8.2 Eye and Ear Basic Concepts
Anatomy of the Eye
Our sense of vision occurs due to transduction of light stimuli received through the eyes. The eyes are located within either orbit in the skull. See Figure 8.1[1] for an illustration of the eye. The eyelids, with lashes at their leading edges, help to protect the eye from abrasions by blocking particles that may land on the surface of the eye. The inner surface of each lid is a thin membrane known as the conjunctiva. The conjunctiva extends over the white areas of the eye called the sclera, connecting the eyelids to the eyeball. The iris is the colored part of the eye. The iris is a smooth muscle that opens and closes the pupil, the hole at the center of the eye that allows light to enter. The iris constricts the pupil in response to bright light and dilates the pupil in response to dim light. The cornea is the transparent front part of the eye that covers the iris, pupil, and anterior chamber. The cornea, with the anterior chamber and lens, refracts light and contributes to vision. The cornea can be reshaped by surgical procedures such as LASIK. The innermost layer of the eye is the retina that contains the nervous tissue and specialized cells called photoreceptors for the initial processing of visual stimuli. Two types of photoreceptors within the retina are the rods and the cones. The cones are sensitive to different wavelengths of light and provide color vision. These nerve cells of the retina leave the eye and enter the brain via the optic nerve (cranial nerve II).[2]
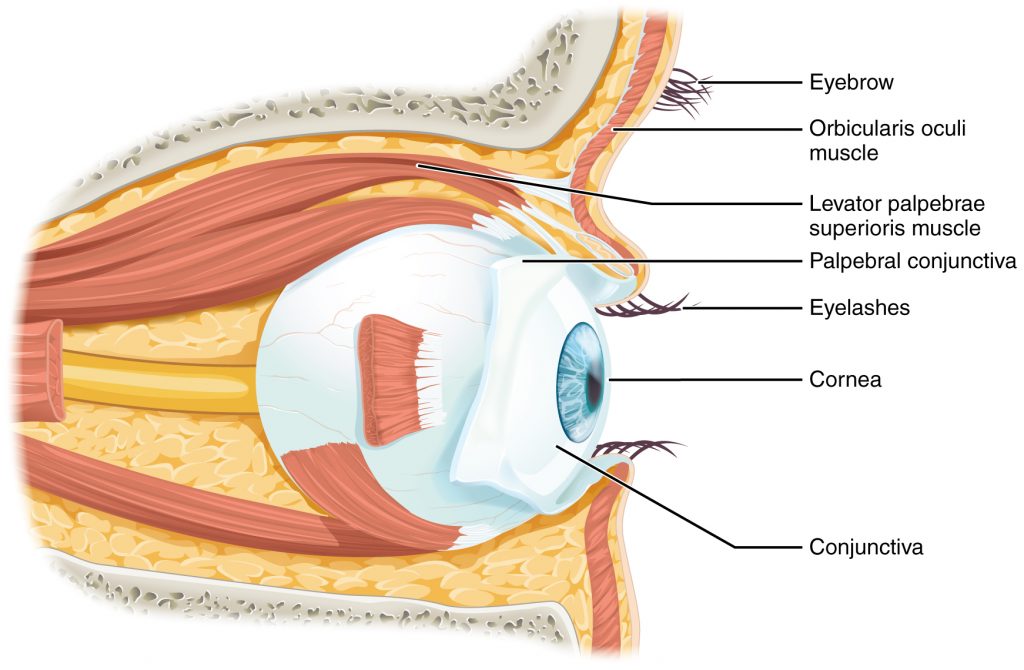
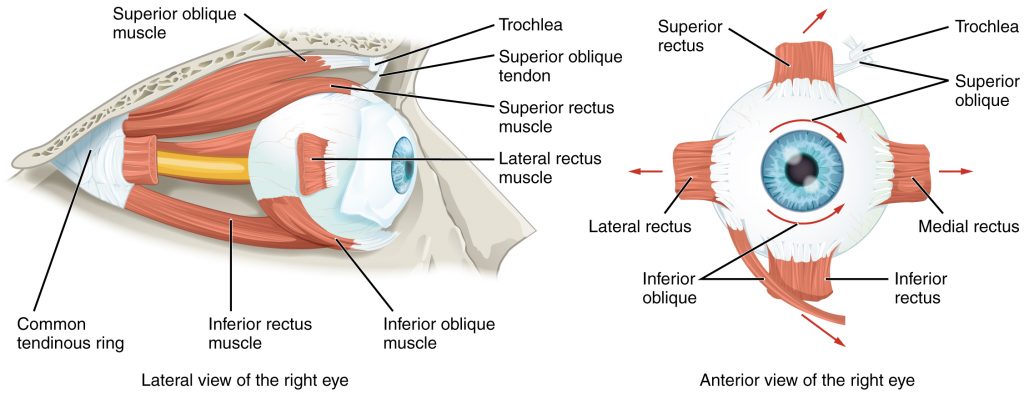
Tears are produced by the lacrimal gland that is located beneath the lateral edges of the nose. Tears flow through the lacrimal duct to the medial corner of the eye and flow over the conjunctiva to wash away foreign particles. Movement of the eye within the orbit occurs by the contraction of six extraocular muscles that originate from the bones of the orbit and insert into the surface of the eyeball. The extraocular muscles are innervated by the abducens nerve, the trochlear nerve, and the oculomotor nerve (cranial nerves III, IV, and V).[3] See the illustration of the extraocular muscles in Figure 8.2.[4]
Review for Anatomy of the Eye on YouTube[5]
Common Disorders of the Eye
Eye disorders that nurses commonly see in practice include myopia, presbyopia, color blindness, dry eye, conjunctivitis, styes, cataracts, macular degeneration, and glaucoma.
