10.3 Wounds
Open Resources for Nursing (Open RN)
Phases of Wound Healing
When skin is injured, there are four phases of wound healing that take place: hemostasis, inflammatory, proliferative, and maturation. See Figure 10.10[1] for an illustration of wound healing demonstrating hemostasis/inflammation, proliferation, and maturation.
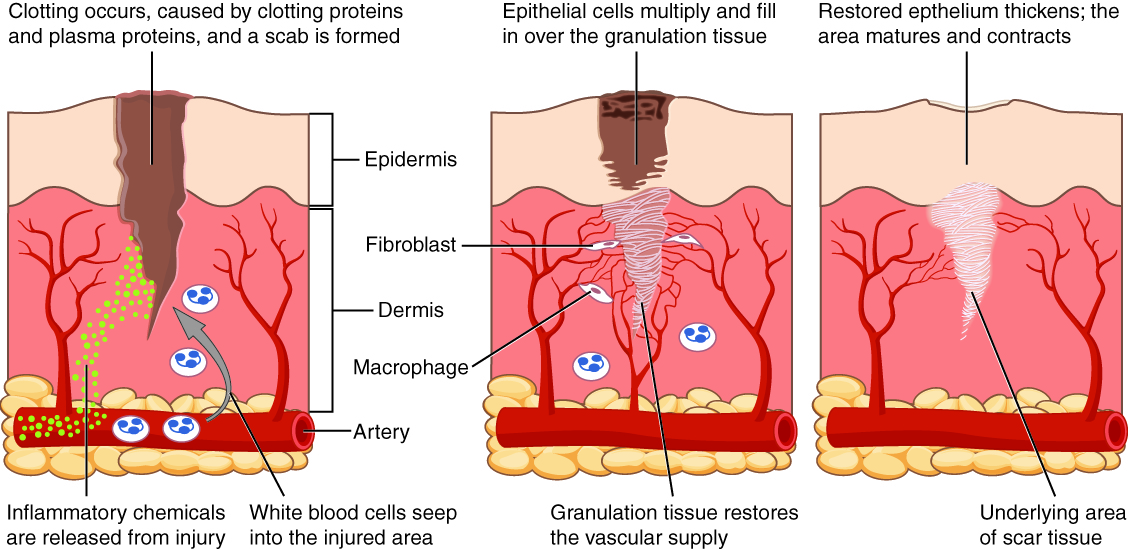
To illustrate the phases of wound healing, imagine that you accidentally cut your finger with a knife as you were slicing an apple for a snack. Immediately after the injury occurs, blood vessels constrict and clotting factors are activated. This is referred to as the hemostasis phase. Clotting factors are released to form clots and to stop the bleeding. Platelets release growth factors that alert various cells to start the repair process at the wound location. The hemostasis phase lasts up to 60 minutes, depending on the severity of the injury.[2],[3]
After the hemostasis phase, the inflammatory phase begins. Vasodilation occurs so that white blood cells in the bloodstream can move to the location of the wound and start cleaning the wound bed. The inflammatory process appears as edema (swelling), erythema (redness), and exudate. Exudate is fluid that oozes out of a wound, such as pus or other drainage.[4],[5]
The proliferative phase of wound healing begins within a few days after the injury and includes four important processes: epithelialization, angiogenesis, collagen formation, and contraction. Epithelialization refers to the development of new epidermis and granulation tissue. Granulation tissue is new connective tissue with new, fragile, thin-walled capillaries. Collagen is also formed to provide strength and integrity to the wound. At the end of the proliferation phase, the wound begins to contract in size.[6],[7]
Capillaries begin to develop within the wound 24 hours after injury during a process called angiogenesis. These capillaries bring more oxygen and nutrients to the wound for healing. When performing dressing changes, it is essential for the nurse to protect this granulation tissue and the associated new capillaries. Healthy granulation tissue appears pink due to the new capillary formation. It is moist, painless to the touch, and may appear “bumpy.” Conversely, unhealthy granulation tissue is dark red and painful. It bleeds easily with minimal contact and may be covered by shiny white or yellow fibrous tissue, referred to as biofilm, that impairs healing and should be removed by a trained health care provider. Unhealthy granulation tissue is often caused by an infection, so wound cultures should be obtained when infection is suspected.[8]
During the maturation phase, collagen continues to be created to strengthen the wound. Collagen contributes strength to the wound to prevent it from reopening. A wound typically heals within 4-5 weeks and often leaves behind a scar. The scar tissue is initially firm, red, and slightly raised from the excess collagen deposition. In roughly nine months, the scar begins to soften, flatten, and become pale.[9],[10]
Types of Wound Healing
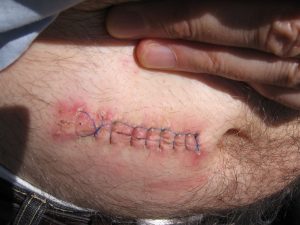
There are three types of wound healing: primary intention, secondary intention, and tertiary intention. Healing by primary intention means that the wound is sutured, stapled, glued, or otherwise closed so the wound heals beneath the closure. This type of healing occurs with clean-edged lacerations or surgical incisions, and the closed edges are referred to as approximated. See Figure 10.11[11] for an image of a surgical wound healing by primary intention with approximated edges.
