5.12 Corticosteriods
Corticosteroids can be prescribed in a variety of routes. Fluticasone is an example of a commonly used inhaled corticosteroid that can be inhaled or used as a nasal spray. Prednisone is an example of a commonly used oral corticosteroid, and methylprednisolone is a commonly used IV corticosteroid. Additional information about corticosteroids and potential adrenal effects is located in the “Corticosteroids” section of the “Endocrine System” chapter.
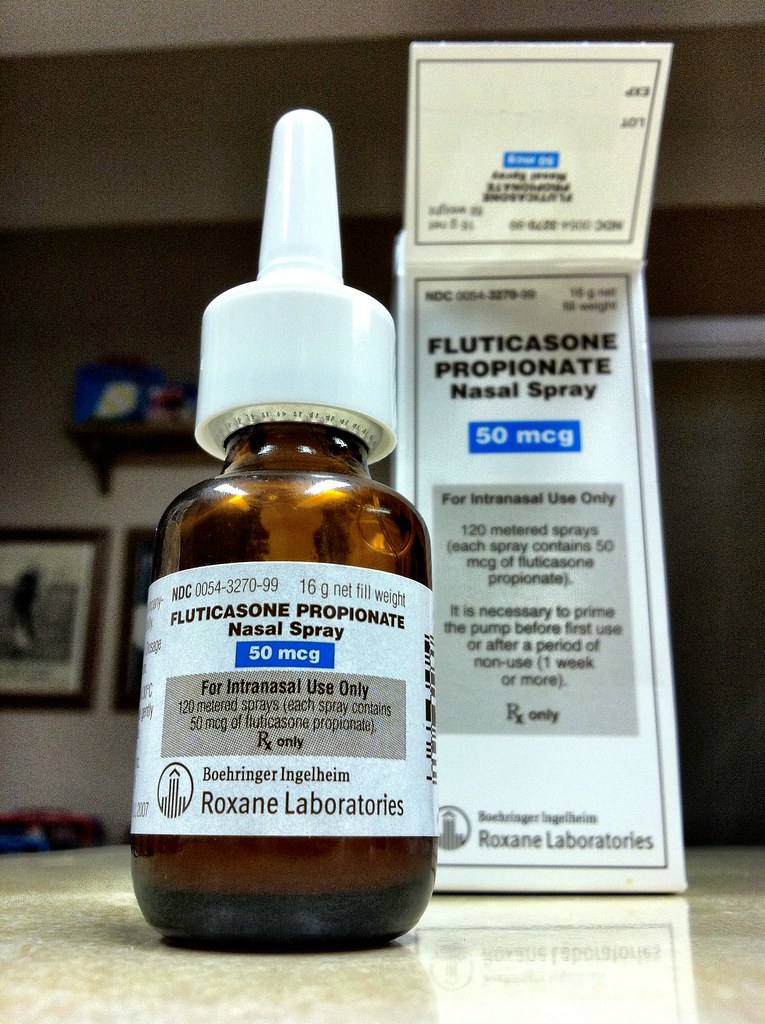
Mechanism of Action: Fluticasone is a locally acting anti-inflammatory and immune modifier. The nasal spray is used for allergies, and the oral inhaler is used for long-term control of asthma. Fluticasone is also used in a combination product with salmeterol. It decreases the frequency and severity of asthma attacks and improves overall asthma symptoms. See Figures 5.15-17[1],[2],[3] for images of different formulations of fluticasone.
Oral prednisone prevents the release of substances in the body that cause inflammation. It also suppresses the immune system.
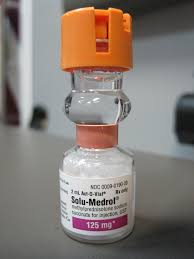
Methylprednisolone IV prevents the release of substances in the body that cause inflammation. It also suppresses the immune system. Methylprednisolone comes in powder form and must be reconstituted (mixed) with sterile saline before administration. See Figure 5.17[4] for an image of methylprednisolone.
Indications: Fluticasone inhalers are used to prevent asthma attacks. Fluticasone nasal spray is used to reduce inflammation of sinus passages. In respiratory conditions, oral prednisone is used to control severe or incapacitating allergic conditions, severe asthma, and acute exacerbations of COPD. Oral prednisone is also used to relieve contact dermatitis, atopic dermatitis, serum sickness, and drug hypersensitivity reactions. Methylprednisolone IV is used to rapidly control these same conditions.