Myopia
Myopia is impaired vision, also known as nearsightedness that makes far-away objects look blurry. It happens when the eyeball grows too long from front to back or when there are problems with the shape of the cornea or the lens. These problems make light focus in front of the retina, instead of on it, causing blurriness. See Figure 8.3[6] for a simulated image of a person’s vision with myopia. Nearsightedness usually becomes apparent between ages 6 and 14. It is corrected with glasses, contacts, or LASIK surgery.[7]

Presbyopia
Presbyopia is impaired near vision. It commonly occurs in middle-aged and older adults, making it difficult to clearly see objects up close. As people age, the lens in the eye gets harder and less flexible and stops focusing light correctly on the retina.[8] Presbyopia can be corrected with glasses and/or contacts. See Figure 8.4[9] for a simulated image of a person’s vision with presbyopia.

Color Blindness
Color blindness makes it difficult to differentiate between certain colors. Color blindness can occur due to damage to the eye or to the brain. There’s no cure for color blindness, but special glasses and contact lenses can help people differentiate between colors. Most people who have color blindness are able to use visual strategies related to color selection and don’t have problems participating in everyday activities.[10]
Dry Eye
Dry eye is a very common eye condition that occurs when the eyes don’t make enough tears to stay wet or the tears don’t work correctly. Symptoms of dry eye include a scratchy feeling, stinging, and burning. Treatment includes over-the-counter and prescription eye drops, as well as lifestyle changes to decrease the dryness of the eyes.[11]
Conjunctivitis
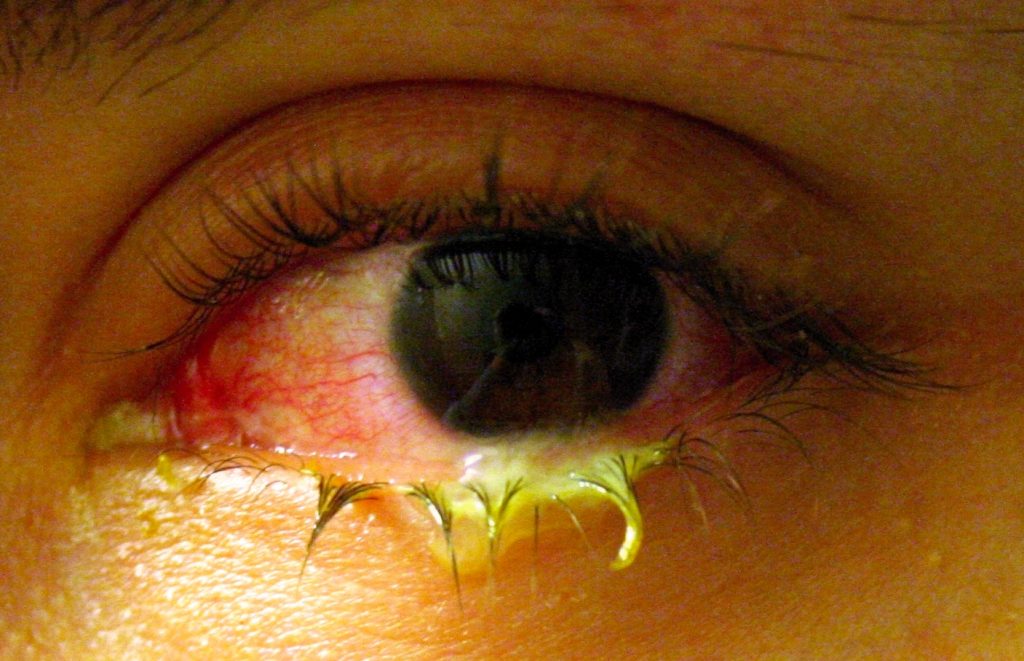
Conjunctivitis is a viral or bacterial infection that causes swelling and redness in the conjunctiva and sclera. See Figure 8.5[12] for an image of conjunctivitis. The eye may feel itchy and painful with crusty yellow drainage present. Conjunctivitis is very contagious, so the nurse should educate the patient and family caregivers to wash hands frequently. Additionally, the patient should not share items like pillowcases, towels, or makeup. Bacterial conjunctivitis is treated with antibiotic eye drops.[13]
Stye
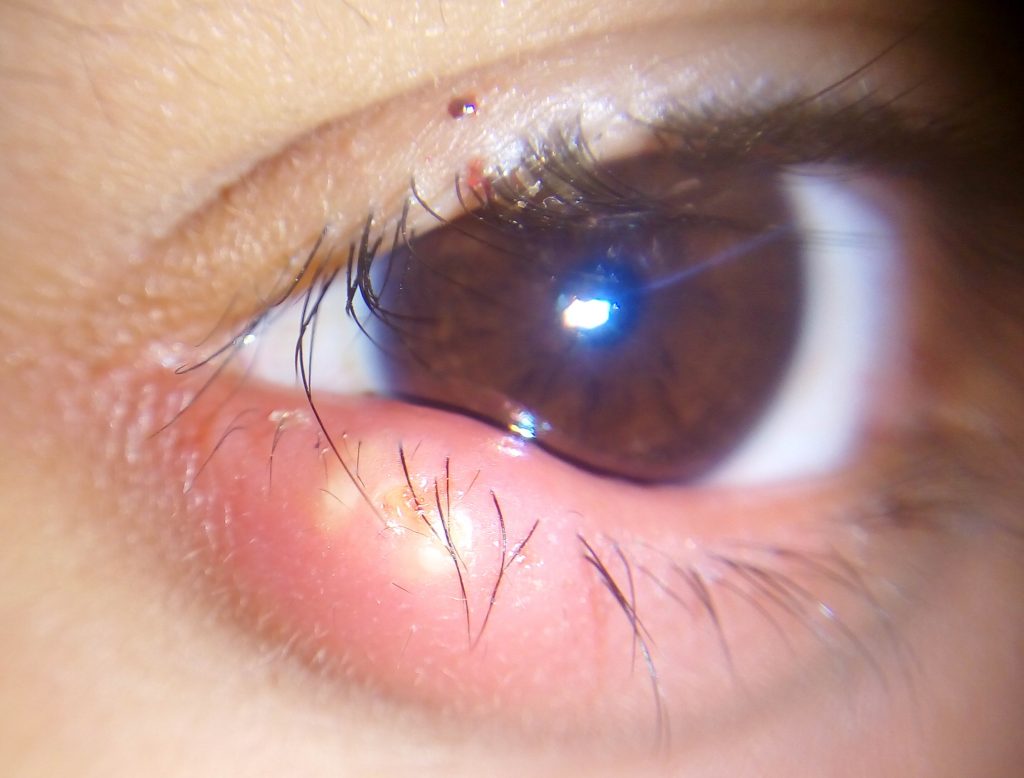
A stye is a bacterial infection of an oil gland in the eyelid, causing a red, tender bump at the edge of the eyelid. See Figure 8.6[14] for an image of a stye. Treatment includes applying warm compresses to the eyelid and prescription eyedrops.[15]
