10.9 Rheumatoid Arthritis
Rheumatoid arthritis (RA) causes symptoms such as bilateral joint pain, stiffness, and swelling. It is known for its pattern of remission and exacerbations, where symptoms might improve and worsen intermittently. Deformities may occur like a swan-like deformity of the hands (see Figure 10.37[1]) or boutonniere deformities, which are firm, observable lumps underneath the skin on or near the base of the joint (see Figure 10.38[2]).[3]
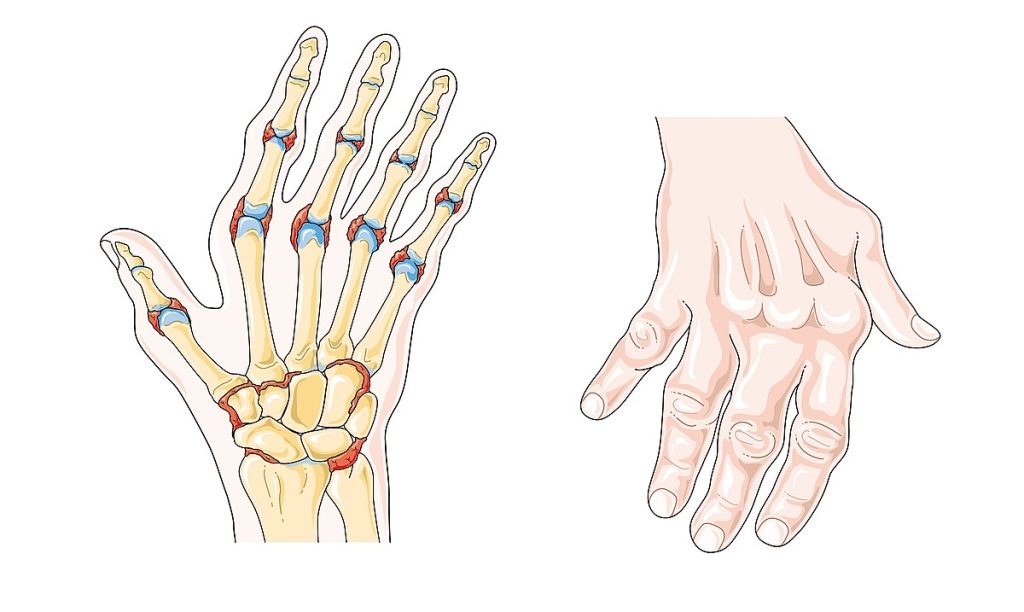
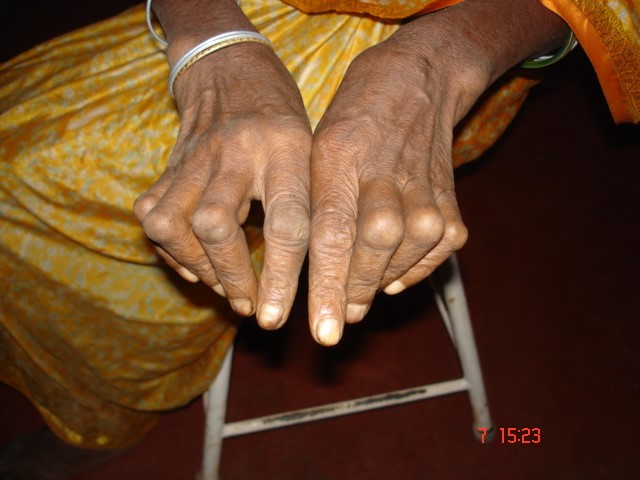
Several risk factors contribute to the development of RA. Women are more likely than men to develop RA, and it commonly begins between the ages of 20 and 50. Genetic predisposition also plays a significant role, so family history of RA can increase the likelihood of occurrence. Chronic stress has also been associated with RA because of its effect on the immune system.
