14.4 Integumentary Assessment
Now that we have reviewed the anatomy of the integumentary system and common integumentary conditions, let’s review the components of an integumentary assessment. The standard for documentation of skin assessment is within 24 hours of admission to inpatient care. Skin assessment should also be ongoing in inpatient and long-term care.[1]
A routine integumentary assessment by a registered nurse in an inpatient care setting typically includes inspecting overall skin color, inspecting for skin lesions and wounds, and palpating extremities for edema, temperature, and capillary refill.[2]
Subjective Assessment
Begin the assessment by asking focused interview questions regarding the integumentary system. Itching is the most frequent complaint related to the integumentary system. See Table 14.4a for sample interview questions.
Table 14.4a Focused Interview Questions for the Integumentary System
| Questions | Follow-up |
|---|---|
| Are you currently experiencing any skin symptoms such as itching, rashes, or an unusual mole, lump, bump, or nodule?[3] | Use the PQRSTU method to gain additional information about current symptoms. Read more about the PQRSTU method in the “Health History” chapter. |
| Have you ever been diagnosed with a condition such as acne, eczema, skin cancer, pressure injuries, jaundice, edema, or lymphedema? | Please describe. |
| Are you currently using any prescription or over-the-counter medications, creams, vitamins, or supplements to treat a skin, hair, or nail condition? | Please describe. |
Objective Assessment
There are five key areas to note during a focused integumentary assessment: color, skin temperature, moisture level, skin turgor, and any lesions or skin breakdown. Certain body areas require particular observation because they are more prone to pressure injuries, such as bony prominences, skin folds, perineum, between digits of the hands and feet, and under any medical device that can be removed during routine daily care.[4]
Inspection
Color
Inspect the color of the patient’s skin and compare findings to what is expected for their skin tone. Note a change in color such as pallor (paleness), cyanosis (blueness), jaundice (yellowness), or erythema (redness). Note if there is any bruising (ecchymosis) present.
Scalp
If the patient reports itching of the scalp, inspect the scalp for lice and/or nits.
Lesions and Skin Breakdown
Note any lesions, skin breakdown, or unusual findings, such as rashes, petechiae, unusual moles, or burns. Be aware that unusual patterns of bruising or burns can be signs of abuse that warrant further investigation and reporting according to agency policy and state regulations.
Auscultation
Auscultation does not occur during a focused integumentary exam.
Palpation
Palpation of the skin includes assessing temperature, moisture, texture, skin turgor, capillary refill, and edema. If erythema or rashes are present, it is helpful to apply pressure with a gloved finger to further assess for blanching (whitening with pressure).
Temperature, Moisture, and Texture
