7.3 A Systematic Approach to Interpreting an ECG
A systematic approach to interpreting an ECG improves the speed and reliability of the assessment, especially if a dysrhythmia is present. This section outlines a systematic approach to interpreting an ECG, as well as common findings in ECG waveforms that occur during dysrhythmias. Review basic information about ECG waveforms and intervals in Table 7.2a in the “Basic Concepts” section of this chapter. Supplementary videos demonstrating how to interpret an ECG are provided at the end of this section, and an online cardiac rhythm game in the “Learning Activities” section provides practice in interpreting ECG strips.
Calculate the Rate
Calculate the ventricular and atrial rates.
There are several methods to calculate the rate. The simplest method to obtain a ventricular rate is to count the number of R waves in a 6-second strip (i.e., over 30 large boxes) and multiply this number by 10. See Figure 7.10[1] for an image of counting the R waves on a 6-second strip for a ventricular heart rate of 80.
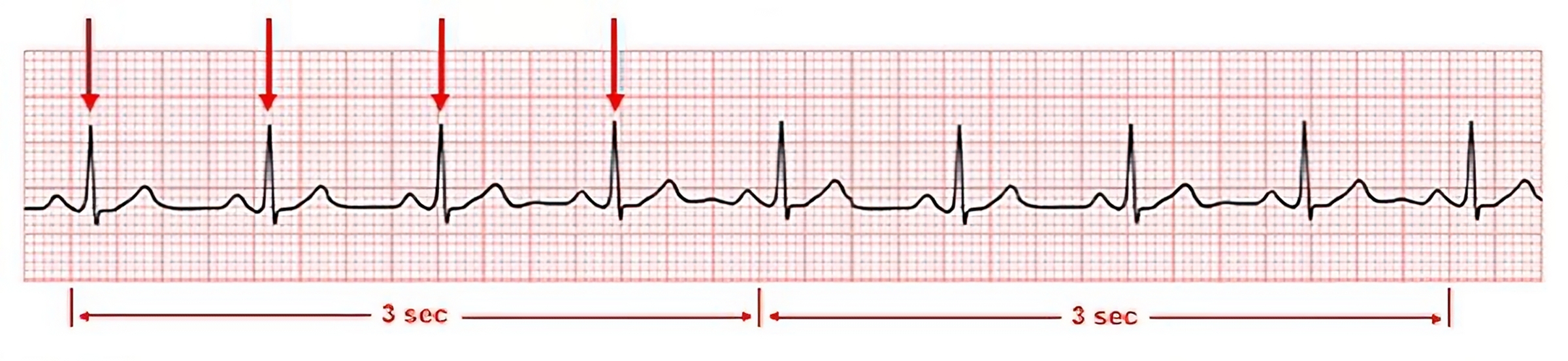
In a similar manner, the atrial rate can be calculated (if P waves are present) by counting the number of P waves in a 6-second strip and multiplying this number by 10. In order to ensure accuracy of this method, please make sure that the rhythm strip that is used is a 6-second strip.
Determine the Regularity of the Rhythm
Determine if the rhythm is regular or irregular.
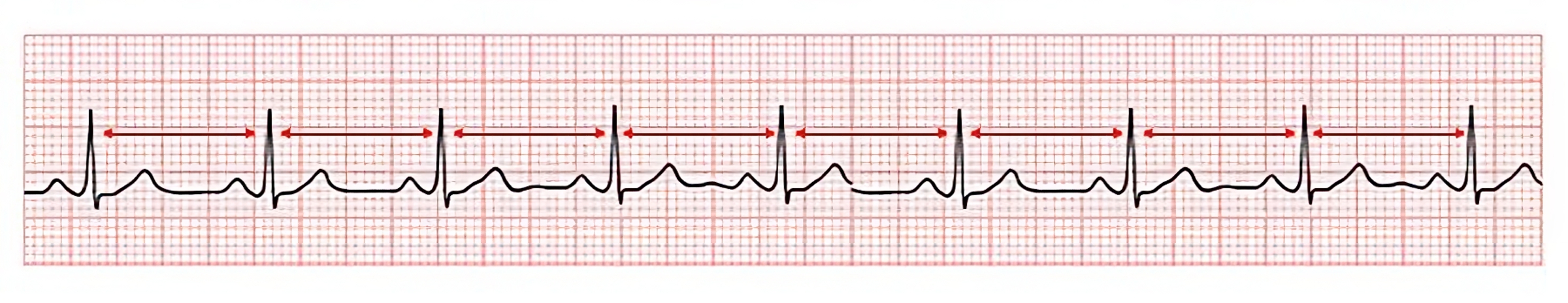
View leads I, II, aVF, and V1 for the most accurate interpretation of the rhythm.[2] Assess the distances between the R waves to determine the regularity of the rhythm using a caliper or ruler. It is important to assess the distances across the whole strip to account for any potential abnormality. See Figure 7.11[3] for an image depicting the R to R distance on an ECG strip. Cardiac rhythms are categorized into four types of rhythms:
- Regular Rhythm: The R to R distances are always equal distance apart. For example, normal sinus rhythm is a regular rhythm.