Early diagnosis and appropriate management, including medications, physical therapy, and lifestyle modifications, aim to reduce inflammation, manage symptoms, and slow down joint damage progression in individuals with RA.[4]
Pathophysiology
RA is a chronic, systemic autoimmune disorder primarily affecting the synovial tissue (i.e., the lining of joints). The inflammatory process that occurs in RA is bilateral, meaning it affects both sides of the body, and often involves multiple joints simultaneously. The immune system’s attack on the synovial tissue causes chronic inflammation, which, if left untreated, can cause damage to the joint cartilage, bones, and other nearby structures.
Assessment
Physical assessment findings for rheumatoid arthritis vary based on early versus late stages of the disease. A summary of signs and symptoms of early and late stages of rheumatoid arthritis by body system is provided in Table 10.9.
Table 10.9. Manifestations of Early and Late Stages of Rheumatoid Arthritis[5],[6],[7]
| Body System | Early RA Physical Assessment Findings | Late RA Physical Assessment Findings |
|---|---|---|
| Musculoskeletal | Joint pain and tenderness; swelling, warmth, and erythema at affected joints; morning stiffness lasting greater than 30 minutes; symmetrical involvement of multiple joints (hands, wrists, etc.); muscle weakness; and fatigue | Severe joint deformities (e.g., swan-neck or boutonniere deformities), limited range of motion, joint contractures due to chronic inflammation, joint instability, and muscle wasting due to disuse |
| Eyes | Mild dryness or irritation | Scleritis (inflammation of the eye’s outer layers) |
| Cardiovascular | Pericardial friction rub may be heard in auscultation | Increased risk of cardiovascular diseases due to accelerated atherosclerosis |
| Respiratory | Mild pleuritic chest pain or dry cough | Pleurisy (inflammation of lung lining) or interstitial lung disease |
| Neurological | Numbness or tingling due to nerve compression or inflammation | Peripheral neuropathy |
Diagnostic Testing
Blood tests commonly ordered by health care providers to diagnosis RA include the following[8]:
- Rheumatoid Factor (RF) Antibody Assay: Detects atypical IgG and IgM antibodies commonly found in connective tissue disorders
- Antinuclear Antibody (ANA): Measures antibodies that target cell nuclei, contributing to tissue damage in autoimmune conditions
- Erythrocyte Sedimentation Rate (ESR): Confirms the presence of inflammation or infection throughout the body
- C-reactive Protein (CRP): Assists in gauging the level of inflammation present
Diagnostic testing may include X-rays, MRIs, and ultrasounds.
Nursing Problems and Diagnoses
For clients diagnosed with RA, nursing diagnoses often revolve around managing symptoms, promoting mobility, and providing support. Common nursing diagnoses for clients with RA include the following:
- Chronic Pain
- Impaired Mobility
- Fatigue
- Risk for Altered Skin Integrity
Outcome Identification
Outcome identification includes setting short- and long-term goals and creating expected outcome statements customized for the client’s specific needs. Expected outcomes are statements of measurable action for the client within a specific time frame that are responsive to nursing interventions. Sample expected outcomes for a client diagnosed with RA include the following:
- The client will report a reduction in pain levels to 3/10 or less on the pain scale within two weeks.
- The client will accurately demonstrate prescribed exercises and mobility-enhancing techniques within two weeks.
- The client will verbalize a reduction in fatigue levels, reporting increased energy to perform daily activities within three weeks.
- The client will maintain intact skin over nodules utilizing moisturizing techniques.
Interventions
Medical Interventions
Medical interventions include medication therapy and physical/occupational therapy.
Medication Therapy
Medication therapy focuses on managing symptoms, reducing inflammation, and slowing disease progression and may include the following medications[9],[10]:
- Analgesics, Nonsteroidal Anti-Inflammatory Drugs (NSAIDs), and Opioids: Acetaminophen, ibuprofen, naproxen, or opioids may be prescribed to manage chronic pain.
- Antimalarial Medications: Antimalarial medications like hydroxychloroquine and chloroquine may be prescribed for their anti-inflammatory properties to manage joint pain and fatigue and to prevent flare-ups.