Fever, decreased perfusion of the extremities, and local inflammation in tissues can cause changes in skin temperature. For example, a fever can cause a patient’s skin to feel warm and sweaty (diaphoretic). Decreased perfusion of the extremities can cause the patient’s hands and feet to feel cool, whereas local tissue infection or inflammation can make the localized area feel warmer than the surrounding skin. Research has shown that experienced practitioners can palpate skin temperature accurately and detect differences as small as 1 to 2 degrees Celsius. For accurate palpation of skin temperature, do not hold anything warm or cold in your hands for several minutes prior to palpation. Use the palmar surface of your dominant hand to assess temperature.[5] While assessing skin temperature, also assess if the skin feels dry or moist and the texture of the skin. Skin that appears or feels sweaty is referred to as being diaphoretic.
Capillary Refill
The capillary refill test is a test done on the nail beds to monitor perfusion, the amount of blood flow to tissue. Pressure is applied to a fingernail or toenail until it turns white, indicating that the blood has been forced from the tissue under the nail. This whiteness is called blanching. Once the tissue has blanched, remove pressure. Capillary refill is defined as the time it takes for color to return to the tissue after pressure has been removed that caused blanching. If there is sufficient blood flow to the area, a pink color should return within 2 seconds after the pressure is removed.[6]
View the Cardiovascular Assessment Part Two | Capillary Refill Test YouTube video for a demonstration of capillary refill.[7]
Skin Turgor
Skin turgor may be included when assessing a patient’s hydration status, but research has shown it is not a good indicator. Skin turgor is the skin’s elasticity. Its ability to change shape and return to normal may be decreased when the patient is dehydrated. To check for skin turgor, gently grasp skin on the patient’s lower arm between two fingers so that it is tented upwards, and then release. Skin with normal turgor snaps rapidly back to its normal position, but skin with poor turgor takes additional time to return to its normal position.[8] Skin turgor is not a reliable method to assess for dehydration in older adults because they have decreased skin elasticity, so other assessments for dehydration should be included.[9]
Edema
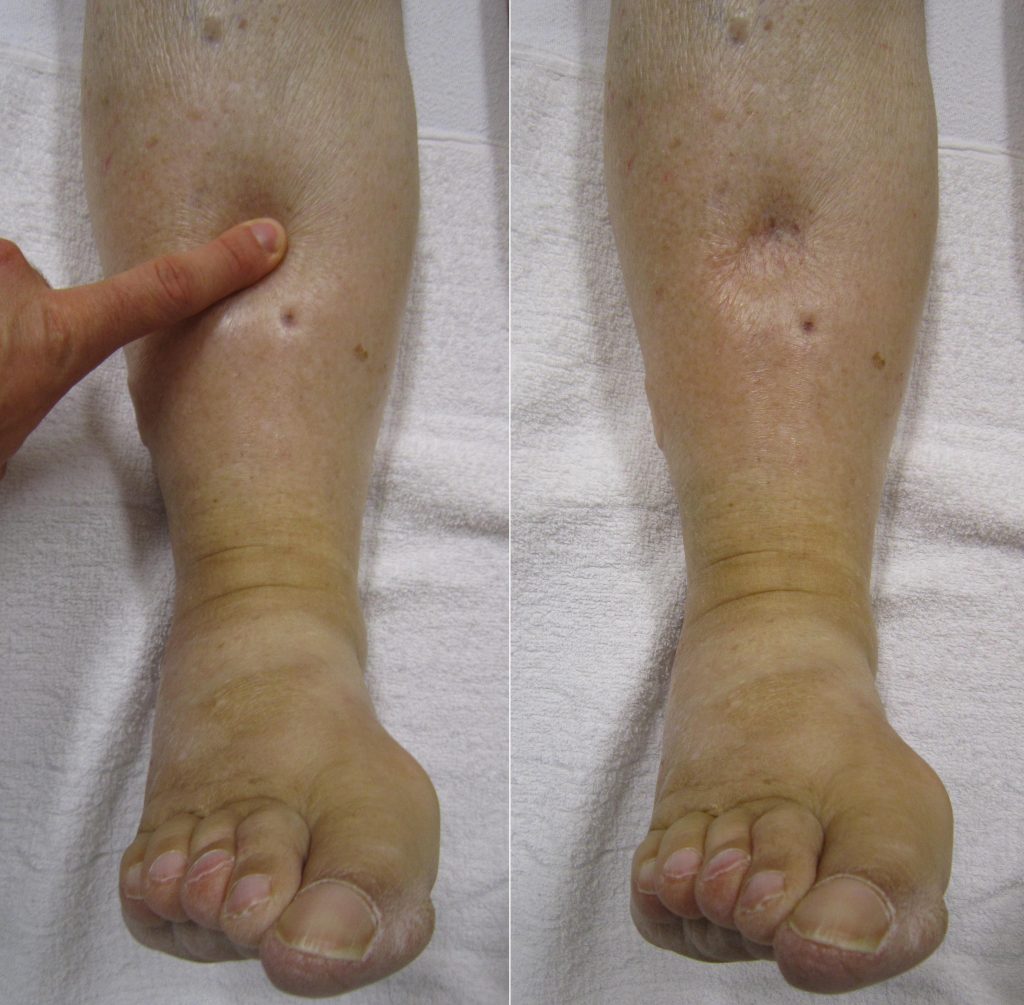
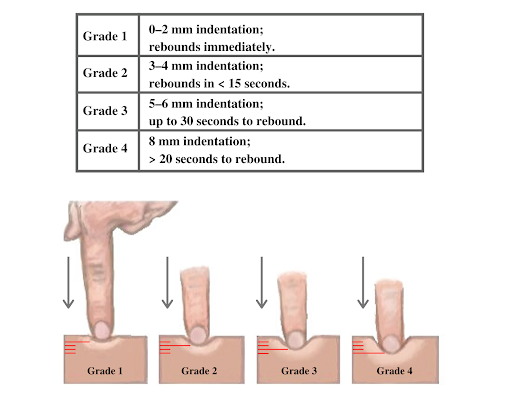
If edema is present on inspection, palpate the area to determine if the edema is pitting or nonpitting. Press on the skin to assess for indentation, ideally over a bony structure, such as the tibia. If no indentation occurs, it is referred to as nonpitting edema. If indentation occurs, it is referred to as pitting edema. See Figure 14.22[10] for an image demonstrating pitting edema. If pitting edema is present, document the depth of the indention and how long it takes for the skin to rebound back to its original position. The indentation and time required to rebound to the original position are graded on a scale from 1 to 4, where 1+ indicates a barely detectable depression with immediate rebound, and 4+ indicates a deep depression with a time lapse of over 20 seconds required to rebound. See Figure 14.23[11] for an illustration of grading edema.
