3.5 Anemia
Anemia is a condition characterized by a reduction in either the number of red blood cells, the amount of hemoglobin, or the hematocrit (percentage of red blood cells in the total blood volume). There are several types of anemia with different causes and treatments. Anemia itself is not a specific disease, but an abnormal condition that causes a decreased amount of oxygen delivered to body tissues, resulting in a variety of potential symptoms.[1]
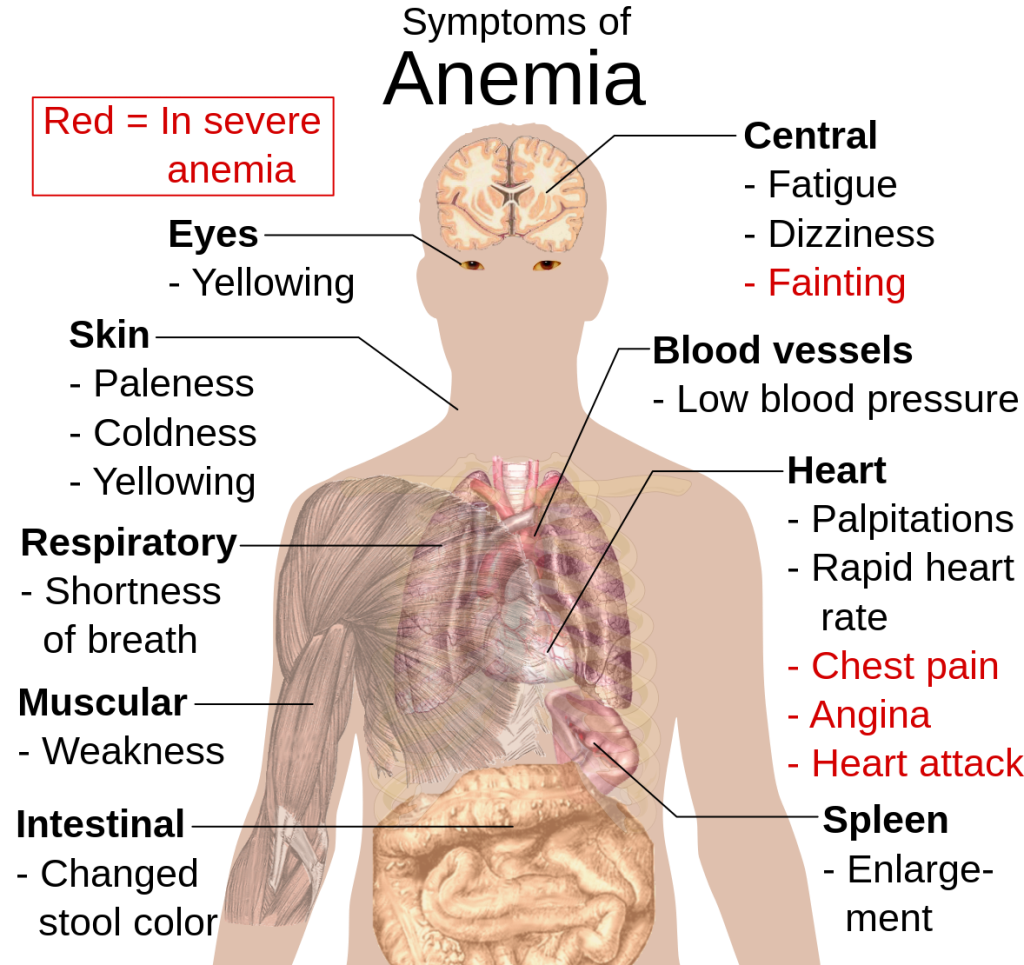
Common symptoms of anemia include fatigue, weakness, pale skin, unexplained shortness of breath, and heart palpitations.[2] Severe symptoms can include fainting, angina (chest pain), and myocardial infarction (heart attack). See Figure 3.7[3] for an illustration of the symptoms of anemia.
A common reason for anemia in adults is gastrointestinal (GI) bleeding that can be caused by various gastrointestinal disorders such as peptic ulcers, inflammatory bowel disease, or colorectal cancer. Another common reason for anemia in adult females is excessive menstrual bleeding. GI bleeding and excessive menstrual bleeding cause loss of red blood cells and decreased hemoglobin levels, resulting in symptoms of anemia.[4]
- American Society of Hematology. (n.d.). Anemia. https://www.hematology.org/education/patients/anemia ↵
- American Society of Hematology. (n.d.). Anemia. https://www.hematology.org/education/patients/anemia ↵
- “Symptoms_of_anemia.svg.png” by Mikael Häggström is licensed in the Public Domain ↵
- American Society of Hematology. (n.d.). Anemia. https://www.hematology.org/education/patients/anemia ↵
A clinical sign characterized by a reduction in either the number of red blood cells, the amount of hemoglobin, or the hematocrit (percentage of red blood cells in the total blood volume).

