5.3 Safety Strategies
Open Resources for Nursing (Open RN)
Safety strategies have been developed based on research to reduce the likelihood of errors and to create safe standards of care. Examples of safety initiatives include strategies to prevent medication errors, standardized checklists, and structured team communication tools.
Medication Errors
Several initiatives have been developed nationally to prevent medication errors, such as the establishment of a “Do Not Use List of Abbreviations,” a “List of Error-Prone Abbreviations,” “Frequently Confused Medication List,” “High-Alert Medications List,” and the “Do Not Crush List.” Additionally, it is considered a standard of care for nurses to perform three checks of the rights of medication administration whenever administering medication. View more information about these safety initiatives to prevent medication errors in the box below. Specific strategies to prevent medication errors are discussed in the “Preventing Medication Errors” of the “Legal/Ethical” chapter of the Open RN Nursing Pharmacology, 2e textbook. The rights of medication administration are discussed in the “Basic Concepts of Administering Medications” section of the “Administration of Enteral Medications” chapter of the Open RN Nursing Skills, 2e textbook.
Read more about safety initiatives implemented to prevent medication errors:
Checklists
Performance of complex medical procedures is often based on memory, even though humans are prone to short-term memory loss, especially when we are multitasking or under stress. The point-of-care checklist is an example of a patient care safety initiative that reduces this reliance on fallible memory. For example, a surgical checklist developed by the World Health Organization (WHO) has been adopted by most surgical providers around the world as a standard of care. It has significantly decreased injuries and deaths caused by surgeries by focusing on teamwork and communication. The Association of PeriOperative Registered Nurses (AORN) combined recommendations from The Joint Commission and the WHO to create a specific surgical checklist for nurses. See Figure 5.2[1] for an image of the WHO surgical checklist.
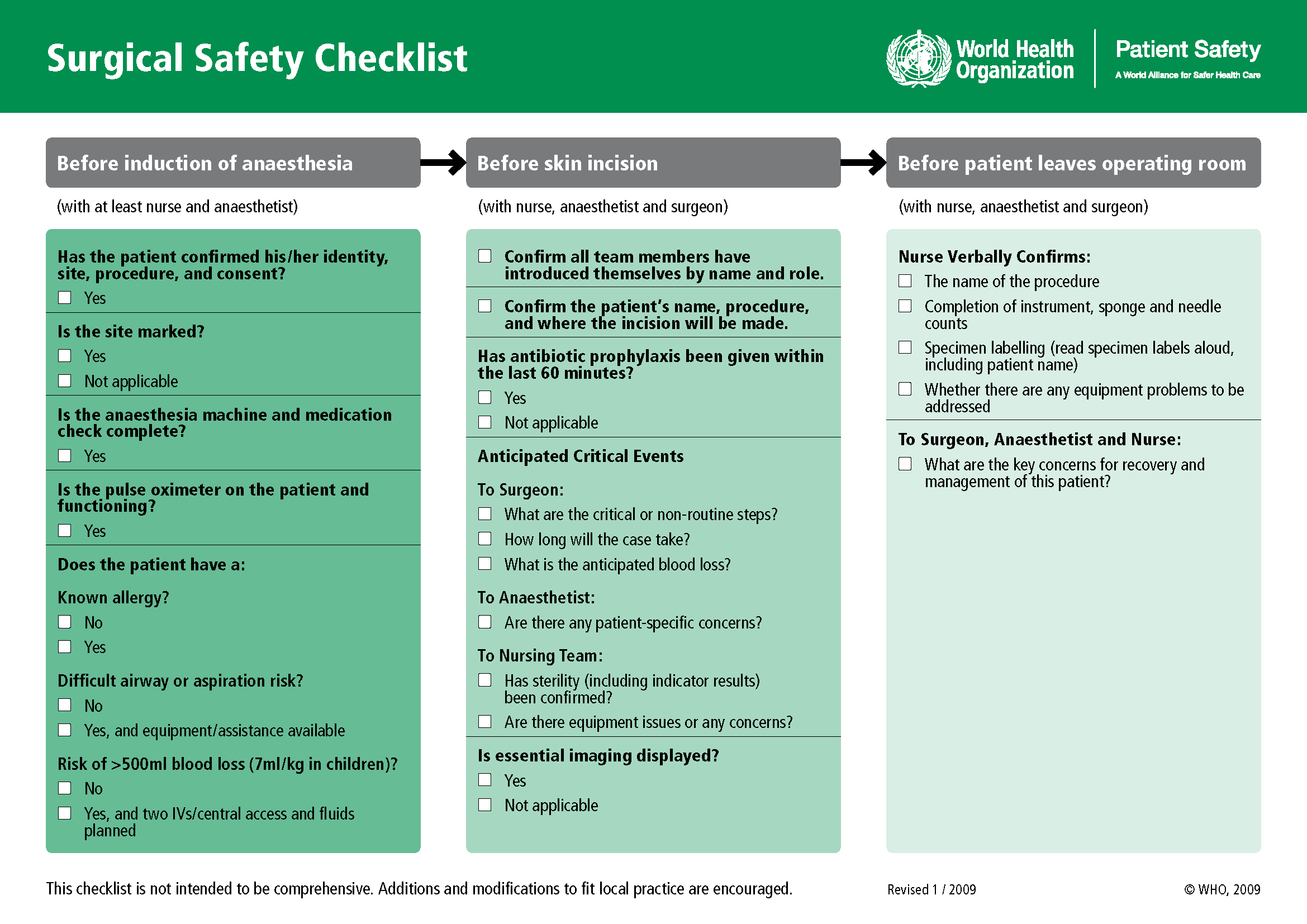