Cataracts
A cataract is a cloudy area on the lens of the eye. Cataracts are very common in older adults. Over half of all Americans age 80 or older either have cataracts or have had surgery to remove cataracts. See Figure 8.7[16] for an image of a cataract. Cataracts develop slowly and symptoms include faded colors, blurred or double vision, halos around light, and trouble seeing at night. See Figure 8.8[17] for a simulated image of a person’s vision with cataracts. Decreased vision due to cataracts may result in trouble reading and driving and increases the risk of falling. Patients often undergo surgery for cataracts. During cataract surgery, the doctor removes the clouded lens and replaces it with a new, artificial lens.[18]
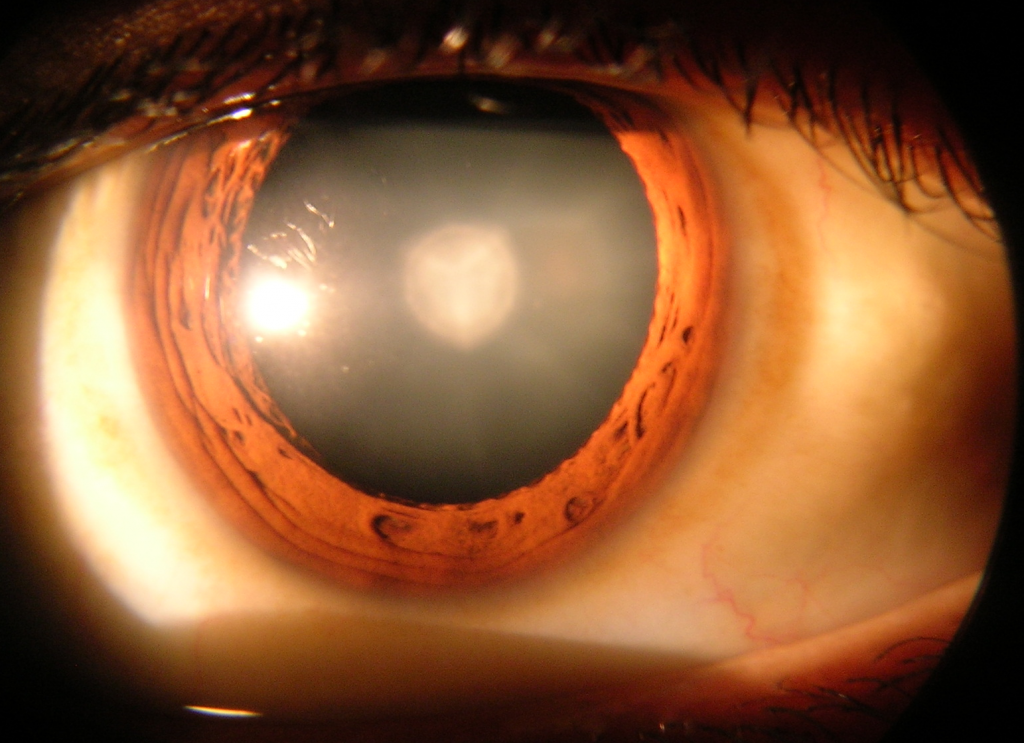

Macular Degeneration
Age-related macular degeneration is a common condition that causes blurred central vision. It is the leading cause of vision loss for people 50 and older. See Figure 8.9[19] for a simulated image of a person’s vision with macular degeneration. There are two types of macular degeneration: dry (nonexudative) and wet (exudative). During dry macular degeneration, cellular debris called drusen accumulates and scars the retina. In the wet (exudative) form, which is more severe, blood vessels grow behind the retina that leak exudate fluid, causing hemorrhaging and scarring. There is no treatment for dry macular degeneration, but laser therapy can be used to help treat wet (exudative) macular degeneration.[20]

Glaucoma
Glaucoma is a group of eye diseases that causes vision loss by damaging the optic nerve due to increased intraocular pressure. Treatment includes prescription eye drops to lower the pressure inside the eye and slow the progression of the disease. If not treated appropriately, glaucoma can cause blindness. Symptoms of glaucoma include gradual loss of peripheral vision. See Figure 8.10[21] for a simulated image of a person’s vision with glaucoma. Because the loss of vision occurs so slowly, many people don’t realize they have symptoms until the disease is well-progressed or it is discovered during an eye exam.[22]

Screening Tools for Eye Exams
Common screening tools used during an eye exam are the Snellen chart, a near vision chart, and Ishihara plates. Nurses working in outpatient settings or school settings use these tools when screening patients for vision problems. If a vision problem is identified, the patient is referred to an optometrist for further testing. When performing a vision assessment, be sure to provide adequate lighting.