- Steroids: Prednisone is a corticosteroid that can swiftly reduce inflammation and provide rapid relief. It is often prescribed for acute flare-ups of RA or as a short-term bridge therapy. Intra-articular injections of corticosteroids directly into affected joints can provide targeted relief from pain and inflammation, particularly when specific joints are severely affected.
- Immunosuppressants: Immunosuppressants help to slow down the immune system’s response that causes joint inflammation and damage. Cyclophosphamide is a potent immunosuppressant that may be considered in severe cases of RA.
- Disease-Modifying Anti-Rheumatic Drugs (DMARDs): Medications like methotrexate and sulfasalazine aim to slow or alter the disease progression by modifying the immune response. Methotrexate is one of the most commonly used DMARDs due to its effectiveness in reducing inflammation and slowing joint damage. DMARDs have potentially distressing and life-threatening side effects such as drug reaction with eosinophilia and systemic symptoms (DRESS), erythema multiforme, Stevens-Johnson syndrome, toxic epidermal necrolysis, torsades de pointes, hepatotoxicity, or aplastic anemia.
- Biological Response Modifiers: Also known as biologics, these medications target specific components of the immune system to reduce inflammation.
- Tumor Necrosis Factor (TNF) Inhibitors: Medications like infliximab and adalimumab are biologics that target TNF, a protein involved in the inflammatory response. They can effectively reduce symptoms and slow joint damage. However, caution is necessary as these medications can suppress the immune system, increasing susceptibility to infections. Therefore, they might not be suitable for clients with serious infections.
Physical/Occupational Therapy
Structured exercise programs and physical therapy are integral for maintaining joint flexibility, strength, and function. Customized exercises help manage pain, prevent muscle atrophy, and improve mobility. Occupational therapists assist clients in adapting their daily routines and environments to reduce strain on joints. They provide guidance on adaptive equipment and techniques for tasks like dressing, cooking, and using tools.[11]
Assistive devices such as splints, braces, or orthotics may be recommended to support and protect affected joints, reducing strain and improving function.[12]
Nursing Interventions
Pain Management
Nurses assess client’s pain levels using pain scales to effectively manage pain and evaluate the effectiveness of pain medications and nonpharmacological interventions such as heat or cold therapy, massage, or relaxation techniques.
Skin and Joint Care
Nurses assist in joint protection by reinforcing the effective use of splints or braces. If these devices are used, nurses perform skin assessments on areas at risk for skin breakdown and educate clients on proper skin care to prevent pressure injuries.
Health Teaching
Clients taking immune-suppression drugs must follow stringent infection control techniques to minimize the risk of infections. Nurses provide teaching on the following topics:
- Perform Good Hand and Personal Hygiene: Regular and thorough handwashing with soap and water or using alcohol-based hand sanitizers helps prevent the spread of infections. Maintaining good personal hygiene, including regular bathing and oral care, helps prevent the spread of bacteria and viruses.
- Avoid Individuals Who Are Ill: Clients should avoid close contact with individuals who are sick or showing possible signs of infection to reduce the risk of exposure.
- Stay Current on Vaccinations: Staying up-to-date on vaccinations, including flu shots and other recommended vaccines, can provide additional protection against preventable infections.
- Follow Safe Food Handling Practices: Ensuring that food is properly cooked and handling it with care help prevent foodborne illnesses.
- Avoid Crowded Places: Limiting exposure to crowded places, especially during flu seasons or outbreaks, can reduce the risk of coming into contact with infectious agents.
- Use Protective Equipment: Wear face masks, gloves, and other protective equipment in health care and crowded settings to provide an extra layer of protection.
- Maintain Environmental Hygiene: Keep living spaces clean. Regularly disinfect surfaces to help eliminate potential sources of infection.
- Monitor Symptoms: Monitor for signs of infection and seek prompt medical attention if symptoms arise.
