16.2 Basic Concepts
Topical and Transdermal Medications
Topical medications are medications that are administered via the skin or mucous membranes for direct local action, as well as for systemic effects. An inunction is a medication that is massaged or rubbed into the skin and includes topical creams such as nystatin antifungal cream. The transdermal route of medication administration includes patches or disks applied to the skin that deliver medication over an extended period of time. Common types of transdermal medications are analgesics (such as fentanyl), cardiac medications (such as nitroglycerin), hormones (such as estrogen), and nicotine patches (for smoking cessation). See Figure 16.1[1] for an image of typical packaging of a topical patch. Medications delivered transdermally provide a consistent level of the drug in the bloodstream for distribution. The transdermal route is also helpful for patients who are nauseated or having difficulty swallowing.
Heat may be applied with the administration of some inunctions. Heat causes vasodilation that enhances blood flow and improves absorption of some medication. However, heat should never be applied over patches, such as the fentanyl or nitroglycerin patches, because it increases the release of the drug and can cause overdose and death. Be sure to reference manufacturer recommendations regarding the application of heat.[2]
When applying transdermal patches, the nurse should always wear gloves and check the rights of medication administration as is done with other types of medication. Before applying a new patch, the old patch should be removed, the skin around the old patch should be assessed, and the site for the patch cleansed and dried thoroughly. The skin around the patch should be monitored for any irritation or reaction to the medication or patch adhesive. Patches should not be applied to broken or irritated skin.
When applying a new patch, the nurse should remove the clear plastic backing and take care to not touch the medication surface of the patch while placing it on the patient’s skin. Patches should be placed on an appropriate skin area per manufacturer guidelines, such as the upper arms or on the chest. The patch should be pressed firmly to the skin for ten seconds to ensure adhesion to the skin. For documentation purposes, the nurse should initial, date, and time a piece of tape that is applied close to the patch. If your agency allows you to mark the patch directly, please be sure to use a marking pen in order to not puncture the patch and render it ineffective. Based on the onset of the medication, the patient should be evaluated to ensure they are responding appropriately to the therapeutic effects of the medication and not experiencing any adverse effects.
Patch placement should be routinely assessed for dislodgement per agency policy. For example, for some opioid patches like fentanyl, the nurse is required to assess and document that the patch is present during every shift. The nurse should also be aware that patches with aluminum backing can cause issues with defibrillation and MRI scans, so this type of patch should be removed prior to either of these actions.
To remove a patch, the nurse should wear gloves and remove the patch carefully so as not to tear the skin. The patch should be disposed of in the proper waste receptacle per agency policy. For example, some agencies have specific receptacles for nitroglycerin patches. Additionally, agencies have specific policies for disposal of fentanyl patches to prevent drug diversion of used patches. Patch removal should be documented in the patient’s record.
Eye Instillations and Irrigations
Eye Drops
Eye drops are administered for a local effect on the eye. Examples of eye drop medications include antibiotic drops for conjunctivitis, glaucoma medication to reduce intraocular pressure, and saline drops to relieve dry eyes. The amount of drops to administer per eye is indicated on the provider order. When instilling eye drops, the nurse should perform hand hygiene, apply gloves, and check the same rights of medication administration as done with other types of medication. Prior to administration of eye medication, the patient’s eyes should be assessed for new or unusual redness or drainage. If discharge is present, the eyelids should be cleansed with gauze saturated with warm water or normal saline to remove any dirt or debris that could be carried into the eye during instillation. When cleaning the eyelids, the nurse should clean from the inner canthus toward the outer canthus so as not to introduce debris or dirt into the lacrimal ducts that could cause an infection. A new gauze pad is used for each stroke. The nurse should remove gloves after cleansing, perform hand hygiene, and apply new gloves prior to medication administration.