Snellen Chart
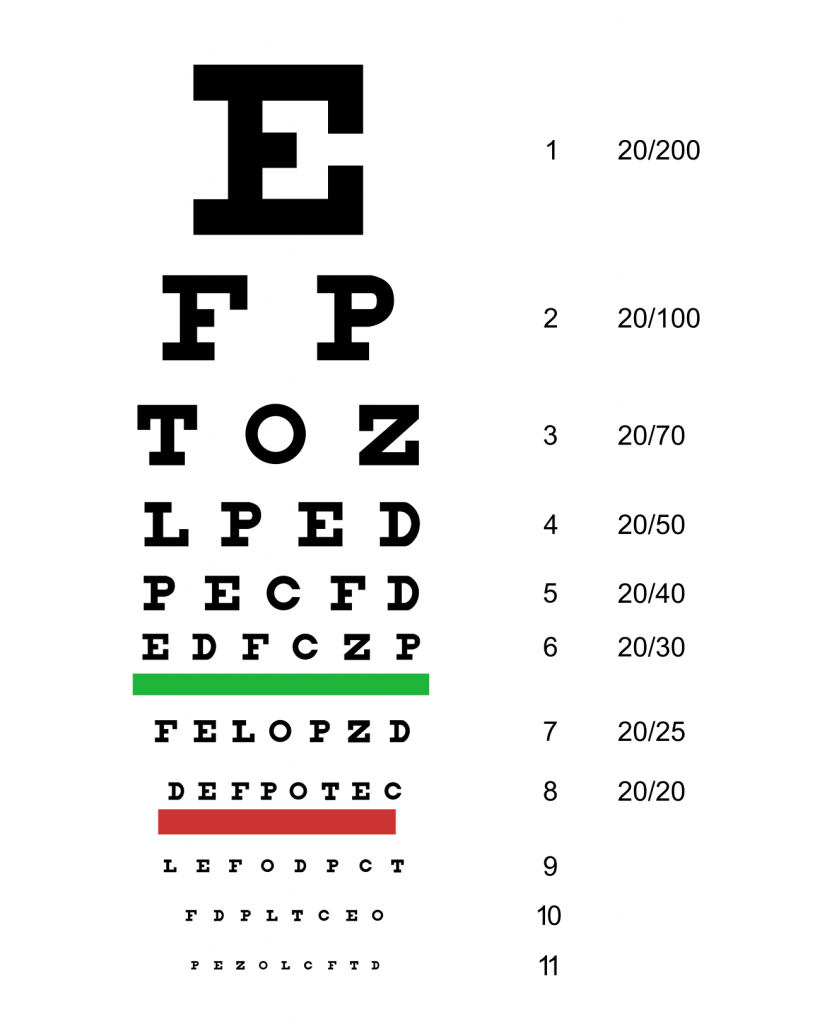
Distant vision is tested by using the Snellen chart. See Figure 8.11[23] for an image of the Snellen chart. Place the patient 20 feet away from the Snellen chart. Ask them to cover one eye and read the letters from the lowest line they can see clearly. Record the corresponding fraction in the furthermost right-hand column. Repeat with the other eye. If the patient is wearing glasses or contact lens during this assessment, document the results as “corrected vision” when wearing these assistive devices.
A person with no visual impairment is documented as having 20/20 vision. A person with impaired vision has a different lower denominator of this fraction. For example, a vision measurement of 20/30 indicates the patient can see letters clearly at 20 feet that a person with normal vision can see clearly at 30 feet.[24] Alternative charts are also available for children or adults who can’t read letters in English. See Figure 8.12[25]for an alternative eye chart.

Near Vision
Near vision is assessed by having a patient read from a prepared card that is held 14 inches away from the eyes. If a card is not available, the patient can be asked to read from a newspaper as an alternative quick screening tool. See Figure 8.13[26] for an image of a prepared card used to assess near vision.

Ishihara Plates
Ishihara plates are commonly used to assess color vision. Each of the colored dotted plates shows either a number or a path. See Figure 8.14[27] for an example of Ishihara plates. A person with color blindness is not able to distinguish the numbers or paths from the other colored dots on the plate.
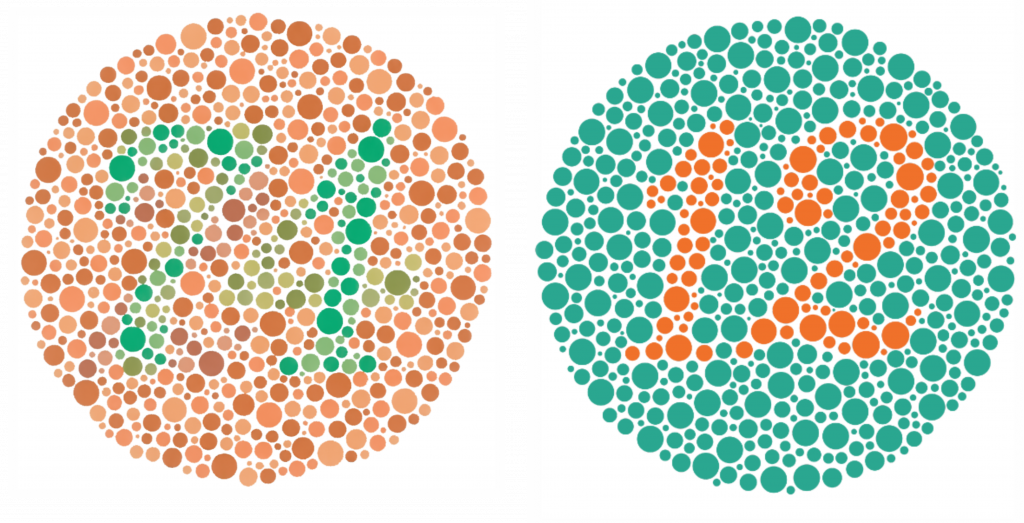
Anatomy of the Ear
Hearing is the transduction of sound waves into a neural signal by the structures of the ear. See Figure 8.15[28] for an image of the anatomy of the ear. The large, fleshy structure on the lateral aspect of the head is known as the auricle. The C-shaped curves of the auricle direct sound waves toward the ear canal. At the end of the ear canal is the tympanic membrane, commonly referred to as the eardrum, that vibrates after it is struck by sound waves. The auricle, ear canal, and tympanic membrane are referred to as the external ear. The middle ear consists of a space with three small bones called the malleus, incus, and stapes, the Latin names that roughly translate to “hammer,” “anvil,” and “stirrup.” The malleus is attached to the tympanic membrane and articulates with the incus. The incus, in turn, articulates with the stapes. The stapes is attached to the inner ear, where the sound waves are transduced into a neural signal. The middle ear is also connected to the pharynx through the Eustachian