- Irregularly Irregular Rhythm: The R to R distances are never equal distances apart. For example, atrial fibrillation is an irregularly irregular rhythm.
- Regularly Irregular: The R to R distances are unequal, but there is a repetitive pattern to the unequal distances. For example, second-degree heart block type II may have a regularly irregular rhythm.
- Occasionally Irregular: The R to R distances are equal except for an occasional out of place R. For example, sporadic premature ventricular contractions (PVCs) are an occasionally irregular rhythm.
Assess the P Waves
The P waves are critical to determining the origin of a heartbeat. Assess the following characteristics related to the P waves:
- Are P waves present? The absence of P waves indicates the heartbeat did not originate in the SA node.
- Do all of the P waves look the same? When a heartbeat originates somewhere other than the SA node, the contour of the P wave changes.
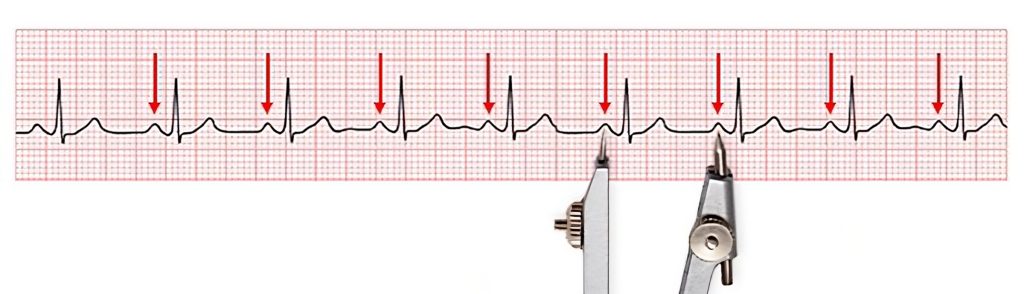
- Do the P waves occur at a regular rate? Using a caliper or ruler, assess the distance from “P to P” waves. If this distance varies, there is an issue in conduction from the SA node to the AV node. See Figure 7.12[4] for an image of assessing the distance between P waves.
- Is there one P wave with every QRS complex? This helps to further assess conduction. Is the electrical communication between the atria and the ventricles working correctly?
An example of a dysrhythmia that lacks P waves is atrial fibrillation. The presence of “irregularly irregular” narrow QRS complexes with no distinct P waves or a wavy baseline is the hallmark feature in the identification of atrial fibrillation.[5]
Determine the PR Interval
Measure the distance from the beginning of the P wave to the beginning of the QRS complex.
Recall that the normal PR interval is 0.12 to 0.2 seconds (i.e., 3-5 small boxes). When the PR interval is too long, there is a problem with conduction from the SA node to the AV node. A delay in SA to AV node conduction is representative of a heart block. See Figure 7.13[6] for an image of measuring the PR interval.
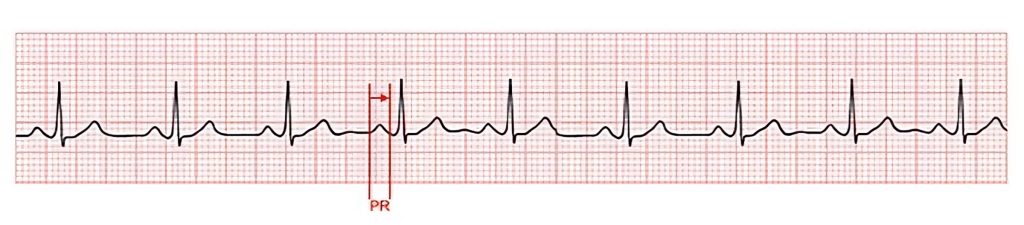
The PR interval represents the time from the beginning of atrial depolarization to the start of ventricular depolarization and includes the delay at the AV node. Variations in the PR interval can be seen in various disorders. For example, a long PR interval may indicate first-degree AV block. Short PR intervals are present in conditions with accelerated AV conduction, such as Wolf-Parkinson-White syndrome, a disorder that is present at birth.[7]
Determine the QRS Duration
Measure the distance from the beginning to the end of the QRS complex.
Recall that normal QRS duration is 0.04 to 0.12 seconds (i.e., 1-3 small boxes). When the QRS complex is too wide, it indicates the heartbeat did not originate in the atria. See Figure 7.14[8] for an image of measuring the QRS duration.
