1.7 Specialized Infusions
In addition to the provision of IV fluid therapy and medication administration via the intravenous route, nurses must also be aware of specialized infusions and the safety implications that may be associated with these types of infusions. Two types of specialized infusions include medication administered via a patient-controlled analgesia (PCA) pump and those administered via epidural infusion. There are many unique advantages and risks associated with specialized infusions, and nurses must be aware of the safety implications and associated interventions to ensure quality patient care.
Patient-Controlled Analgesia
Patient-controlled analgesia (PCA) is a method of pain management that allows hospitalized patients with severe pain to safely self-administer opioid medications using a programmed pump according to their level of discomfort. A computerized pump contains a syringe of pain medication and is connected directly to a patient’s intravenous (IV) line. Doses of medication can be administered as either a basal (i.e., continuous) rate, self-administered as needed on demand, or a combination of both methods. Doses are self-administered by the patient by pressing a button that initiates a “demand” for medication. However, the pump is programmed to only allow administration of medication every set number of minutes with a maximum dose of medication every hour. These pump settings and the design of the system require the patient to be alert enough to press the button to receive a demand dose. These design features are safety measures to help prevent overmedication that can cause sedation and respiratory depression. However, despite these safety measures it is vital for nurses to closely monitor patients receiving PCA for respiratory depression.[1] See Figure 1.18[2] for an image of a PCA pump.
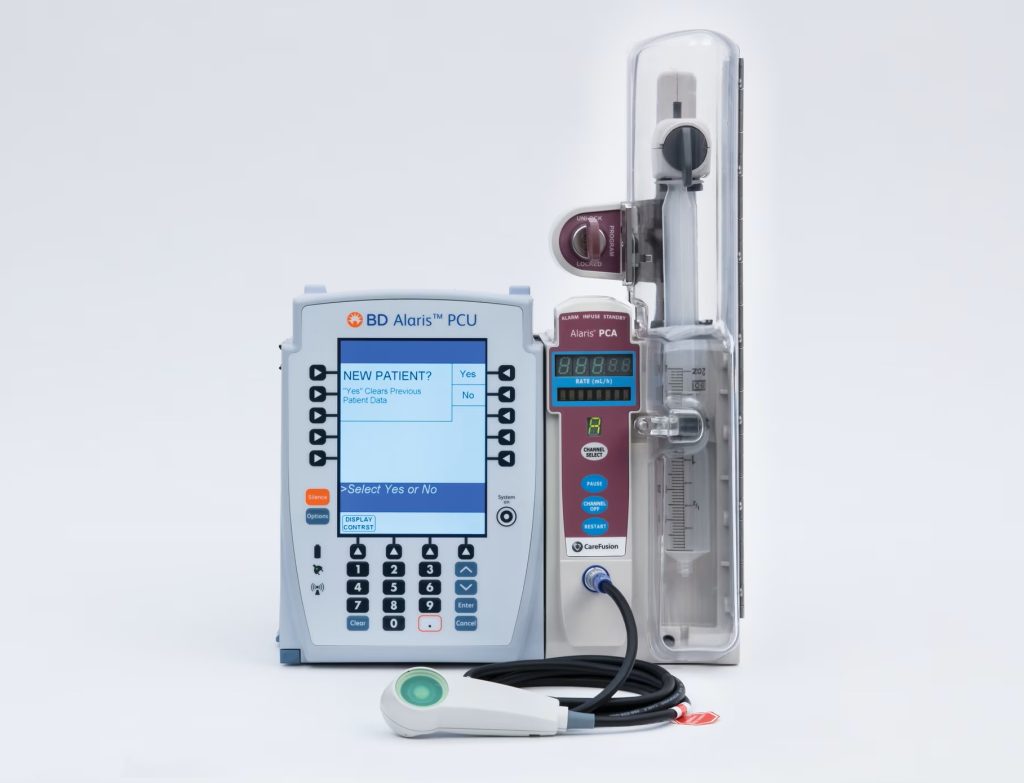
Patient-controlled analgesia can be very beneficial for select patients, reducing the time for medication administration and allowing pain medication to reach the patient more rapidly to reduce pain symptoms. This can help prevent out-of-control pain levels that require a significant length of time to resolve. The principles behind the method of patient-controlled analgesia involve the patient’s experience of pain, subsequent administration of a drug via the PCA pump, the drug action within the bloodstream, and the patient response. Depending on the level of pain relief, the patient may experience symptom resolution or may proceed with a dose demand process by activating the PCA pump at a subsequent interval. The patient becomes an active party in medicating themselves to help control the pain experience.