When administering the drops, the patient should be instructed to tilt their head backwards or be positioned in a supine position with their head on a pillow looking up. When the cap of the medication is removed, it should be placed on a clean surface with care taken to keep the inside of the cap sterile and to not contaminate the dropper tip. The patient should look up and away while the nurse gently uses pressure to pull the lower lid down and expose the lower conjunctival sac. By holding the dropper close to the sac without touching it, the nurse should squeeze the bottle and allow the drop to fall into the sac, taking care to not touch the dropper to the eye. After the eye drop has been instilled, the patient should close their eye. The nurse should apply gentle pressure to the inner canthus, when appropriate, to prevent the medication from entering the lacrimal duct and causing a possible systemic reaction to the medication. This procedure should be repeated in the other eye as ordered. The patient should be instructed to not to rub their eye(s). During the procedure, the nurse evaluates the patient’s tolerance of the medication and the procedure and documents it. See Figure 16.2[3] for an image of a nurse administering eye drops.
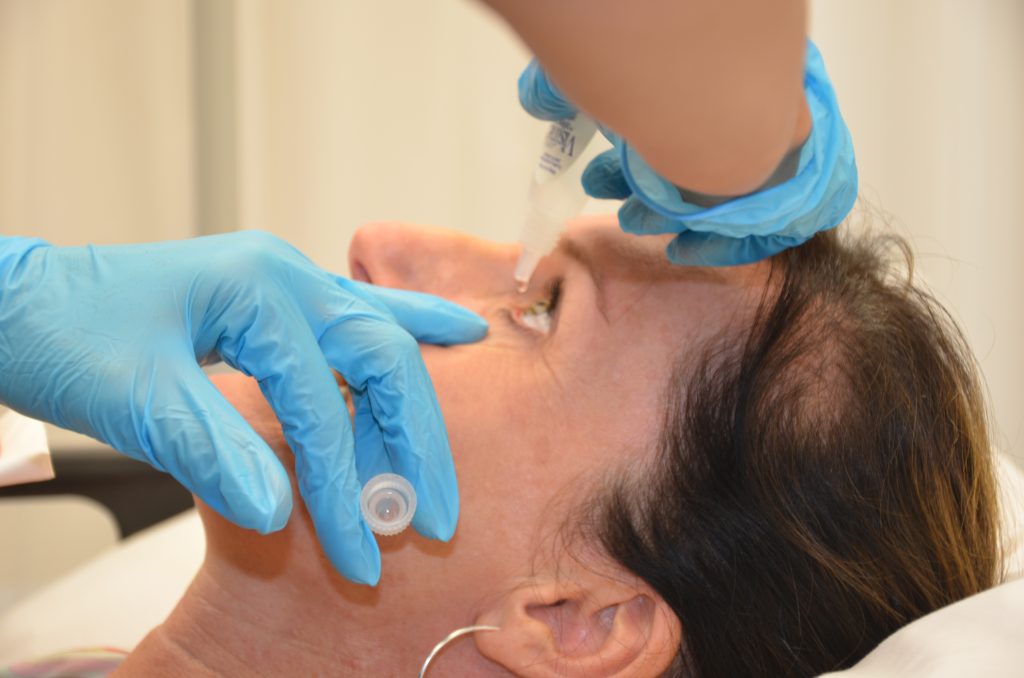
Review of Administering Eye Drops on YouTube[4]
Eye Ointment
Administering eye ointment follows the same procedure as administering eye drops, except that instead of drops, ½ inch of ointment is placed in the lower conjunctival sac. When applying the ointment, the nurse should start at the inner canthus and move outward. After application, the patient should be instructed to close their eyelid and move the eye to spread the ointment, so it is absorbed. They should be advised they may experience blurry vision for a few minutes until the medication is absorbed.
Eye Irrigations
Eye irrigations are used to flush foreign bodies from the eye, such as debris or chemicals, using large amounts of saline. The amount of solution and length of time used to irrigate the eye depends on the contaminant. Follow agency policy when performing eye irrigation. For example, some emergency eye flush stations provide a 15-minute flush to the eye. Care should be taken to not contaminate the other eye while removing the debris unless it is necessary to flush both eyes.