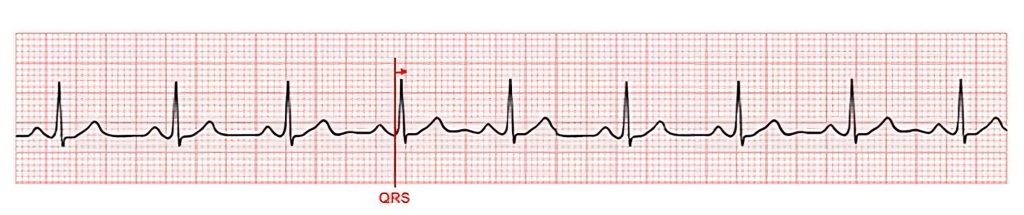
The QRS complex represents ventricular depolarization as the electrical signal passes down from the AV node. A prolonged QRS may indicate hyperkalemia or bundle branch block. A premature ventricular contraction, intraventricular conduction delay (bundle branch block), or other ventricular dysrhythmias are associated with a wide QRS.[9]
Evaluate the T Waves
Evaluate the T waves. Do they follow the QRS complex? Are they upright and rounded?
Recall the T wave represents ventricular repolarization. Its morphology is highly susceptible to cardiac and noncardiac influences such as hormonal and neurological factors. The size of a typical T wave is between one eighth and two thirds of the size of the R wave and a height of less than 10 mm.
Abnormalities in the T wave morphology include inverted, flat, biphasic, or tall tented or peaked T waves. T wave changes can occur with a variety of conditions. Tall T waves in an anterior chest lead III, aVR, and V1 with a negative QRS complex may suggest acute myocardial ischemia. Other causes of T wave abnormalities are caused by temporary physiological factors (for example, after eating a high carbohydrate meal), endocrine or electrolyte imbalances, myocarditis, pericarditis, cardiomyopathy, post-cardiac surgery state, pulmonary embolism, fever, infection, anemia, acid-base disorders, drugs, endogenous catecholamines, metabolic changes, acute abdominal processes, and intracranial pathology.[10]
Evaluate the ST Segment
What is the appearance of the S-T segment? Is it isoelectric (i.e., is it on the same level of the PR segment)?
Recall the ST segment depicts the interval between the end of ventricular depolarization and the beginning of ventricular repolarization. A normal ST segment falls along the isoelectric line and lies at the same level as the PR interval. See Figure 7.15[11] to review an illustration of ST segments, waves, and other intervals discussed in this section.
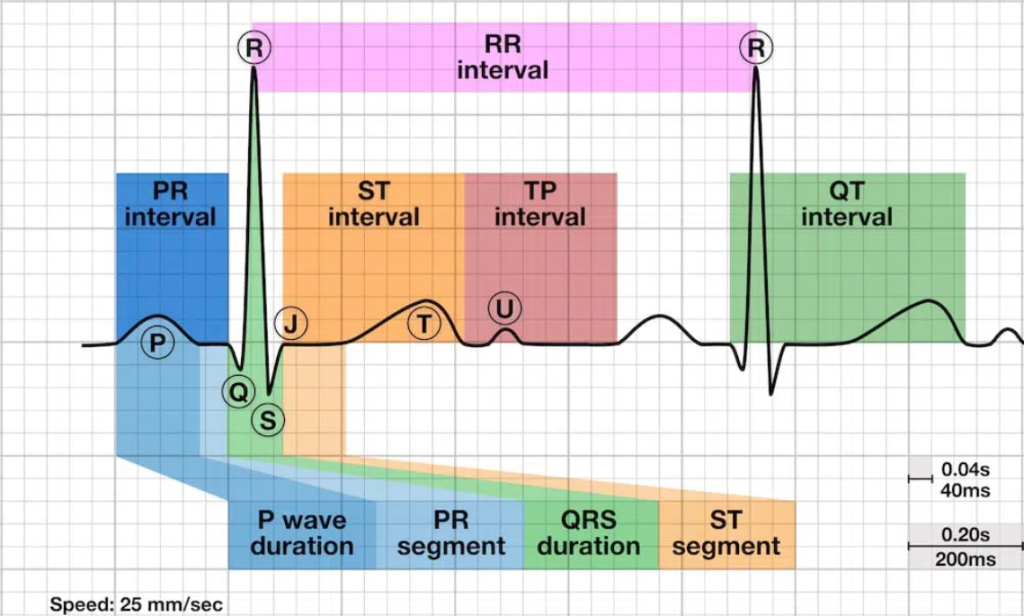
Elevation or depression of the ST segment by 1 mm or more, measured at the J point, is abnormal. The J point is a region between the QRS complex and the ST segment. ST elevation is highly specific if present in two or more contiguous leads in the setting of an acute myocardial infarction and usually indicates a complete blockage of the coronary artery. If ST elevation on the ECG tracing above the baseline after the J point is at least 1 mm in a limb lead or 2 mm in a precordial lead, it is clinically significant for diagnosing acute myocardial infarction. ST depression greater than 1 mm below the baseline is often a sign of myocardial ischemia or angina. It can appear as a downsloping, upsloping, or a horizontal segment on the ECG. ST depressions are also associated with nonischemic causes, including digoxin toxicity, hypokalemia, hypothermia, and tachycardia.[12]
Determine the QT Interval Duration
Is the QT (or QTc) interval duration within normal limits?