It is critical that patients who are prescribed a PCA pump with demand dosing understand the safety principles behind the medication administration. Patients and their family members must be aware that only the patient is allowed to initiate the demand dose by pressing the medication button to ensure they are alert enough to do so. In this manner, oversedation and life-threatening respiratory depression can be avoided with demand dosing.
Additionally, patients should receive education regarding the frequency with which they will receive a demand dose in order to be reassured that they cannot accidentally overdose themselves by pressing the demand button too frequently. Cues such as an audible “beep” often accompany the demand dose and can help cue the patient that the medication was administered. Conversely, if the demand button has been initiated too closely within the programmed interval, an audible “chirp” may signal to the patient that the demand dose was too soon. The patient should receive instruction that if the chirp has been noted, they may wish to wait a few minutes and reinitiate the demand.
Patients with impaired cognition or restricted upper extremity dexterity may not be appropriate for PCA. If a nurse has concerns regarding the appropriateness of self-administration of pain medication via a PCA pump based on characteristics and clinical condition of an individual patient, the prescribing provider should be notified, and alternate pain control measures should be considered.
The basic principles of a PCA medication order include the following:
Loading dose: Ordered amount of medication administered at the time of PCA initiation
Demand dose: Medication dose given on activation of demand (pressing the demand button)
Lockout interval: Time period in which no follow-up demand dose may be administered (even if demand button is activated)
Basal infusion: Continuous rate of medication administration, regardless of demand attempts
Lockout maximum: The maximum dose of medication that can be administered within a certain period, commonly prescribed to 1 hour limit
Breakthrough bolus dose: A dose of opioid or non-opioid medication administered by the nurse for breakthrough pain.
Medications that are commonly prescribed for PCA administration include opioids such as morphine, hydromorphone, and fentanyl. Nurses must be familiar with specific institutional policies and protocols regarding the use of PCA administration. These protocols commonly include the use of specific provider orders, safety checks, and patient monitoring. Many organizations have transitioned to the use of preprinted PCA order sets to help guarantee that required PCA dosing parameters are appropriately addressed. Within a PCA order, the prescriber must include the following information: identification of the specific medication to be used in the PCA pump, the medication concentration, the specific quantity of the demand dose, the lockout interval, and the order lockout maximum. When a nurse is initiating a PCA pump, it is critical that the order be reviewed and verified with another registered nurse according to agency policy. The double-check verification helps ensure that the pump is programmed correctly, and lockout limits are included to decrease the risk of accidentally self-administering too much medication.[3]
Due to the potential adverse effects of opioids administered via a PCA pump, there is a significant risk for patient safety requiring specific monitoring by the nurse. Continuous pulse oximetry, end tidal carbon dioxide monitoring, and frequent vital signs monitoring may be required with initiation and ongoing use of a PCA pump. Individuals with obstructive airway disease, sleep apnea, obesity, renal or hepatic impairment, and recent analgesia, sedation, or anesthesia are at increased risk of complications associated with PCA administration, such as decreased level of consciousness, respiratory distress, and hypotension.[4] Dosing parameters must account for patient specific factors and individualized clinical need when initiated by the prescribing provider. Additionally, nurses must be especially vigilant when first initiating PCA infusion because initial infusion is when administration complications may be more frequently observed.
Please review the “Adverse Effects of Opioids” section in Open RN Nursing Fundamentals for more information about potential patient side effects.
Nursing staff must also be cognizant of the post-administration assessment and individualized response of each patient to PCA. Even though the patient is actively participating in their pain control plan through self-administration, pain response must be thoroughly documented. Nurses must frequently assess the patient’s number of demands and subsequent doses received. Nurses should also carefully monitor the patient’s vital signs, pain self-report, and nonverbal indications of the pain experience. This focused pain assessment helps ensure that the pain level is adequately controlled.