tube that helps equilibrate air pressure across the tympanic membrane. The Eustachian tube is normally closed but will pop open when the muscles of the pharynx contract during swallowing or yawning. The inner ear is often described as a bony labyrinth because it is composed of a series of semicircular canals. The semicircular canals have two separate regions, the cochlea and the vestibule, that are responsible for hearing and balance. The neural signals from these two regions are relayed to the brain stem through separate fiber bundles. However, they travel together from the inner ear to the brain stem as the vestibulocochlear nerve (cranial nerve VIII).[29]
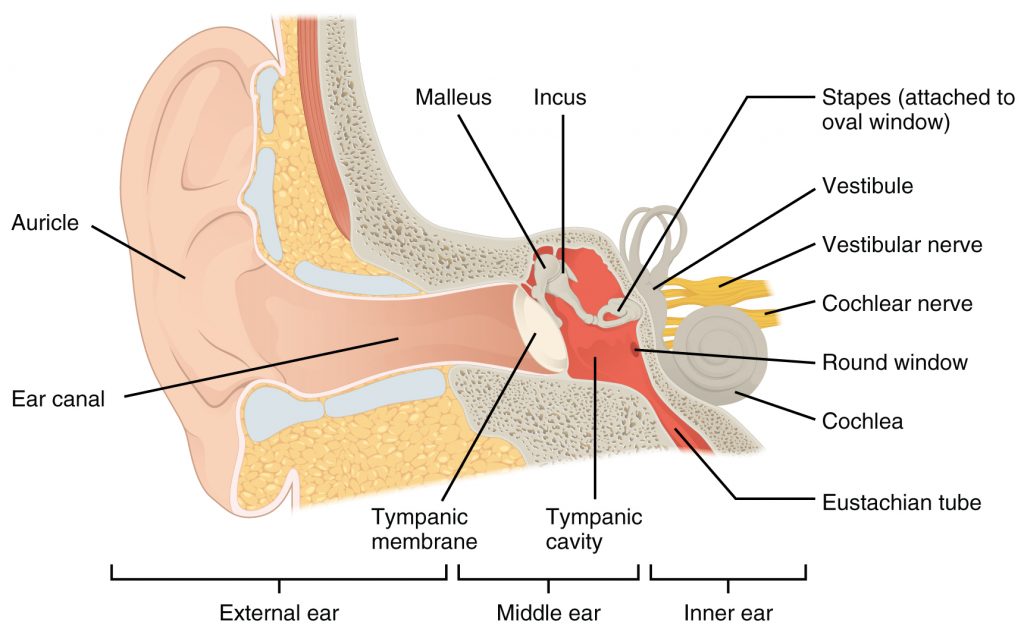
Hearing
Sound waves cause the tympanic membrane to vibrate. This vibration is amplified as it moves across the malleus, incus, and stapes and into the cochlea. Within the inner ear, the cochlear duct contains sound-transducing neurons. As the frequency of a sound changes, different hair cells within the cochlear duct are sensitive to a particular frequency. In this manner, the cochlea separates auditory stimuli by frequency and sends impulses to the brain stem via the cochlear nerve. The cochlea encodes auditory stimuli for frequencies between 20 and 20,000 Hz, the range of sound that human ears can detect.[30]
Balance
Along with hearing, the inner ear is also responsible for the sense of balance. Semicircular canals in the vestibule have three ring-like extensions. One extension is oriented in the horizontal plane, and the other two are oriented in the vertical plane. Hair cells within the vestibule sense head position, head movement, and body motion. By comparing the relative movements of both the horizontal and vertical planes, the vestibular system can detect the direction of most head movements within three-dimensional space. However, medical conditions affecting the semicircular canals cause incorrect signals to be sent to the brain, resulting in a spinning type of dizziness called vertigo.
Review of Anatomy of the Ear on YouTube[31]
Common Ear Disorders
Hearing Loss
Hearing loss is classified as conductive hearing loss or sensorineural hearing loss. Conductive hearing loss occurs when something in the external or middle ear is obstructing the transmission of sound. For example, cerumen impaction or a perforated tympanic membrane can cause conductive hearing loss. Sensorineural hearing loss is caused by pathology of the inner ear, cranial nerve VIII, or auditory areas of the cerebral cortex. Presbycusis is sensorineural hearing loss that occurs with aging due to gradual nerve degeneration. Ototoxic medications can also cause sensorineural hearing loss by affecting the hair cells in the cochlea.