- Communicate with Health Care Providers: Open communication with health care providers about symptoms, concerns, and any changes in health status is essential for proper management of RA.
Advocacy and Psychosocial Support
Nurses advocate for clients’ needs within the health care team, ensuring comprehensive care and addressing barriers to treatment. Nurses may collaborate with other health care professionals like physical therapists, occupational therapists, and rheumatologists to ensure a multidisciplinary approach to client care. Nurses promote optimal functioning and independence by providing health teaching on self-care and self-management of chronic illness, including joint protection, energy conservation, and the use of assistive devices to enhance independence.
Nurses also provide active listening and therapeutic communication while addressing the emotional impact of living with a chronic illness. Clients are encouraged to participate in support groups or other community resources to cope with chronic illness and maximize emotional well-being.
Evaluation
During the evaluation stage, nurses determine the effectiveness of nursing interventions for a specific client. The previously identified expected outcomes are reviewed to determine if they were met, partially met, or not met by the time frames indicated. If outcomes are not met or only partially met by the time frame indicated, the nursing care plan is revised. Evaluation should occur every time the nurse implements interventions with a client, reviews updated laboratory or diagnostic test results, or discusses the care plan with other members of the interprofessional team.
- “Rheumatoid_arthritis_--_Smart-Servier_(cropped).jpg" by Laboratoires Servier” is licensed under CC BY-SA 3.0 ↵
- "RA_hand_deformity.JPG" by Prashanthns is licensed CC BY-SA 3.0. ↵
- National Institute of Arthritis and Musculoskeletal and Skin Diseases. (2022, November). Rheumatoid arthritis. National Institutes of Health. https://www.niams.nih.gov/health-topics/rheumatoid-arthritis ↵
- Arthritis Foundation. (2021, October 15). Rheumatoid arthritis: Causes, symptoms, treatments and more. https://www.arthritis.org/diseases/rheumatoid-arthritis ↵
- Arthritis Foundation. (2021, October 15). Rheumatoid arthritis: Causes, symptoms, treatments and more. https://www.arthritis.org/diseases/rheumatoid-arthritis ↵
- National Institute of Arthritis and Musculoskeletal and Skin Diseases. (2022, November). Rheumatoid arthritis. National Institutes of Health. https://www.niams.nih.gov/health-topics/rheumatoid-arthritis ↵
- A.D.A.M. Medical Encyclopedia [Internet]. Atlanta (GA): A.D.A.M., Inc.; c1997-2024. Rheumatoid arthritis; [reviewed 2023, Jan. 25; cited 2023, Dec. 15). https://medlineplus.gov/ency/article/000431.htm ↵
- Johns Hopkins Medicine. (n.d.). Diagnosing bone disorders. https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/diagnosing-bone-disorders. ↵
- Arthritis Foundation. (2021, October 15). Rheumatoid arthritis: Causes, symptoms, treatments and more. https://www.arthritis.org/diseases/rheumatoid-arthritis ↵
- A.D.A.M. Medical Encyclopedia [Internet]. Atlanta (GA): A.D.A.M., Inc.; c1997-2024. Rheumatoid arthritis; [reviewed 2023, Jan. 25; cited 2023, Dec. 15). https://medlineplus.gov/ency/article/000431.htm ↵
- National Institute of Arthritis and Musculoskeletal and Skin Diseases. (2022, November). Rheumatoid arthritis. National Institutes of Health. https://www.niams.nih.gov/health-topics/rheumatoid-arthritis ↵
- National Institute of Arthritis and Musculoskeletal and Skin Diseases. (2022, November). Rheumatoid arthritis. National Institutes of Health. https://www.niams.nih.gov/health-topics/rheumatoid-arthritis ↵
A disease known for patterns of remission and exacerbation causing symptoms such as bilateral joint pain, stiffness, and swelling.
A bending in (flexion) of the base of the finger, a straightening out (extension) of the middle joint, and a bending in (flexion) of the outermost joint.
Observable lumps underneath the skin on or near the base of the joint.