The use of PCA pumps require vigilant checks by two licensed registered nurses minimally at the start of every shift. The secure PCA pump holds the prescribed opioid medication in a locked device with a demand button that is given to the patient. Keys to the PCA pump are safely stored in secure areas such as within an automated drug dispensing machine. The pumps also have an access code to ensure that tampering with the pump settings does not occur. To document the amount and frequency of pain medication the patient is receiving, as well as to prevent drug diversion, the settings on the pump are checked at the end of every shift as part of the bedside report. The incoming and outgoing nurses double-check and document the pump settings, the amount of medication administered during the previous shift, and the amount of medication left in the syringe. When a PCA is discontinued, nurses must carefully document the remainder of medication left in the PCA syringe and follow organizational policies related to narcotic wasting and documentation.
PCA pumps often have specialized tubing and connections to prevent inadvertent connection of secondary medication to the dedicated PCA line above the pump. If a bolus of medication is administered via a dedicated PCA line below the pump, the nurse must ensure it is compatible with the PCA medication.
Epidural
Epidural medication administration is a type of specialized infusion that is different than intravenous infusion. The use of an epidural involves administering analgesics and anesthetics directly into the spinal fluid via an epidural catheter for severe pain management. It is inserted by specially trained health professionals and requires additional safety measures and nurse monitoring to help prevent patient complications. Safety measures such as specially colored tubing and different Luer lock systems are incorporated to ensure only epidural medications are administered via the epidural line.
Epidurals are typically used with surgical procedures or during labor and delivery. Epidural infusions may also be used to treat chronic pain that has not responded to more conservative treatments. Common anesthetics that are used in epidural infusions include bupivacaine and ropivacaine administered alone or in combination with opioid medications. Anesthetics and analgesics administered via the epidural route work synergistically (i.e., cooperatively) to provide greater pain relief at lower doses.[5] See Figure 1.19[6] for an image of an epidural pump with colored tubing and an image of freshly inserted lumbar epidural catheter. The epidural site has been prepared with tincture of iodine, and the dressing has not yet been applied.
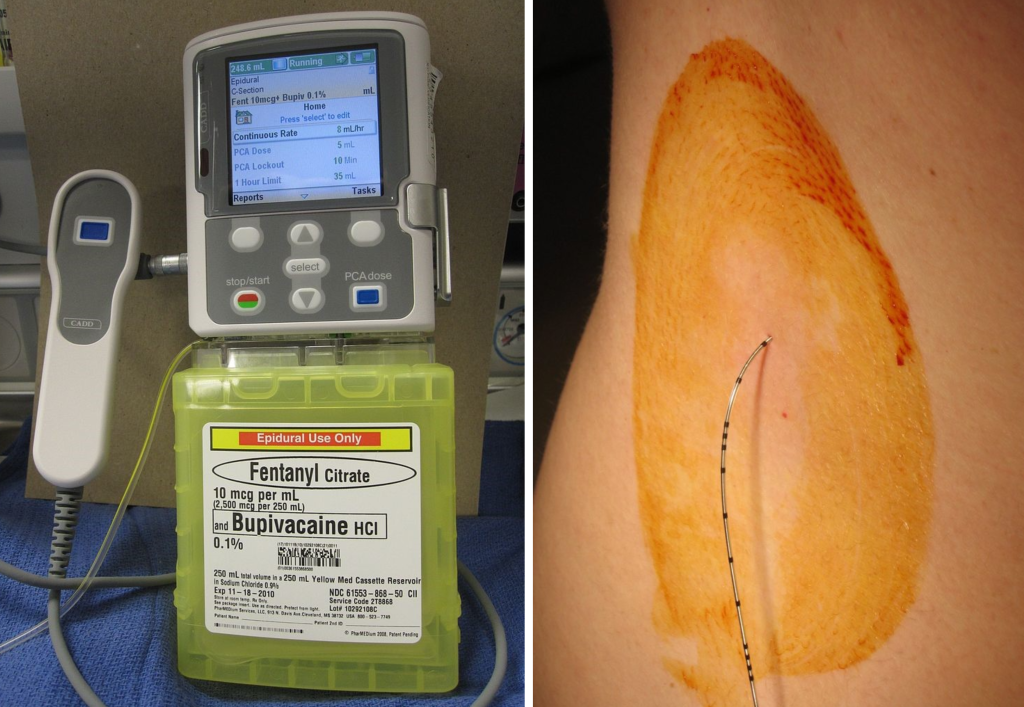
Epidural catheters are inserted and may only be repositioned by trained anesthesia professionals. The anesthesia provider will administer a test dose of medication into the epidural to ensure that it is appropriately positioned. Once adequate positioning has been confirmed, the anesthesia provider will record the documented block height by assessing the patient’s response to cold at various levels of the thoracic spine. This should be recorded in the patient’s chart and is the subsequent block height for all future neurosensory assessments. Any block level that progresses up the body or is recorded above a level of T4 (fourth thoracic vertebra) must be immediately communicated to the anesthesia provider to prevent respiratory distress and cardiovascular collapse.[7]
Once the catheter has been inserted and the position safely confirmed, a prescribing provider will order the medication for epidural infusion. The order must contain the medication name, concentration, and infusion rate. The epidural pump is similar to a PCA pump in that it must be locked and the infusion settings securely programmed. Some epidural pumps allow patients to self-administer on-demand doses. The initiation of the epidural medication may involve setting the pump to infuse at a constant rate or by providing an initial bolus dose and then a constant infusion rate.
