16.2 Basic Concepts
Open Resources for Nursing (Open RN)
Let’s begin by reviewing the basic anatomy and physiology of the urinary and gastrointestinal systems.
Urinary System
The urinary system, also referred to as the renal system or urinary tract, consists of the kidneys, ureters, bladder, and urethra. The purpose of the urinary system is to eliminate waste from the body, regulate blood volume and blood pressure, control levels of electrolytes and metabolites, and regulate blood pH. The kidneys filter blood in the nephrons and remove waste in the form of urine. Urine exits the kidney via the ureters and enters the urinary bladder, where it is stored until it is expelled by urination (also referred to as voiding).[1] See Figure 16.1[2] for an image of the male urinary system. The female urinary system is similar except for a smaller urethra.
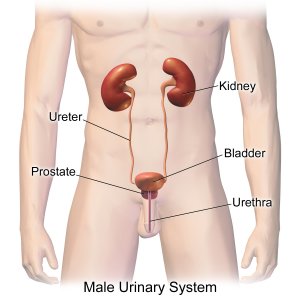
A healthy adult with normal kidney function produces 800-2,000 mL of urine per day, depending on fluid intake, as well as the amount of fluid lost through sweating and breathing. The bladder typically holds about 360-480 mL of urine. As the bladder fills, it sends signals to the brain that it is time to urinate. The urinary tract includes two sets of muscles that work together as a sphincter, closing off the urethra to keep urine in the bladder until the brain sends signals to urinate. Urination occurs when the brain sends signals to the wall of the bladder to contract and squeeze urine out of the bladder and through the urethra. Frequency of urination depends on how quickly the kidneys produce urine and how much urine a person’s bladder can comfortably hold.[3]
Normal urine should be clear, pale to light yellow in color, and not foul-smelling. However, some foods or medications may change the smell or color of urine. For instance, phenazopyridine (Pyridium), a common medication prescribed to treat the pain, frequency, and burning associated with urinary tract infections, can cause urine to appear orange.[4]
Nurses frequently monitor and document a client’s urine output as part of the overall plan of care. It can be collected by placing a collection hat in the client’s toilet and then measured in a graduated cylinder. If the client has an indwelling catheter, the urine is emptied every shift from the catheter bag and measured in a graduated cylinder. For infants and toddlers, the number of daily wet diapers provides a general measure of urine output. For more specific measurement of urine output during hospitalization, wet diapers are weighed.
Terms commonly used to document conditions related to the urinary tract are as follows:
- Anuria: Absence of urine output, typically found during kidney failure, defined as less than 50 mL of urine over a 24-hour period.
- Dysuria: Painful or difficult urination.
- Frequency: The need to urinate several times during the day or at night (nocturia) in normal or less-than-normal volumes. It may be accompanied by a feeling of urgency.[5]
- Hematuria: Blood in the urine, either visualized or found during microscopic analysis.
- Oliguria: Decreased urine output, defined as less than 500 mL of urine in adults in a 24-hour period. In hospitalized clients, oliguria is further defined as less than 0.5 mL of urine per kilogram per hour for adults and children or less than 1 mL of urine per kilogram per hour for infants.[6] New oliguria should be reported to the health care provider because it can indicate dehydration, fluid retention, or decreasing kidney function.
- Nocturia: The need to get up at night on a regular basis to urinate. Nocturia often causes sleep deprivation that affects a person’s quality of life.[7]
- Polyuria: Greater than 2.5 liters of urine output over 24 hours, also referred to as diuresis. Urine is typically clear with no color.[8] New polyuria should be reported to the health care provider because it can be a sign of many medical conditions.
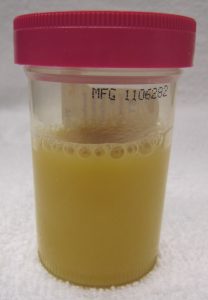
- Pyuria: At least ten white blood cells in each cubic millimeter of urine in a urine sample, typically indicating infection. In severe infections, pus may be visible in the urine.[9] See Figure 16.2[10] for an image of pyuria for a client with urosepsis.
- Urgency: A sensation of an urgent need to void.[11] Urgency can cause urge incontinence if the client is not able to reach the bathroom quickly.
View an activity reviewing the Vascular System of the Kidneys.