Ear Instillations and Irrigations
Medications and fluids may be instilled into the ear for local effect, including antibiotics, analgesics, wax softeners, and irrigation fluid to remove foreign objects or wax buildup. Medications and fluids are instilled into the outer ear canal, with the tympanic membrane forming a thin barrier to the middle and inner ear. However, if the tympanic membrane is ruptured, instillation of ear drops is generally contraindicated unless a sterile, no-touch technique is used. However, if a patient has a surgical opening in the tympanic membrane (i.e., tympanostomy tubes have been placed), ear drops may be prescribed but caution must be taken not to introduce debris into the middle or inner ear.
Ear Drops
When administering ear drops, the nurse should carefully follow the dosage and amount of drops per ear according to the provider order. The nurse should perform hand hygiene, apply gloves, and check the same rights of medication administration as is completed with other types of medication. The external ear should be cleaned of debris prior to drops being instilled. The patient should be positioned so the affected ear is tilted in the uppermost position. If the patient is lying in bed, position the patient so they are lying with the unaffected ear against the pillow and the affected ear upward. When removing the cap of the medication, caution should be used to not touch the dropper or the inside of the cap to avoid contamination. The pinna of the ear should be grasped and pulled backwards and upwards for an adult. For children, the pinna should be pulled straight back, and for infants, it should be pulled down and back. This movement straightens the auditory canal and prepares it for instillation. The nurse should squeeze the bottle so that the drops of medication fall onto the side of the auditory canal and not directly onto the tympanic membrane. The medication should run towards the tympanic membrane after it is instilled. The tragus can be massaged to help move the medication into place. The patient should remain in this lying position for five minutes. After five minutes, this procedure can be repeated on the other ear, if ordered. Evaluation of the patient should be performed post administration to assess if the patient tolerated the procedure and if anticipated therapeutic effects occurred. When instilling medication or fluids into the ear, monitor for side effects such as dizziness or nausea. See Figure 16.3[5] for an image of a nurse administering ear drops.
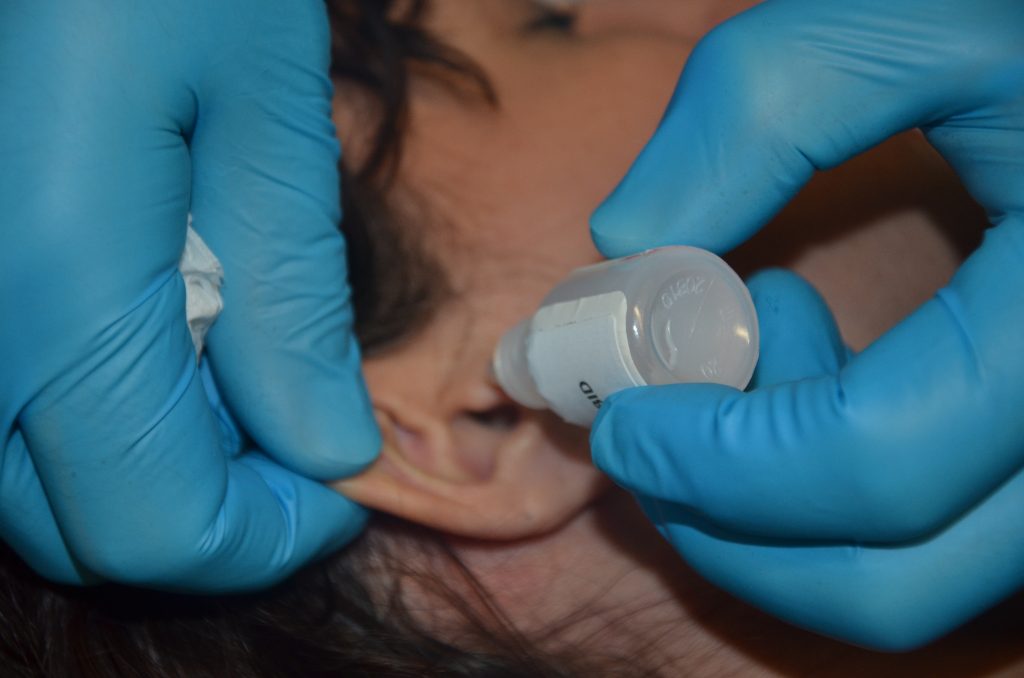
Ear Irrigations
Ear irrigations are typically performed to remove wax buildup or foreign bodies from the external ear canal. Normal saline at room temperature is typically used, although a mixture of saline and hydrogen peroxide can also be used. A 60-cc needleless syringe is typically used to irrigate the ear, or a spray bottle with a soft angiocatheter can also be used. Ask the patient to hold an emesis basin under the ear to catch the expelled irrigant. During and after the irrigation, the patient should be evaluated for side effects such as dizziness, nausea, or pain.