View an example of a Preop Checklist in the “Preoperative Care” section of the “Perioperative” chapter of Open RN Nursing Health Alterations.
Team Communication
Nurses routinely communicate with multidisciplinary health care team members and contact health care providers to report changes in patient status. Serious patient harm can occur when patient information is absent, incomplete, erroneous, or delayed during team communication. Standardized methods of communication are used to ensure that accurate information is exchanged among team members in a structured and concise manner, such as ISBARR reports and handoff reports.
ISBARR is a mnemonic for the components of Introduction, Situation, Background, Assessment, Request/Recommendations, and Repeat back. See Figure 5.3[2] for an image of an ISBARR reference card.
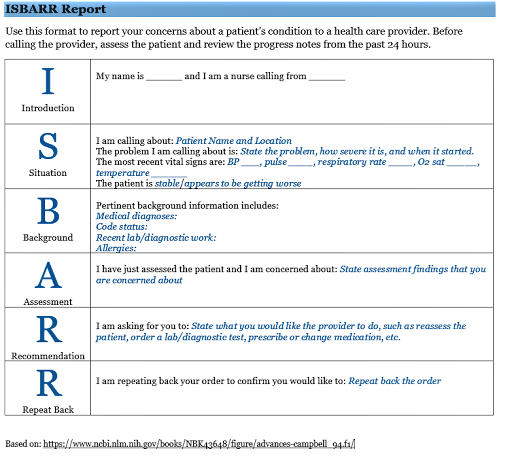

Handoff reports are a specific type of team communication as patient care is transferred. Handoff reports are defined by The Joint Commission as, “A transfer and acceptance of patient care responsibility achieved through effective communication. It is a real-time process of passing patient specific information from one caregiver to another, or from one team of caregivers to another, for the purpose of ensuring the continuity and safety of the patient’s care.”[3]
Review information about ISBARR and handoff reports in Chapter 2.4.
- “9789241598590_eng_Checklist.pdf” by WHO is in the Public Domain ↵
- “ISBARR Reference Card” by Kim Ernstmeyer at Chippewa Valley Technical College is licensed under CC BY 4.0 ↵
- The Joint Commission. (2017). Sentinel Event Alert: Inadequate Handoff Communication. https://www.jointcommission.org/-/media/tjc/documents/resources/patient-safety-topics/sentinel-event/sea_58_hand_off_comms_9_6_17_final_(1).pd ↵
A mnemonic for the format of professional communication among health care team members that includes Introduction, Situation, Background, Assessment, Request/Recommendations, and Repeat back.
A transfer and acceptance of patient care responsibility achieved through effective communication. It is a real-time process of passing patient specific information from one caregiver to another, or from one team of caregivers to another, for the purpose of ensuring the continuity and safety of the patient’s care.

