3.8 Culturally Responsive Care
Open Resources for Nursing (Open RN)
After establishing a culturally sensitive environment and performing a cultural assessment, nurses and nursing students can continue to promote culturally responsive care. Culturally responsive care includes creating a culturally safe environment, using cultural negotiation, and considering the impact of culture on patients’ time orientation, space orientation, eye contact, and food choices.
Culturally Safe Environment
A primary responsibility of the nurse is to ensure the environment is culturally safe for the patient. A culturally safe environment is a safe space for patients to interact with the nurse, without judgment or discrimination, where the patient is free to express their cultural beliefs, values, and identity. This responsibility belongs to both the individual nurse and also to the larger health care organization.
Cultural Negotiation
Many aspects of nursing care are influenced by the patient’s cultural beliefs, as well as the beliefs of the health care culture. For example, the health care culture in the United States places great importance on punctuality for medical appointments, yet a patient may belong to a culture that views “being on time” as relative. In some cultures, time is determined simply by whether it is day or night or time to wake up, eat, or sleep. Making allowances or accommodations for these aspects of a patient’s culture is instrumental in fostering the nurse-patient relationship. This accommodation is referred to as cultural negotiation. See Figure 3.6[1] for an image illustrating cultural negotiation. During cultural negotiation, both the patient and nurse seek a mutually acceptable way to deal with competing interests of nursing care, prescribed medical care, and the patient’s cultural needs. Cultural negotiation is reciprocal and collaborative. When a patient’s cultural needs do not significantly or adversely affect their treatment plan, their cultural needs should be accommodated when feasible.
As an example, think about the patient previously discussed for whom a fixed schedule is at odds with their cultural views. Instead of teaching the patient to take a daily medication at a scheduled time, the nurse could explain that the patient should take the medication every day when he awakens rather than every morning at 0800. Another example of cultural negotiation is illustrated by a scenario in which the nurse is preparing a patient for a surgical procedure. As the nurse goes over the preoperative checklist, the nurse asks the patient to remove her head covering (hijab). The nurse is aware that personal items should be removed before surgery; however, the patient wishes to keep on the hijab. As an act of cultural negotiation and respect for the patient’s cultural beliefs, the nurse makes arrangements with the surgical team to keep the patient’s hijab in place for the surgical procedure and covering the patient’s hijab with a surgical cap.

Decision-Making
Health care culture in the United States mirrors cultural norms of the country, with an emphasis on individuality, personal freedom, and self-determination. Self-determination refers to a person’s right to determine what will be done with and to their own body. This perspective may conflict with a patient whose cultural background values group decision-making and decisions made to benefit the group, not necessarily the individual. As an example, in the 2019 film The Farewell, a Chinese-American family decides to not tell the family matriarch she is dying of cancer and only has a few months left to live. The family keeps this secret from the woman in the belief that the family should bear the emotional burden of this knowledge, which is a collectivistic viewpoint in contrast to American individualistic viewpoint.
Space Orientation
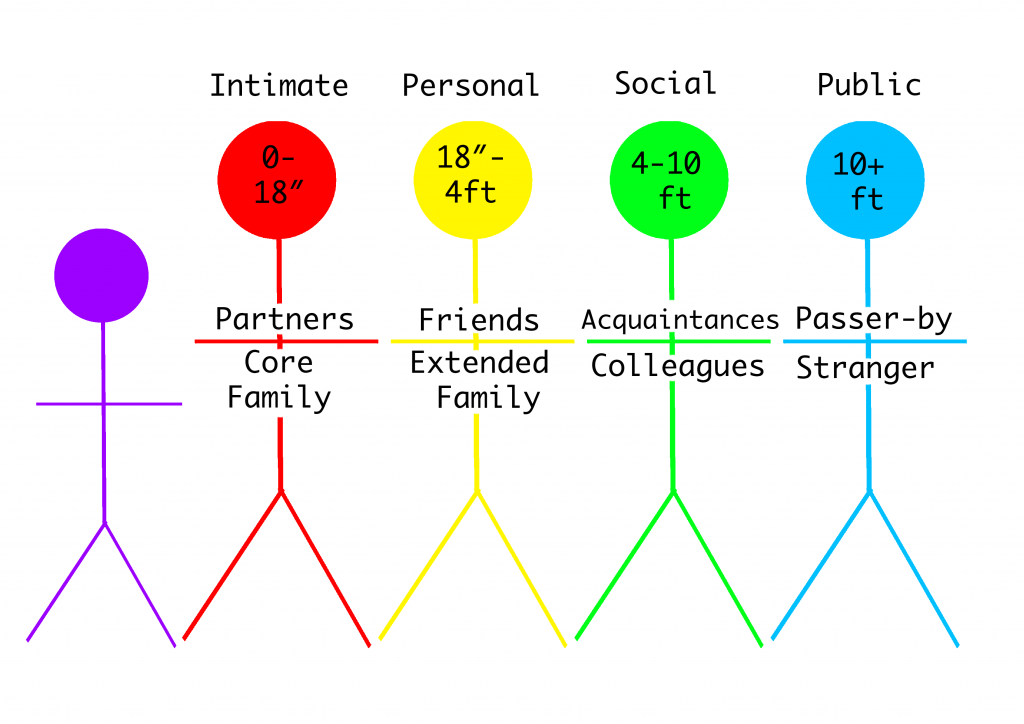
The amount of space that a person surrounds themselves with to feel comfortable is influenced by culture. See Figure 3.7[2] for an image illustrating space orientation. For example, for some people, it would feel awkward to stand four inches away from another person while holding a social conversation, but for others a small personal space is expected when conversing with another.[3] There are times when a nurse must enter a patient’s intimate or personal space, which can cause emotional distress for some patients. The nurse should always ask for permission before entering a patient’s personal space and explain why close contact is necessary and what is about to happen.