Life Span Considerations
Older Adults
Older adults have several changes associated with aging that are apparent during assessment of the integumentary system. They often have cardiac and circulatory system conditions that cause decreased perfusion, resulting in cool hands and feet. They have decreased elasticity and fragile skin that often tears more easily. The blood vessels of the dermis become more fragile, leading to bruising and bleeding under the skin. The subcutaneous fat layer thins, so it has less insulation and padding and reduced ability to maintain body temperature. Growths such as skin tags, rough patches (keratoses), skin cancers, and other lesions are more common. Older adults may also be less able to sense touch, pressure, vibration, heat, and cold.[12]
When completing an integumentary assessment, it is important to distinguish between expected and unexpected assessment findings. Please review Table 14.4b to review common expected and unexpected integumentary findings.
Table 14.4b Expected Versus Unexpected Findings on Integumentary Assessment
| Assessment | Expected Findings | Unexpected Findings (Document and notify provider if it is a new finding*) |
|---|---|---|
| Inspection | Skin is expected color for ethnicity without lesions or rashes. | Jaundice
Erythema Cyanosis Irregular-looking mole Bruising (ecchymosis) Rashes Petechiae Skin breakdown Burns |
| Auscultation | Not applicable | |
| Palpation | Skin is warm and dry with no edema. Capillary refill is less than 3 seconds. Skin has normal turgor with no tenting. | Diaphoretic or clammy
Cool extremity Edema Lymphedema Capillary refill greater than 3 seconds Tenting |
| *CRITICAL CONDITIONS to report immediately | Cool and clammy
Diaphoretic Petechiae Jaundice Cyanosis Redness, warmth, and tenderness indicating a possible infection |
- Medline Industries, Inc. (n.d.). Are you doing comprehensive skin assessments correctly? Get the whole picture. https://www.medline.com/skin-health/comprehensive-skin-assessments-correctly-get-whole-picture/#:~:text=A%20comprehensive%20skin%20assessment%20entails,actually%20more%20than%20skin%20deep ↵
- Giddens, J. F. (2007). A survey of physical examination techniques performed by RNs: Lessons for nursing education. Journal of Nursing Education, 46(2), 83-87. https://doi.org/10.3928/01484834-20070201-09 ↵
- McKay, M. (1990). The dermatologic history. In Walker, H. K., Hall, W. D., Hurst, J. W. (Eds.), Clinical methods: The history, physical, and laboratory examinations (3rd ed.). https://www.ncbi.nlm.nih.gov/books/NBK207/ ↵
- Medline Industries, Inc. (n.d.). Are you doing comprehensive skin assessments correctly? Get the whole picture. https://www.medline.com/skin-health/comprehensive-skin-assessments-correctly-get-whole-picture/#:~:text=A%20comprehensive%20skin%20assessment%20entails,actually%20more%20than%20skin%20deep ↵
- Levine, D., Walker, J. R., Marcellin-Little, D. J., Goulet, R., & Ru, H. (2018). Detection of skin temperature differences using palpation by manual physical therapists and lay individuals. The Journal of Manual & Manipulative Therapy, 26(2), 97-101. https://dx.doi.org/10.1080%2F10669817.2018.1427908 ↵
- Johannsen, L.L. (2005). Skin assessment. Dermatology Nursing, 17(2), 165-66. ↵
- Nurse Saria. (2018, September 18). Cardiovascular assessment part two | Capillary refill test [Video]. YouTube. All rights reserved. https://youtu.be/A6htMxo4Cks ↵
- A.D.A.M. Medical Encyclopedia [Internet]. Atlanta (GA): A.D.A.M., Inc.; c1997-2020. Skin turgor; [updated 2020, Sep 16; cited 2020, Sep 18]. https://medlineplus.gov/ency/article/003281.htm#:~:text=To%20check%20for%20skin%20turgor,back%20to%20its%20normal%20position ↵
- Nursing Times. (2015, August 3). Detecting dehydration in older people. https://www.nursingtimes.net/roles/older-people-nurses-roles/detecting-dehydration-in-older-people-useful-tests-03-08-2015/ ↵
- “Combinpedal.jpg” by James Heilman, MD is licensed under CC BY-SA 3.0 ↵
- “Grading of Edema” by Meredith Pomietlo for Chippewa Valley Technical College is licensed under CC BY 4.0 ↵
- A.D.A.M. Medical Encyclopedia [Internet]. Atlanta (GA): A.D.A.M., Inc.; c1997-2020. Aging changes in skin; [updated 2020, Sep 16; cited 2020, Sep 18]. https://medlineplus.gov/ency/article/004014.htm#:~:text=The%20remaining%20melanocytes%20increase%20in,the%20skin's%20strength%20and%20elasticity ↵
A reduced amount of oxyhemoglobin the skin or mucous membranes. Skin and mucous membranes present with a pale skin color.
A bluish discoloration of the skin, lips, and nail beds. It is an indication of decreased perfusion and oxygenation.
A yellowing of the skin or sclera caused by underlying medical conditions.
A red color of the skin.
Bruising.
The whiteness that occurs when pressure is placed on tissue or a nailbed, causing blood to leave the area.
Excessive, abnormal sweating.
The skin's elasticity and its ability to change shape and return to normal when gently grasped between two fingers.