Acute Otitis Media
Acute otitis media is the medical diagnosis for a middle ear infection. Ear infections are a common illness in the pediatric population. Children between the ages of 6 months and 2 years are more susceptible to ear infections because of the size and shape of their Eustachian tubes. Acute otitis media typically occurs after an upper respiratory infection when the Eustachian tube becomes inflamed and the middle ear fills with fluid, causing ear pain and irritability. This fluid can become infected, causing purulent fluid and low-grade fever. Acute otitis media is diagnosed by a health care provider using an otoscope to examine the tympanic membrane for bulging and purulent fluid. If not treated, acute otitis media can potentially cause perforation of the tympanic membrane. Treating early acute otitis media with antibiotics is controversial in the United States due to the effort to prevent antibiotic resistance. However, the treatment goals are to control pain and treat infection with antibiotics if a bacterial infection is present.[32]
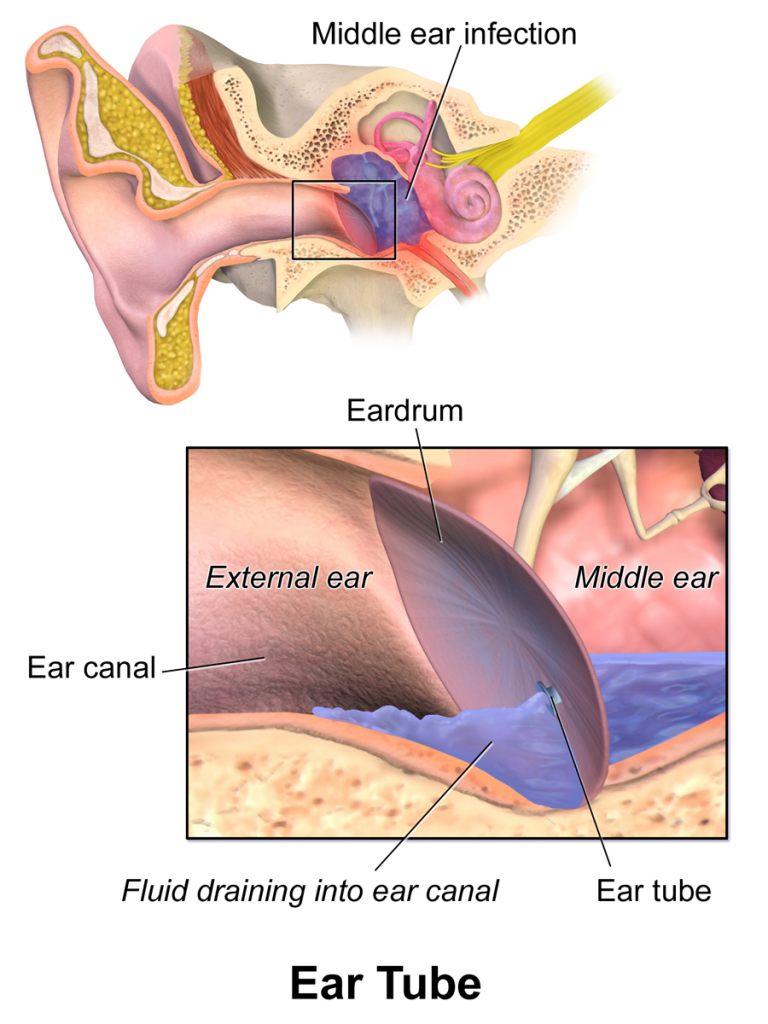
Some children develop recurrent ear infections that can cause hearing loss affecting their language development. For children experiencing recurring cases, a surgery called myringotomy surgery is performed by an otolaryngologist. During myringotomy surgery, a tympanostomy tube is placed in the tympanic membrane to drain fluid from the middle ear and prevent infection from developing. If a child has a tympanostomy tube in place, it is expected to see clear fluid in their ear canal as it drains out of the tube. See Figure 8.16[33] for an image of a tympanostomy tube in the ear.[34]
Otitis Externa
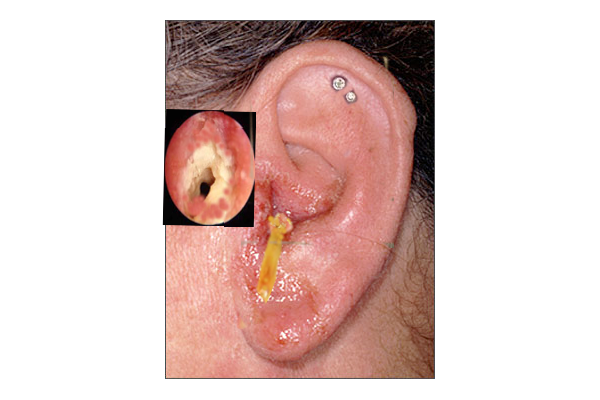
Otitis externa is the medical diagnosis for external ear inflammation and/or infection. See Figure 8.17[35] for an image of otitis externa. It is commonly known as “swimmer’s ear” because it commonly occurs in swimmers, especially in summer months. Otitis externa can occur in all age groups and causes an erythematous and edematous ear canal with associated yellow, white, or grey debris. Patients often report itching in the ear canal with pain that is worsened by pulling upwards and outwards on the auricle. Otitis externa is treated with antibiotic drops placed in the ear canals.[36]
Cerumen Impaction
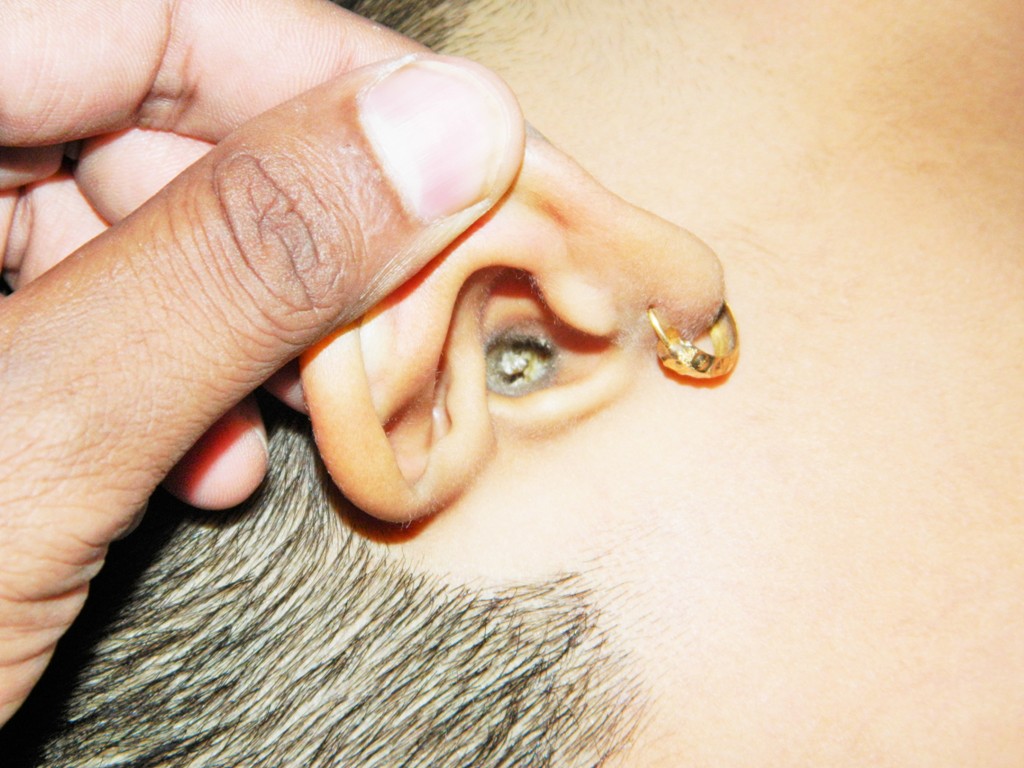
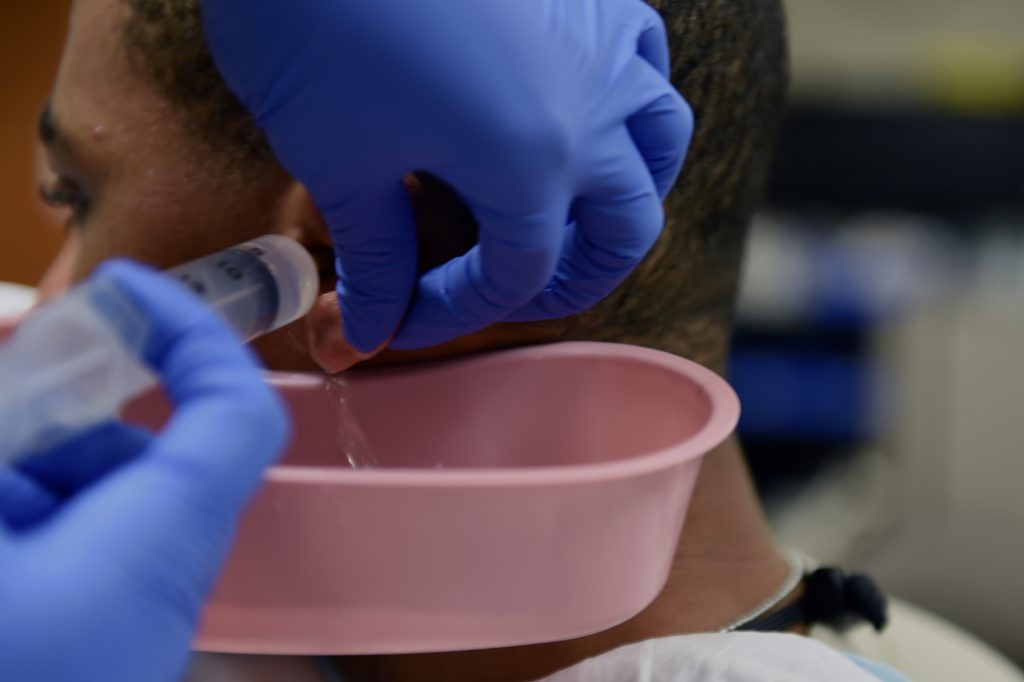
Cerumen impaction refers to a buildup of earwax causing occlusion of the ear canal. This occlusion often causes symptoms such as hearing loss, ear fullness, and itching. See Figure 8.18[37] for an image of cerumen impaction. Cerumen can be removed via irrigation of the ear canal, ear drops to dissolve the wax, or manual removal.[38] In outpatient settings, nurses often assist with ear irrigation to remove cerumen impaction according to agency policy. See Figure 8.19[39] for an image of an ear irrigation procedure.
Tinnitus
Tinnitus is a ringing, buzzing, roaring, hissing, or whistling sound in the ears. The noise may be intermittent or continuous. Tinnitus can be caused by cerumen impaction, noise trauma, or ototoxic medications, such as diuretics or high doses of aspirin. Military personnel have a high incidence of tinnitus due to noise trauma from loud explosions and gunfire. There are no medications to treat tinnitus, but patients can be referred to an otolaryngologist for treatment such as cognitive therapy or noise masking.[40]
Vertigo
Vertigo is a type of dizziness that is often described by patients as, “the room feels as if it is spinning.” Benign positional vertigo (BPV) is a common condition caused by crystals becoming lodged in the semicircular canals in the vestibule of the inner ear that send false movement signals to the brain. BPV can be treated by trained professionals using a specific set of maneuvers that guide the crystals back to the chamber where they are supposed to be in the inner ear.[41]