Nasal Instillation
Medications administered via the nasal passage are typically used to treat allergies, sinus infections, and nasal congestion. Nasal spray or drops should be administered via the nasal passage using a clean technique. The nurse should perform hand hygiene, apply gloves, and perform the same rights of medication administration as is completed with other types of medications. The patient should be given tissues and asked to blow their nose. Position the patient with their head tilted backwards while sitting or lying supine looking upwards. The nurse should insert the tip of the spray bottle or the nasal dropper into one nare while occluding the other nare and then activate the spray as the patient inhales. The bottle should remain compressed as it is removed from the nose to prevent contamination. The patient should be instructed to hold their breath for a few seconds and then breathe through their mouth. Repeat this procedure in the other nare if ordered. Wipe the outside of the bottle with clean tissue before storing it and advise the patient to avoid blowing their nose for 5-10 minutes after nasal instillation. Note any unexpected situations such as nosebleeds or increased congestion.[6]
Vaginal Instillations
Vaginal instillations are typically used to administer hormone therapy and antifungal treatment. Vaginal applications can be supplied in foams, suppositories that melt with body heat, creams, and tablets. The patient should be asked to void prior to placement. The nurse should perform hand hygiene, apply gloves, perform the same rights of medication administration as is completed with other types of medications, and provide privacy. Position the patient on their back with knees flexed. Perineal care should be performed by the nurse prior to administration of the medication. After perineal care, remove gloves, perform hand hygiene, and apply new gloves. Fill a vaginal applicator with cream or foam or open the suppository to be placed. Lubricate the applicator or your gloved finger with water-based lubricant. With the nondominant hand, spread the labia and place the applicator into the full length of the vagina, push the plunger, and then remove the applicator. If a suppository is being placed, insert the rounded end of the suppository with your index finger, placing it along the posterior wall of the vagina. Ask the patient to remain in the supine position for 5-10 minutes for optimal absorption. If possible, administer the medication at bedtime so the patient can remain in the supine position for an extended period of time to enhance absorption. Assess the patient for any unexpected situations, such as the suppository coming out. See Figure 16.4[7] for an illustration of vaginal administration of cream medication.
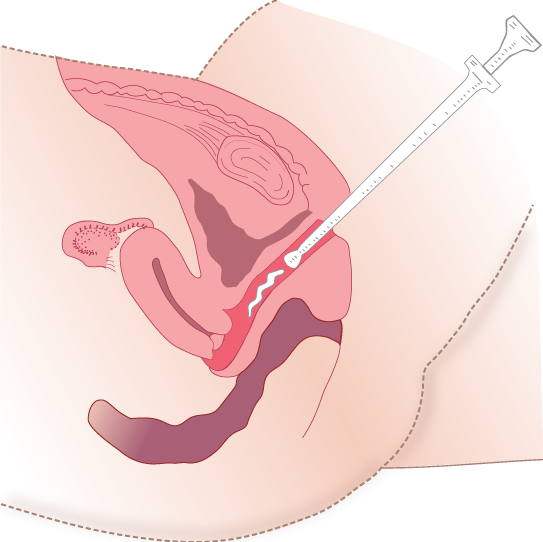
Inhaled Medications
The lungs have a large surface area with an increased amount of blood flow, so medications are easily absorbed. Medications inhaled from the mouth into the lungs can be administered using a metered dose inhaler (MDI), a dry powder inhaler (DPI), or a small-volume nebulizer. A metered dose inhaler (MDI) provides a mist of medication that is inhaled through the mouth into the lungs. See Figure 16.5[8] for an image of an albuterol MDI. However, during inhalation from an MDI, small medication particles can get trapped on the tongue or aerosolize into the air and not make it into the lungs, so a spacer is optimally used for full absorption of medication.