Recall the QT interval, measured from the Q wave to the end of the T wave, represents the start of depolarization to the end of the repolarization of the ventricles. Generally, the normal QT interval is less than 0.4 to 0.44 seconds. Women usually have a slightly longer QT interval than men, and heart rate also impacts the QT interval, so typically the corrected QT interval (QTc) is monitored.
A short QTc (less than 0.36 seconds) may be associated with hypercalcemia, acidosis, hyperkalemia, hyperthermia, or short QT syndrome.[13] A prolonged QTc presents an imminent risk for serious ventricular arrhythmias, including torsades de pointes, ventricular tachycardia, and ventricular fibrillation. Common causes of QTc prolongation include side effects of medications, electrolyte abnormalities such as hypocalcemia and hypomagnesemia, and congenital long QT syndrome.[14]
Evaluate Other ECG Components
Are there extra beats on the waveform? Is anything else abnormal?
The U wave is a small wave that can follow the T wave, though it is not always visible. It represents the delayed repolarization of the papillary muscles or Purkinje fibers and is commonly associated with hypokalemia.[15]
The J wave is an abnormal finding typically found during hypothermia. It appears as an extra deflection on an ECG at the QRS complex and ST segment junction.[16]
Clinically Observe the Client
When analyzing an ECG strip, it is vital to clinically observe the client for signs and symptoms that determine the significance of the dysrhythmia. For example, the more abnormal a rhythm becomes, the less blood the heart pumps, causing symptoms due to low blood pressure such as dizziness, confusion, and loss of consciousness.[17]
View a supplementary YouTube video[18] on ECG interpretation basics:
View a supplementary YouTube video[19] on PQRST EKG rhythm:
- “Counting the R Waves” by Chippewa Valley Technical College is licensed by CC BY 4.0 ↵
- This work is a derivative of StatPearls by Sattar and Chhabra and is licensed under CC BY 4.0 ↵
- “Assessing Distance Between R Waves” by Chippewa Valley Technical College is licensed by CC BY 4.0 ↵
- “Assessing Distance Between P Waves” by Chippewa Valley Technical College is licensed by CC BY 4.0 ↵
- This work is a derivative of StatPearls by Sattar and Chhabra and is licensed under CC BY 4.0 ↵
- “Measuring the PR Interval” by Chippewa Valley Technical College is licensed by CC BY 4.0 ↵
- This work is a derivative of StatPearls by Sattar and Chhabra and is licensed under CC BY 4.0 ↵
- “Measuring the QRS Duration” by Chippewa Valley Technical College is licensed by CC BY 4.0 ↵
- This work is a derivative of StatPearls by Sattar and Chhabra and is licensed under CC BY 4.0 ↵
- This work is a derivative of StatPearls by Sattar and Chhabra and is licensed under CC BY 4.0 ↵
- “ECG-waves-segments-and-intervals-LITFL-ECG-library-3.jpg” by unknown author at LITFL is licensed under CC BY-NC-SA 4.0. Access the original image at https://litfl.com/st-segment-ecg-library/ ↵
- This work is a derivative of StatPearls by Sattar and Chhabra and is licensed under CC BY 4.0 ↵
- This work is a derivative of StatPearls by Sattar and Chhabra and is licensed under CC BY 4.0 ↵
- This work is a derivative of StatPearls by Sattar and Chhabra and is licensed under CC BY 4.0 ↵
- This work is a derivative of StatPearls by Sattar and Chhabra and is licensed under CC BY 4.0 ↵
- This work is a derivative of StatPearls by Sattar and Chhabra and is licensed under CC BY 4.0 ↵
- Physical Therapy Reviewer. (n.d.). How to read an ECG. https://ptreviewer.com/electrocardiogram-ecg-2/reading-an-ecg/ ↵
- RegisteredNurseRN. (2022, March 7). EKG/ECG interpretation basics nursing NCLEX | QRS complex, P wave, T wave, PR interval [Video]. YouTube. All rights reserved. https://youtu.be/bUF12VIgzP0 ↵
- RegisteredNurseRN. (2015, May 21). How to memorize the PQRST EKG rhythm strip wave for anatomy & pathophysiology [Video]. YouTube. All rights reserved. https://youtu.be/QAQiK-zRtl0 ↵