- “1411 Eye in The Orbit.jpg” by OpenStax College is licensed under CC BY 3.0. Access for free at https://openstax.org/books/anatomy-and-physiology/pages/14-1-sensory-perception ↵
- Giddens, J. (2007). A survey of physical examination techniques performed by RNs: Lessons for nursing education. Journal of Nursing Education, 46(2), 83-87. ↵
- This work is a derivative of Anatomy & Physiology by OpenStax and is licensed under CC BY 4.0. Access for free at https://openstax.org/books/anatomy-and-physiology/pages/1-introduction ↵
- “1412 Extraocular Muscles.jpg” by OpenStax is licensed under CC BY 3.0. Access for free at https://openstax.org/books/anatomy-and-physiology/pages/14-1-sensory-perception ↵
- Forciea, B. (2015, May 12). Anatomy of the eye (v2.0) [Video]. YouTube. All rights reserved. Video used with permission. https://youtu.be/HmKGyJUcRLw ↵
- “Eye disease simulation, myopia.jpg” by National Eye Institute, National Institutes of Health is in the Public Domain. ↵
- National Eye Institute. (2019, July 9). Types of refractive errors. https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/refractive-errors/types-refractive-errors#section-id-6802 ↵
- National Eye Institute. (2019, July 9). Types of refractive errors. https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/refractive-errors/types-refractive-errors#section-id-6802 ↵
- “Pesto ingredients - blurred.jpg” by Colin is licensed under CC BY-SA 4.0 ↵
- National Eye Institute. (2019, July 3). Color blindness. https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/color-blindness ↵
- National Eye Institute. (2019, July 5). Dry eye. https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/dry-eye ↵
- “Swollen eye with conjunctivitis.jpg” by Tanalai at English Wikipedia is licensed under CC BY 3.0 ↵
- National Eye Institute. (2019, July 8). Causes of pink eye. https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/pink-eye/causes-pink-eye ↵
- “External hordeolum.jpg” by Inrankabirhossain is licensed under CC BY-SA 4.0 ↵
- National Eye Institute. (2019, July 2). Blepharitis. https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/blepharitis ↵
- “Cataract in human eye.png” by Rakesh Ajuja, MD is licensed under CC BY-SA 3.0 ↵
- “Eye disease simulation, cataract.jpg” by National Eye Institute, National Institutes of Health is in the Public Domain. ↵
- National Eye Institute. (2019, August 3). Cataracts. https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/cataracts ↵
- “Eye disease simulation, age-related macular degeneration.jpg” by National Eye Institute, National Institutes of Health is in the Public Domain. ↵
- National Eye Institute. (2020, August 17). Age-related macular degeneration. https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/age-related-macular-degeneration ↵
- “Eye disease simulation, glaucoma.jpg” by National Eye Institute, National Institutes of Health is in the Public Domain. ↵
- National Eye Institute. (2020, July 28). Glaucoma. https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/glaucoma ↵
- “Snellen chart.jpg” by Jeff Dahl is licensed under CC BY-SA 3.0 ↵
- Sue, S. (2007). Test distance vision by using a Snellen chart. Community Eye Health, 20(63), 52. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2040251/ ↵
- “US Navy 070808-N-6278K-128 Hospital Corpsman 3rd Class Edward Mace, an optician attached to the Military Sealift Command (MSC) hospital ship USNS Comfort (T-AH 20), instructs a patient on how to read an eye chart.jpg” by Mass Communication Specialist 2nd Class Joan E. Kretschmer for U.S. Navy is in the Public Domain. ↵
- “111012-F-ZT401-067.JPG” by Airman 1st Class Brooke P. Beers for U.S. Air Force is in the Public Domain. Access for free at https://www.pacaf.af.mil/News/Article-Display/Article/593609/keeping-sight-all-right/ ↵
- This work is a derivative of “Ishihara 9.png” and "Ishihara_1.png" by Shinobu Ishihara and in the Public Domain. ↵