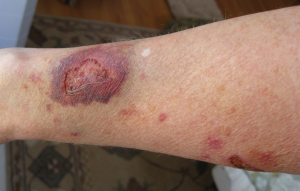
Secondary intention occurs when the edges of a wound cannot be approximated (brought together), so the wound heals by filling in from the bottom up with the production of granulation tissue. Examples of common wounds that heal by secondary intention are pressure injuries and skin tears. Wounds that heal by secondary infection are at higher risk for infection and must be protected from contamination. See Figure 10.12[12] for an image of a wound that if left untreated, would heal by secondary intention.
Tertiary intention refers to the healing of a wound that has had to remain open or has been reopened, often due to severe infection or swelling. The wound is typically closed at a later date when infection or swelling has resolved. Wounds that heal by secondary and tertiary intention have delayed healing times and increased risk for infection and scar tissue.
Types of Wounds
There are many common types of wounds that nurses care for, such as skin tears, venous ulcers, arterial ulcers, diabetic ulcers, and pressure injuries.
Wound Care
Wound care includes assessing and cleansing wounds, performing dressing changes, and implementing interventions to promote wound healing. Assessing wounds and implementing interventions to promote wound healing are further discussed in the “Applying the Nursing Process” section later in this chapter.
- “417 Tissue Repair.jpg” by OpenStax is licensed under CC BY 3.0. Access for free at https://openstax.org/books/anatomy-and-physiology/pages/1-introduction ↵
- Doyle, G. R., & McCutcheon, J. A. (2015). Clinical Procedures for Safer Patient Care. BCcampus. https://opentextbc.ca/clinicalskills/front-matter/introduction/ ↵
- Grubbs, H. (2023). Wound physiology. StatPearls [Internet]. https://www.ncbi.nlm.nih.gov/books/NBK518964/ ↵
- Doyle, G. R., & McCutcheon, J. A. (2015). Clinical Procedures for Safer Patient Care. BCcampus. https://opentextbc.ca/clinicalskills/front-matter/introduction/ ↵
- Grubbs, H. (2023). Wound physiology. StatPearls [Internet]. https://www.ncbi.nlm.nih.gov/books/NBK518964/ ↵
- Doyle, G. R., & McCutcheon, J. A. (2015). Clinical Procedures for Safer Patient Care. BCcampus. https://opentextbc.ca/clinicalskills/front-matter/introduction/ ↵
- Grubbs, H. (2023). Wound physiology. StatPearls [Internet]. https://www.ncbi.nlm.nih.gov/books/NBK518964/ ↵
- McKay, M. (1990). The dermatologic history. In Walker, H. K., Hall, W. D., Hurst, J. W. (Eds.), Clinical methods: The history, physical, and laboratory examinations (3rd ed.). https://www.ncbi.nlm.nih.gov/books/NBK207/ ↵
- Doyle, G. R., & McCutcheon, J. A. (2015). Clinical Procedures for Safer Patient Care. BCcampus. https://opentextbc.ca/clinicalskills/front-matter/introduction/ ↵
- Grubbs, H. (2023). Wound physiology. StatPearls [Internet]. https://www.ncbi.nlm.nih.gov/books/NBK518964/ ↵
- “Ventriculoperitoneal shunt - surgical wound healing - belly - day 12.jpg” by Hansmuller is licensed under CC BY-SA 4.0 ↵
- “Atrophied skin.png” by sansea2 is licensed under CC BY-SA 3.0 ↵
The first stage of wound healing when clotting factors are released to form clots to stop the bleeding.
The second stage of healing when vasodilation occurs to move white blood cells into the wound to start cleaning the wound bed.
Swelling.
Redness.
Fluid that oozes from a wound.
The third stage of wound healing that begins a few days after injury and includes four processes: epithelialization, angiogenesis, collagen formation, and contraction.
The development of new epidermis and granulation tissue in a healing wound.
New connective tissue in a healing wound with new, fragile, thin-walled capillaries.
The process of wound healing when new capillaries begin to develop within the wound 24 hours after injury to bring in more oxygen and nutrients for healing.
The final stage of wound healing when collagen continues to be created to strengthen the wound and prevent it from reopening.
A type of wound that is sutured, stapled, glued, or otherwise closed so the wound heals beneath the closure.
The well-closed edges of a wound healing by primary intention.
A type of healing that occurs when the edges of a wound cannot be brought together, so the wound fills in from the bottom up by the production of granulation tissue. An example of a wound healing by secondary intention is a pressure injury.
The healing of a wound that has had to remain open or has been reopened, often due to severe infection.