Nurses caring for patients receiving epidural medications must monitor patient response to the medication and the epidural insertion site for potential complications associated with epidural infusion. Follow agency policy regarding focused assessments that typically include the patient’s pain management response, vital signs, and motor/sensory checks. Signs of respiratory depression must be carefully monitored and reported to the provider if the patient exhibits a respiratory rate of less than eight breaths/minute, declining oxygen saturation, or decreased level of consciousness. Nurses must also carefully observe the patient’s blood pressure and heart rate with epidural analgesia. Changes in vital signs may be associated with the epidural infusion but can also be the result of post-procedural complications, so vigilant postoperative monitoring must occur. Patients receiving epidural administration are also at risk for bradycardia, so atropine should be readily available in case the patient experiences symptomatic bradycardia.[8],[9]
Nurses should be prepared to assess for signs of potential clinical problems associated with epidural usage. Table 1.7 summarizes common clinical problems associated with epidural infusions.
Table 1.7 Clinical Problems and Interventions With Epidural Infusions[10],[11]
| Clinical Problem | Potential Interventions |
|---|---|
| Inadequate pain control; partial block | Work with the anesthesia provider to adjust the patient’s position or increase infusion rate. If the block is one-sided, position the patient painful side down to allow gravity to assist the medication to travel down the nerves on the side of pain. |
| Hypotension | Hypotension may occur with epidural use due to the dilation of blood vessels. Notify the provider. The epidural rate may need to be decreased or bolus fluids administered. The patient may require placement in Trendelenberg position. |
| Bradycardia | May occur as the result of blockage of sympathetic nerves. If symptomatic, notify the provider and anticipate possible administration of atropine. |
| Increasing sensation block height/difficulty breathing | The patient may first report signs of tingling in fingers, especially the fifth digits. Notify the provider, turn off infusion, elevate the patient’s head, and administer oxygen. |
| Motor blockage | Leg weakness may occur as a result of an epidural block to the low motor nerves. A reduction in rate may be needed if significant paralysis is experienced. Be cautious of mobility implications associated with reduced sensation. |
| Respiratory depression | If a patient experiences respiratory depression of less than eight breaths per minute, stop the infusion and notify the provider. If indicated, request emergency assistance and administer rescue breaths via a bag-valve-mask. |
| Catheter disconnection | Disconnection of the epidural line presents an increased infection risk. Immediately contact the anesthesia provider, but do NOT reconnect the line. The end of the line may be covered with sterile gauze, according to agency policy, until the anesthesia provider arrives. |
| Catheter migration | Migration of the epidural catheter into a blood vessel may result in exacerbated respiratory depression and sedation. Monitor the patient for any report of tingling around the mouth, numbness, twitching, convulsion, or cardiac arrest. Immediately stop the epidural infusion and provide emergency assistance and cardiopulmonary support. |
Common side effects of epidural medication infusion include nausea and itching associated with the specific medications included in the infusions. Many times, these side effects can be adequately managed with medications, and the epidural infusion may continue. Another common side effect is urinary retention. Nurses should monitor urine output for patients who do not have a urinary catheter in place. Intermittent or indwelling catheterization may be required to drain the bladder and prevent discomfort.[12],[13]