- “1404 The Structure of the Ear.jpg” by OpenStax is licensed under CC BY 4.0 ↵
- This work is a derivative of Anatomy & Physiology by OpenStax and is licensed under CC BY 4.0. Access for free at https://openstax.org/books/anatomy-and-physiology/pages/1-introduction ↵
- This work is a derivative of Anatomy & Physiology by OpenStax and is licensed under CC BY 4.0. Access for free at https://openstax.org/books/anatomy-and-physiology/pages/1-introduction ↵
- Forciea, B. (2105, May 12). Anatomy of the ear (v2.0) [Video]. YouTube. All rights reserved. Video used with permission. https://youtu.be/A2ji_Vd8cuE ↵
- This work is a derivative of StatPearls by Danishyar and Ashurst and is licensed under CC BY 4.0 ↵
- “Ear Tube.png” by BruceBlaus is licensed under CC BY-SA 4.0 ↵
- This work is a derivative of StatPearls by Danishyar and Ashurst and is licensed under CC BY 4.0 ↵
- “Otitis externa.gif” by S. Bhjimji MD is licensed under CC BY 4.0. Access for free at https://www.ncbi.nlm.nih.gov/books/NBK556055/ ↵
- This work is a derivative of StatPearls by Medina-Blasini and Sharman and is licensed under CC BY 4.0 ↵
- “Ear Wax.JPG” by Anand2202 is licensed under CC BY-SA 4.0 ↵
- This work is a derivative of StatPearls by Mankowski and Raggio and is licensed under CC BY 4.0 ↵
- “150915-F-GO352-025.jpg” by Staff Sgt. Jason Huddleston for U.S. Air Force is licensed under CC0. Access for free at https://www.59mdw.af.mil/News/Article-Display/Article/647342/photo-essay-559th-medical-group-at-a-glance/ ↵
- This work is a derivative of StatPearls by Grossan and Peterson and is licensed under CC BY 4.0 ↵
- Woodhouse, S. (n.d.). Benign paraoxysmal positional vertigo (BPPV). Vestibular Disorders Association. https://vestibular.org/article/diagnosis-treatment/types-of-vestibular-disorders/benign-paroxysmal-positional-vertigo-bppv/ ↵
Inner surface of the eyelid.
White area of the eye.
Colored part of the eye.
The hole at the center of the eye that allows light to enter.
The transparent front part of the eye that covers the iris, pupil, and anterior chamber.
An inner part of the eye that helps the eye focus.
The nervous tissue and photoreceptors in the eye that initially process visual stimuli.
Cranial nerve II that conducts visual information from the retina to the brain.
Tears produced by the lacrimal gland flow through this duct to the medial corner of the eye.
Six muscles that control the movement of the eye within the orbit. Extraocular muscles are innervated by three cranial nerves, the abducens nerve, the trochlear nerve, and the oculomotor nerve.
Impaired vision, also known as nearsightedness, that makes far-away objects look blurry.
Impaired near vision that commonly occurs in middle-aged and older adults.
A viral or bacterial infection in the eye causing swelling and redness in the conjunctiva and sclera.
A chart used to test far vision.
The large, fleshy structure of the ear on the lateral aspect of the head.
The membrane at the end of the external ear canal, commonly called the eardrum, that vibrates after it is struck by sound waves.
Cranial nerve VIII that transports neural signals from the cochlea and the vestibule to the brain stem regarding hearing and balance.
Hearing loss that occurs when something in the external or middle ear is obstructing the transmission of sound.
Hearing loss caused by pathology of the inner ear, cranial nerve VIII, or auditory areas of the cerebral cortex.
Sensorineural hearing loss that occurs with aging due to gradual nerve degeneration.
Medications that cause the adverse effect of sensorineural hearing loss by affecting the hair cells in the cochlea.
The medical diagnosis for an middle ear infection.
The medical diagnosis for external ear inflammation and/or infection.
A buildup of ear wax causing occlusion of the ear canal.
A sound of ringing, buzzing, roaring, hissing, or whistling in the ears.
A type of dizziness often described by patients as “the room feels as if it is spinning".