Gastrointestinal System
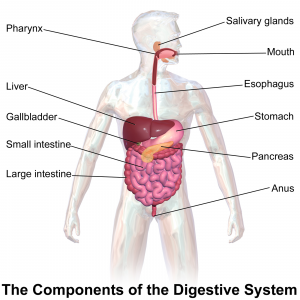
The gastrointestinal (GI) system includes the mouth, esophagus, stomach, small intestine, large intestine, and anus. See Figure 16.3[12] for an image of the gastrointestinal system. Ingested food and liquid are pushed through the GI tract by peristalsis, the involuntary contraction and relaxation of muscle creating wave-like movements of the intestines. The stomach mixes food and liquid with digestive enzymes and then empties into the small intestine. The muscles of the small intestine mix food with enzymes and bile from the pancreas, liver, and intestine and push the mixture forward for further digestion. Bacteria in the GI tract, called normal flora or microbiome, also assist with digestion. The walls of the small intestine absorb water and the digested nutrients into the bloodstream. As peristalsis continues, the waste products of the digestive process move into the large intestine. The large intestine absorbs water and changes the waste from liquid into stool. The rectum, at the lower end of the large intestine, stores stool until it is pushed out of the anus during a bowel movement.[13]
This section will focus on common alterations in bowel elimination, including constipation, diarrhea, and bowel incontinence. These alterations are common symptoms of several diseases and conditions of the gastrointestinal system. Nurses provide care to help manage these alterations.
Terms related to alterations in bowel elimination include the following:
- Black stools: Black-colored stools can be side effects of iron supplements or bismuth subsalicylate (Pepto-Bismol).
- Rectal bleeding: Rectal bleeding refers to bright red blood in the stools, also referred to as hematochezia. It is a sign of bleeding from the lower GI tract. Rectal bleeding can range in severity from minimal drops of blood on the toilet tissue caused by hemorrhoids to severe bleeding in large amounts that are life-threatening and require emergency care.[14] New bleeding should always be reported to the health care provider.
- Tarry stools: Stools that are black, sticky, and appear like tar are referred to as melena. Melena is typically caused by bleeding in the upper part of the gastrointestinal tract, such as the esophagus, stomach, or the first part of the small intestine, or due to the client swallowing blood. The blood appears darker and tarry-looking because it undergoes digestion on its way through the GI tract.[15] Bleeding from the upper part of the GI tract can also range from mild to life-threatening, depending upon the cause, and should always be reported to the health care provider.
Review information about digestion in the “Nutrition” chapter or read more information about the “Gastrointestinal” system in Open RN Nursing Pharmacology, 2e.
Newborns and Infants
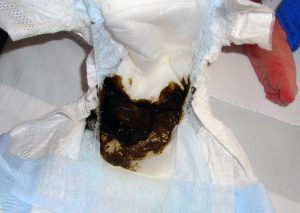
Meconium refers to the first bowel movement of a newborn that appears sticky and black to dark green in color. See Figure 16.4[16] for an image of meconium. The stool of a breastfed baby usually appears like a curdled yellow, while that of a formula-fed baby is pastier. Breastfed babies often have bowel movements after every feeding. Formula-fed babies tend to have fewer bowel movements.
Toddlers
Toddlers usually begin the process of toilet training between two and three years old. Enuresis is the term used to describe incontinence when sleeping (i.e., bed-wetting). Enuresis in children is considered normal unless it continues past seven or eight years of age, when it should be addressed with a pediatrician. Toddlers often have undigested food in their bowel movements due to the intestinal system not fully digesting some foods, such as corn or grapes.
Children
School-aged children may be at risk for developing constipation due to delaying bowel movements during school times until they are in the privacy of their homes. The longer the stool sits in the colon, the more water is absorbed by the intestines, and the harder stool becomes to pass.
Adults
Adult females often develop urinary incontinence related to pregnancy and delivery, menopause, or vaginal hysterectomy. Adult males may have urgency and urinary retention with possible overflow urinary incontinence as their prostate enlarges. Adults over the age of 30 may develop nocturia.
Older Adults
Peristalsis typically slows as aging occurs. Older adults should be encouraged to increase fluids, fiber, and activity, as appropriate, to prevent constipation. If a client is not able to meet the goal of a bowel movement with soft, formed stools every three days, then a bowel management program should be initiated.