Patients may also be concerned about their modesty or being exposed. A patient may deal with the violation of their space by removing themselves from the situation, pulling away, or closing their eyes. The nurse should recognize these cues for what they are, an expression of cultural preference, and allow the patient to assume a position or distance that is comfortable for them.
Similar to cultural influences on personal space, touch is also culturally determined. This has implications for nurses because depending on the culture, it may be inappropriate for a male nurse to provide care for a female patient and vice versa. In some cultures, it is also considered rude to touch a person’s head without permission.
Review more information about space orientation in the “Communication” chapter.
Eye Contact
Eye contact is also a culturally mediated behavior. See Figure 3.8[4] for an image of eye contact. In the United States, direct eye contact is valued when communicating with others, but in some cultures, direct eye contact is interpreted as being rude or bold. Rather than making direct eye contact, a patient may avert their eyes or look down at the floor to show deference and respect to the person who is speaking. The nurse should notice these cultural cues from the patient and mirror the patient’s behaviors when possible.
Food Choices
Culture plays a meaningful role in the dietary practices and food choices of many people. Food is used to celebrate life events and holidays. Most cultures have staple foods, such as bread, pasta, or rice and particular ways of preparing foods. See Figure 3.9[5] for an image of various food choices. Special foods are prepared to heal and to cure or to demonstrate kinship, caring, and love. For example, in the United States, chicken noodle soup is often prepared and provided to family members who are ill. In certain Asian cultures, individuals prefer “heating” or “cooling” foods depending on the illness, with the belief that each specific food will help bring balance back to their system.[6] Additionally, certain foods and beverages (such as meat and alcohol) are forbidden in some cultures. Nurses should accommodate or negotiate dietary requests of their patients, knowing that food holds such an important meaning to many people.

Summary
In summary, there are several steps in the journey of becoming a culturally competent nurse with cultural humility who provides culturally responsive care to patients. As you continue in your journey of developing cultural competency, keep the summarized points in the following box in mind.
Summary of Developing Cultural Competency
- Cultural competence is an ongoing process for nurses and takes dedication, time, and practice to develop.
- Pursuing the goal of cultural competence in nursing and other health care disciplines is a key strategy in reducing health care disparities.
- Culturally competent nurses recognize that culture functions as a source of values and comfort for patients, their families, and communities.
- Culturally competent nurses intentionally provide patient-centered care with sensitivity and respect for culturally diverse populations.
- Misunderstandings, prejudices, and biases on the part of the health care provider interfere with the patient’s health outcomes.
- Culturally competent nurses negotiate care with clients so the care is congruent with their cultural beliefs and values.
- Nurses should examine their own biases, ethnocentric views, and prejudices so as not to interfere with the patient’s care.
- Nurses who respect and understand the cultural values and beliefs of their patients are more likely to develop positive, trusting relationships with their patients.
- “handshake-3378251_1920.jpg” by geralt is licensed under CC0 ↵
- “Proxemics.png” by Natbrock Alicia Tom is licensed under CC BY-SA 3.0 ↵
- Kreuz, R., & Roberts, R. (2019). Proxemics 101: Understanding personal space across cultures. The MITPress Reader. https://thereader.mitpress.mit.edu/understanding-personal-space-proxemics/ ↵
- “271509.png” by amcolley is in the Public Domain ↵
- “wanna-cuppa-singapore-cafe-food-bistro-trees-dishes-craft-beer-ale-breakfast-lunch-dinner-dark-1920x1080.jpg” by Jennette Kwok is licensed under CC BY-NC-SA 4.0 ↵
- College of Naturopathy Medicine. (n.d.). The energy of foods in Chinese medicine. https://www.naturopathy-uk.com/news/news-cnm-blog/blog/2020/07/16/the-energy-of-foods-in-chinese-medicine/ ↵
A safe space for patients to interact with health professionals, without judgment or discrimination, where the patient is free to express their cultural beliefs, values, and identity.
A process where the patient and nurse seek a mutually acceptable way to deal with competing interests of nursing care, prescribed medical care, and the patient’s cultural needs.