A DPI is medication provided in a powder form that is inhaled from the mouth into the lungs using a quick breath to activate the medication and move it into the lungs from the inhaler. An example of Advair Diskus DPI is illustrated in Figure 16.6.[9]
Hand-held, small-volume nebulizers provide a fine mist using oxygen or compressed air to transport the liquid medication from the nebulizer cup into the mouth and into the lungs as the patient breathes normally. See Figure 16.7[10] for an image of medication packaged for use with nebulizers.[11]

Before administering an inhaler, the nurse should perform hand hygiene and check medication rights as with all medication. If the patient is self-administering the medication, advise them to wash their hands. The patient’s respiratory system should be assessed and documented before and after the administration of inhaled medications, including assessment of respiratory rate, pulse oximetry, heart rate, and lung sounds.
When administering an MDI, the nurse should shake the inhaler and add a spacer onto the mouthpiece. The use of spacers with MDIs is considered best practice because they help ensure the medication is inhaled rather than inadvertently placed in the mouth. They also reduce waste by ensuring the patient receives the full amount of medication. The patient should be instructed to exhale while placing the spacer’s mouthpiece into their mouth. The inhaler is depressed to move the aerosolized medication into the spacer, and the patient should breathe in normally through the spacer to receive the medication. If a spacer is not available, the patient should exhale and hold the inhaler mouthpiece about 1 to 2 inches away from their mouth to help ensure the medication is inhaled via the larynx and not sprayed onto the posterior pharynx. As the inhaler is depressed, the patient should inhale the medication deeply through their mouth and into their lungs. The patient should be advised to hold their breath for 5 to 10 seconds after inhaling the medication and then exhale through pursed lips. The patient should wait for 1 to 5 minutes between each puff of medication. When administering inhaled corticosteroids via MDI, the patient should rinse their mouth with water afterwards to prevent fungal infection. See Figure 6.7[12] for an image of a spacer with a mask used in inhaler therapy with children.

When using a DPI, the nurse should load the medication into the devices as required and then activate the inhaler per the manufacturer’s guidelines. The patient should be instructed to exhale and then place their lips around the mouthpiece and inhale strongly and deeply. After they have inhaled, they should hold their breath for 10 seconds or as long as comfortable and then exhale through pursed lips. The patient should wait 1 to 5 minutes between puffs of medication. If the DPI contains a corticosteroid medication, the patient should gargle and rinse with tap water to decrease the risk of developing a fungal infection.[13]
When using a small-volume nebulizer, the nurse pours the liquid medication into the medication cup of the nebulizer. When possible, the patient should be sitting or positioned in high Fowler’s position to enhance deep breaths and absorption of medication. The bottom end of the tubing is attached to the oxygen flowmeter, and the flow rate should be set between 6-10 L/minute, based on the manufacturer’s recommendations. The top end of the tubing is connected to either a nebulizer mask or mouthpiece. The patient should be instructed to inhale slowly through the device into their mouth and hold each breath for a slight pause before exhaling. Remain with the patient during the nebulizer treatment, which usually takes about 15 minutes. After treatment, the patient should be encouraged to cough and perform oral care. The patient’s respiratory system should be reevaluated after the administration of inhaled medications to document therapeutic effects, as well as to monitor for adverse effects.[14]
Inhalers should be cleaned after use per the manufacturer’s directions. Most MDI and DPI inhalers track how much medication is left in the canister. Patients should be advised to obtain refills of these medications before the inhaler runs out of doses.