Now that we have reviewed the basic structure and function of the urinary and gastrointestinal systems, let’s review the common alterations of urinary tract infection, urinary incontinence, urinary retention, constipation, diarrhea, and bowel incontinence in the following sections.
- National Institute of Diabetes and Digestive and Kidney Diseases. (2020). The urinary tract & how it works. U.S. Department of Health and Human Services. https://www.niddk.nih.gov/health-information/urologic-diseases/urinary-tract-how-it-works ↵
- “Urinary_System_(Male).png” by BruceBlaus is licensed under CC BY-SA 4.0 ↵
- National Institute of Diabetes and Digestive and Kidney Diseases. (2020). The urinary tract & how it works. U.S. Department of Health and Human Services. https://www.niddk.nih.gov/health-information/urologic-diseases/urinary-tract-how-it-works ↵
- National Institutes of Health. (2019). Pyridium. DailyMed. https://dailymed.nlm.nih.gov/dailymed/drugInfo.cfm?setid=165d01d4-a9f7-2293-e054-00144ff8d46c ↵
- Maddukuri, G. (2021). Urinary frequency. Merck Manual Professional Version. https://www.merckmanuals.com/professional/genitourinary-disorders/symptoms-of-genitourinary-disorders/urinary-frequency ↵
- Berry, C. (2020). Oliguria. Merck Manual Professional Version. https://www.merckmanuals.com/professional/critical-care-medicine/approach-to-the-critically-ill-patient/oliguria ↵
- Leslie, S. W. (2024). Nocturia. StatPearls [Internet]. https://www.ncbi.nlm.nih.gov/books/NBK518987/ ↵
- U.S. National Library of Medicine. (2023). Urination - excessive amount. MedlinePlus. https://medlineplus.gov/ency/article/003146.htm ↵
- Cherney, K. (2018). Everything you should know about pyuria. Healthline. https://www.healthline.com/health/pyuria ↵
- “Pyuria2011.JPG” by James Heilman, MD is licensed under CC BY-SA 3.0 ↵
- Maddukuri, G. (2021). Urinary frequency. Merck Manual Professional Version. https://www.merckmanuals.com/professional/genitourinary-disorders/symptoms-of-genitourinary-disorders/urinary-frequency ↵
- “Blausen_0316_DigestiveSystem.png” by Blausen.com staff is licensed under CC BY 3.0 ↵
- National Institute of Diabetes and Digestive and Kidney Diseases. (2017). Your digestive system & how it works. U.S. Department of Health and Human Services. https://www.niddk.nih.gov/health-information/digestive-diseases/digestive-system-how-it-works ↵
- U.S. National Library of Medicine. (2024). Rectal bleeding. MedlinePlus. https://medlineplus.gov/ency/article/007741.htm ↵
- U.S. National Library of Medicine. (2024). Black or tarry stools. MedlinePlus. https://medlineplus.gov/ency/article/003130.htm#:~:text=Black%20or%20tarry%20stools%20with,used%20to%20describe%20this%20finding ↵
- Meconium_Diaper.jpg” by Azoreg is licensed under CC BY-SA 3.0 ↵
Absence of urine output that is typically found during kidney failure. Can be defined as less than 50 mL of urine over a 24-hour period.
Painful or difficult urination.
Urinary frequency is the need to urinate many times during the day or at night (nocturia) in normal or less-than-normal volumes.
Blood in urine, either visualized or found during microscopic analysis.
Decreased urine output, defined as less than 500 mL urine in adults in a 24-hour period.
The need for a patient to get up at night on a regular basis to urinate.
Greater than 2.5 liters of urine output over 24 hours; also referred to as diuresis. Urine is typically clear with no color.
At least 10 white blood cells in each cubic millimeter of urine in a urine sample that typically indicates infection. In some cases, pus may be visible in the urine.
A sensation of an urgent need to void.
Involuntary contraction and relaxation of the muscles of the intestine, creating wave-like movements that push digested content forward in the digestive tract.
Black-colored stools can be caused by iron supplements or bismuth subsalicylate (Pepto-Bismol) taken for an upset stomach.
Bright red blood in the stools; also referred to as hematochezia.
Stools that are black and sticky that appear like tar; also referred to as melena.
Passage of black, tarry stools that are caused by blood in the GI tract.
The black to dark green, sticky first bowel movement of a newborn.
Incontinence when sleeping (i.e., bedwetting).