- Soffin, E. M., & Liu, S. S. (2018). Patient-controlled analgesia. In H. T. Benzon, S. N. Raja, S. M. Fishman, S. S., & S. P. Cohen’s (Eds.). Essentials of pain medicine (4th ed., pp. 117-122.e2). Elsevier. https://doi.org/10.1016/B978-0-323-40196-8.00013-9 ↵
- "alaris-pca-module-IF-0518-0034" by unknown author used on the basis of Fair Use. Access original image at https://www.bd.com/en-us/products-and-solutions/products/product-families/bd-alaris-pca-module. ↵
- Soffin, E. M., & Liu, S. S. (2018). Patient-controlled analgesia. In H. T. Benzon, S. N. Raja, S. M. Fishman, S. S., & S. P. Cohen’s (Eds.). Essentials of pain medicine (4th ed., pp. 117-122.e2). Elsevier. https://doi.org/10.1016/B978-0-323-40196-8.00013-9 ↵
- Soffin, E. M., & Liu, S. S. (2018). Patient-controlled analgesia. In H. T. Benzon, S. N. Raja, S. M. Fishman, S. S., & S. P. Cohen’s (Eds.). Essentials of pain medicine (4th ed., pp. 117-122.e2). Elsevier. https://doi.org/10.1016/B978-0-323-40196-8.00013-9 ↵
- Benzon, H. T., Raja, S., Liu, S. S., Fishman, S., Cohen, S. P., & Hurley, R. W. (Eds.). (2018). Essentials of pain medicine (4th ed., pp. 117-122.e2). Elsevier. https://doi.org/10.1016/C2014-0-03837-3 ↵
- “PCA-01.JPG” by DiverDave is licensed under CC BY-SA 3.0 and Epidural.JPG” by User:Ravedave is licensed under CC BY-SA 3.0 ↵
- Galligan, M. (2020). Care and management of patients receiving epidural analgesia. Nursing Standard, 35(12), 77-82. https://doi.org/10.7748/ns.2020.e11573 ↵
- Galligan, M. (2020). Care and management of patients receiving epidural analgesia. Nursing Standard, 35(12), 77-82. https://doi.org/10.7748/ns.2020.e11573 ↵
- Woodall, W. G. (2019). Care for the patient receiving epidural analgesia. Medsurg Nursing, 28(3), 194-195. https://go.openathens.net/redirector/liberty.edu?url=https://www.proquest.com/scholarly-journals/care-patient-receiving-epidural-analgesia/docview/2242627838/se-2?accountid=12085 ↵
- Galligan, M. (2020). Care and management of patients receiving epidural analgesia. Nursing Standard, 35(12), 77-82. https://doi.org/10.7748/ns.2020.e11573 ↵
- Woodall, W. G. (2019). Care for the patient receiving epidural analgesia. Medsurg Nursing, 28(3), 194-195. https://go.openathens.net/redirector/liberty.edu?url=https://www.proquest.com/scholarly-journals/care-patient-receiving-epidural-analgesia/docview/2242627838/se-2?accountid=12085 ↵
- Galligan, M. (2020). Care and management of patients receiving epidural analgesia. Nursing Standard, 35(12), 77-82. https://doi.org/10.7748/ns.2020.e11573 ↵
- Woodall, W. G. (2019). Care for the patient receiving epidural analgesia. Medsurg Nursing, 28(3), 194-195. https://go.openathens.net/redirector/liberty.edu?url=https://www.proquest.com/scholarly-journals/care-patient-receiving-epidural-analgesia/docview/2242627838/se-2?accountid=12085 ↵
A method of pain management that allows hospitalized patients with severe pain to safely self-administer opioid medications using a programmed pump according to their level of discomfort.
Ordered amount of medication administered at the time of PCA initiation.
Medication dose given on activation of demand (pressing the demand button).
Time period in which no follow-up demand dose may be administered (even if demand button is activated).
Continuous rate of medication administration, regardless of demand attempts.
The maximum dose of medication that can be administered within a certain period, commonly prescribed to 1 hour limit.
A dose of opioid or non-opioid medication administered by the nurse for breakthrough pain.
The administration of analgesics and anesthetics into the spinal fluid via an epidural catheter for severe pain management associated with surgical procedures or during labor and delivery.
Level of epidural nerve block recorded by assessing the patient’s response to cold at various levels of the thoracic spine.