- “DSC_17661.jpg” by British Columbia Institute of Technology is licensed under CC BY 4.0. Access for free at https://opentextbc.ca/clinicalskills/chapter/administering-topical-medication/ ↵
- Institute for Safe Medication Practices. (2015). Transdermal patches and heat sources. NurseAdviseERR, 13(4). https://www.ismp.org/sites/default/files/attachments/2018-04/NurseAdviseERR201504.pdf ↵
- “Instilling eye medication” by British Columbia Institute of Technology is licensed under CC BY 4.0. Access for free at https://opentextbc.ca/clinicalskills/chapter/6-5-installing-eye-ear-and-nose-medications/ ↵
- RegisteredNurseRN. (2017, March 24). Eye drop administration nursing | Instill eye drops punctal occlusion for glaucoma [Video.] YouTube. All rights reserved. Video used with permission. https://youtu.be/TLhnsABDtco ↵
- “DSC_2273.jpg” by British Columbia Institute of Technology is licensed under CC BY 4.0. Access for free at https://opentextbc.ca/clinicalskills/chapter/6-5-installing-eye-ear-and-nose-medications/ ↵
- Djupesland, P. G. (2012). Nasal drug delivery devices: Characteristics and performance in a clinical perspective - a review. Drug Delivery and Translational Research, 3, 42-62. https://doi.org/10.1007/s13346-012-0108-9 ↵
- “Administering-med-vaginally-appliator.png” by British Columbia Institute of Technology is licensed under CC BY 4.0. Access for free at https://opentextbc.ca/clinicalskills/chapter/6-4-rectal-and-vaginal-medications/ ↵
- This work is derivative of “RESIZED+SERIALIZED+1202-1.jpg” courtesy of the U.S.National Library of Medicine. This image is included on the basis of Fair Use. ↵
- This work is a derivative of “advair-diskus-spl-graphic-16.jpg” courtesy of the U.S.National Library of Medicine. This image is included on the basis of Fair Use. ↵
- “Ipratropium_Bromide_(1).JPG” by Intropin is licensed under CC BY-SA 3.0 ↵
- Ari, A., & Restrepo, R. D. (2012). Aerosol delivery device selection for spontaneously breathing patients: 2012. Respiratory Care, 57(4), 613-626. http://rc.rcjournal.com/content/respcare/57/4/613.full.pdf ↵
- "Spacer_for_MDI_inhalers_therapy" by Ashashyou is licensed under CC BY-SA 3.0 ↵
- Ari, A., & Restrepo, R. D. (2012). Aerosol delivery device selection for spontaneously breathing patients: 2012. Respiratory Care, 57(4), 613-626. http://rc.rcjournal.com/content/respcare/57/4/613.full.pdf ↵
- Gregory, K. L., Wilken, L., & Hart, M. K. (2017). Pulmonary disease aerosol delivery devices: A guide for physicians, nurses, pharmacists, and other health care professionals (3rd ed.). American Association for Respiratory Care. https://www.aarc.org/wp-content/uploads/2018/03/aersol-guides-for-hcp.pdf ↵
- ARISE. (2016). Inhaler with spacer MVI_7500-ARISE.mp4 [Video]. Licensed under CC BY 3.0. https://youtu.be/-qNySzIGHWQ ↵
Medications administered via the skin or mucous membranes for direct local action, as well as for systemic effects.
A medication that is massaged or rubbed into the skin.
Patches or disks applied to the skin that deliver medication over an extended period of time.
An inhaler that provides a mist of medication that is inhaled through the mouth into the lungs.
An inhaler with medication provided in a powder form that is inhaled from the mouth into the lungs using a quick breath to activate the medication and move it into the lungs.
Devices that provide a fine mist using oxygen or compressed air to transport the medication from a nebulizer cup into the mouth and into the lungs as the patient breathes normally through a mask or pipe device

