares blood pressure in the arms (i.e., brachial artery) to the ankles (i.e., dorsalis pedis or posterior tibial arteries)
A minimally invasive procedure in which a catheter is inserted into a narrowed artery and a balloon is inflated to compress the plaque and widen the artery