Nursing Considerations: Fluticasone is safe for children aged 4 years and older. Prednisone and methylprednisolone are safe for all ages.
Side Effects/Adverse Effects: Fluticasone inhalers can cause hoarseness, dry mouth, cough, sore throat, and oropharyngeal candidiasis. Fluticasone nasal spray can cause dry nasal passages and epistaxis (nosebleeds). Clients should rinse their mouths after using corticosteroid inhalers to prevent candidiasis (thrush).
Prednisone and Methylprednisolone: See more information about adverse effects of corticosteroids in the in the “Corticosteroids” section of the “Endocrine System” chapter. Cardiovascular symptoms can include fluid retention, edema, and hypertension. Imbalances such as hypernatremia (↑Na), hypokalemia (↓K+), and increased blood glucose with associated weight gain can occur. CNS symptoms include mood swings and euphoria. GI symptoms can include nausea, vomiting, and GI bleed. In long-term therapy, bone resorption occurs, which increases the risk for fractures; the skin may bruise easily and become paper thin; wound healing is delayed; infections can be masked; and the risk for infection increases. Long-term corticosteroid therapy should never be stopped abruptly because life-threatening adrenal insufficiency may occur.[5]
Health Teaching & Health Promotion: Instruct clients to rinse their mouths after inhaler use to prevent candidiasis (thrush). Advise clients that corticosteroids are not used to treat an acute asthma attack. They can cause immunosuppression, suppress signs of infection, and cause an increase in blood glucose levels. Clients may experience weight gain, swelling, increased fatigue, bruising, and behavioral changes. These occurrences should be reported to one’s health care provider.[6]


Now let’s take a closer look at the medication grid for fluticasone, prednisone, and methylprednisolone in Table 5.12.[7],[8],[9]
Table 5.12 Fluticasone, Prednisone, and Methylprednisolone Medication Grid
Class/Subclass |
Prototype/Generic |
Nursing Considerations |
Therapeutic Effects |
Side/Adverse Effects |
|---|---|---|---|---|
| Corticosteroids | fluticasone | Rinse mouth after use
Do not use inhaler as a quick-relief medication for asthma attacks |
Nasal spray: Used for management of the nasal symptoms of perennial nonallergic rhinitis
Inhaler: Used to improve the control of asthma by reducing inflammation in the airways |
Nasal spray: Dry nasal passages and epistaxis (nosebleed)
Inhalers: Hoarseness, dry mouth, cough, sore throat, and oropharyngeal candidiasis
|
| Corticosteroids | prednisone | Do not use if signs of a systemic infection
When using more than 10 days, the dose must be slowly tapered May increase blood glucose levels |
Used to control severe or incapacitating allergic or respiratory conditions | CV: Fluid retention, edema, and hypertension
Electrolytes: ↑Na, ↓K+, ↑Ca, and ↑BG CNS: Mood swings and insomnia in high doses GI: Nausea, vomiting, and GI bleed MS: Bone resorption Skin: Acne, paper thin, bruises, infections, and delayed healing Increased appetite and weight gain Adrenal suppression Increased risk for infection, and infections can be masked Long-term use may result in Cushing’s syndrome |
| Corticosteroids | methylprednisolone | May increase blood glucose levels | Used to rapidly control severe or incapacitating allergic or respiratory conditions, in sepsis to reduce systemic inflammation, and to treat adrenal insufficiency | Same as prednisone |
- “Fluticasone Propionate Nasal Spray” by _BuBBy_ is licensed under CC BY 2.0 ↵
- “Fluticasone.JPG” by James Heilman, MD is licensed under CC BY-SA 4.0 ↵
- “Asthmatic Control” by David Camerer is licensed under CC BY-NC-ND 2.0 ↵
- “Methylprednisolone vial.jpg” by Intropin is licensed under CC BY 3.0 ↵
- Frandsen, G., & Pennington, S. (2018). Abrams’ clinical drug: Rationales for nursing practice (11th ed.). Wolters Kluwer. ↵
- uCentral from Unbound Medicine. https://www.unboundmedicine.com/ucentral ↵
- This work is a derivative of Pharmacology Notes: Nursing Implications for Clinical Practice by Gloria Velarde licensed under CC BY-NC-SA 4.0 ↵
- Frandsen, G., & Pennington, S. (2018). Abrams’ clinical drug: Rationales for nursing practice (11th ed.). Wolters Kluwer. ↵
- This work is a derivative of DailyMed by U.S. National Library of Medicine in the Public Domain. ↵

