2.2 Basic Concepts of IV Push Medication
There are several advantages, disadvantages, and potential complications that can occur when administering IV push medication, requiring the nurse to implement many safety considerations.
Advantages
Intravenous push (IV push) is a process of introducing a medication or fluid substance directly into the bloodstream via the venous system. When the medication is administered directly into the bloodstream, it immediately enters the circulatory system and travels to a site of action. Administering the medication directly into the bloodstream reduces the first-pass effect or the action that occurs when a medication must be first metabolized or broken down prior to entering the blood. First-pass effect results in a diminished volume of available circulating drug and a subsequent decrease in therapeutic action.[1] As a result, when utilizing IV push medications, a decreased dosage of medication can be given compared to an oral dosage to achieve the same therapeutic effect.
First-pass metabolism significantly impacts the bioavailability of many medications. For example, larger oral doses of morphine must be provided than intravenous dosages to obtain the same therapeutic pain relief, but the risks of oversedation and respiratory depression are higher with intravenous doses. Nurses who have concerns about an ordered dose of intravenous medication should clarify the dosage with the pharmacist and/or prescribing provider before administering it.
Intravenous medication administration also has a more rapid onset than oral medication. Because the bioavailability of the medication is directly in the circulatory system, the medication is readily transported to the site of action. This is a significant benefit when a rapid response is needed, such as when clients are experiencing severe hemodynamic instability or severe pain.
Let’s consider the following scenario: A nurse on a medical telemetry unit received a direct admission from a cardiac clinic for an 85-year-old male client admitted with an exacerbation of chronic heart failure. The client’s vital signs are heart rate 102, blood pressure 144/88, respiratory rate 24, and pulse oximetry reading of 90% on room air. The nurse listens to the client’s lung sounds and notes crackles in both posterior lungs. The nurse reviews the admitting orders from the provider and sees an order for furosemide 40 mg IV push STAT. Review furosemide’s drug action profile in Table 2.2a and note the different onsets of action for the different routes of furosemide. It is clear that the IV push route of administration will work quickly to remove this client’s excess fluid and positively impact their respiratory status.
Table 2.2a Furosemide Drug Action Profile[2]
| Route | Onset | Peak |
|---|---|---|
| PO | 30-60 minutes | 1-2 hours |
| IM | 10-30 minutes | Unknown |
| IV | 5 minutes | 30 minutes |
Intravenous medication administration can also be of great benefit when clients are experiencing gastrointestinal issues that may affect absorption, such as impaired swallowing or esophageal, stomach, or intestinal absorption issues. Administering a medication directly into the cardiovascular system allows the substance to freely circulate throughout the body and bypass the breakdown and absorption barriers created by the gastrointestinal tract. See Figure 2.1[3] for an image of a nurse administering IV push medication.
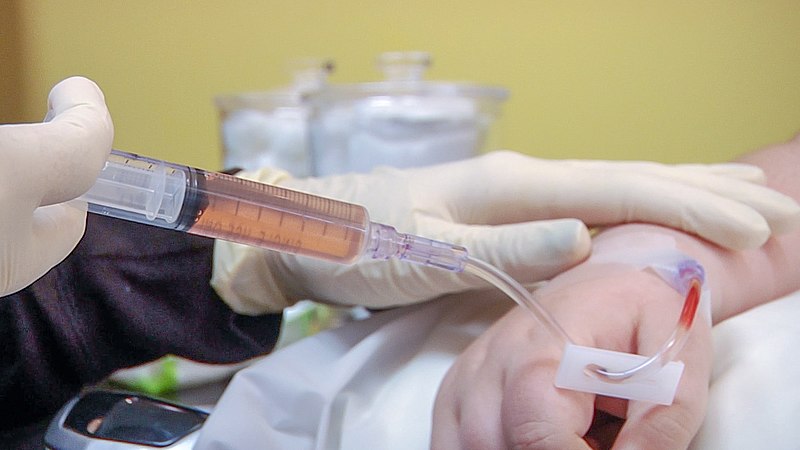
In addition to rapid onset, some medications are only formulated to administer via the IV route, such as certain vasoactive substances. As a result, many patients who are hospitalized may have an “IV lock” inserted to facilitate rapid IV access if their condition deteriorates. An IV lock (also referred to as a “saline lock”) is an IV cannula that has been inserted into a peripheral vein with a short extension tube that is filled with saline and clamped to keep the cannula patent. This type of IV access may also be referred to as a “peripheral lock” because it is inserted into the peripheral vasculature. Historically, many IV locks were flushed with heparin to keep the line from clotting, so they were referred to as a “heparin lock” or “hep lock.” Although evidence-based practice no longer recommends heparin be used to maintain patency of a peripheral IV access device, the name “hep lock” may still be used in practice. An IV lock is beneficial because it provides rapid access to administering medications in the venous system if needed, but continuous infusion of medication or fluid is not required.
IV push medication can also be a valuable alternative route of administration for clients at risk for fluid volume overload. For example, clients who are experiencing acute renal failure or an acute exacerbation of heart failure may benefit from IV push medications administered with smaller amounts of fluids compared to a typical IV infusion of medication.[4]
One of the most obvious benefits of IV push medication administration from a client’s perspective is that it does not require repeated needlesticks for administering repetitive doses of medications intramuscularly or subcutaneously. As a result, client discomfort is minimized when intravenous access can be maintained.
Disadvantages and Potential Complications
When administering IV push medication, nurses must always proceed with significant caution. Remember that medication administered via IV push cannot be retrieved! For this reason, it is vital for the nurse to perform the rights of medication administration before giving IV push medications. The rights of medication administration are reviewed in the “Safety Concepts” subsection later in this section.
Prior to administration, the nurse must carefully review the client’s current IV solutions and/or medications for incompatibilities with the medication to be administered. Many maintenance fluids (i.e., fluids given intravenously to facilitate hydration status) may include additives like electrolytes that may not be compatible with all medications. Nurses must ensure that all components are compatible with one another to ensure that a precipitate does not form when the substances come into contact with one another. A precipitate is the formation of small crystals as the incompatible substances come in contact with one another. Precipitate can occlude the infusion catheter line, inactivate the medications, or create an embolism, putting the client at significant risk for harm.[5] See Figure 2.2[6] for an example of a client’s existing fluids and medications being infused that must be checked for compatibility before IV push medication is administered in the same line and/or access site.
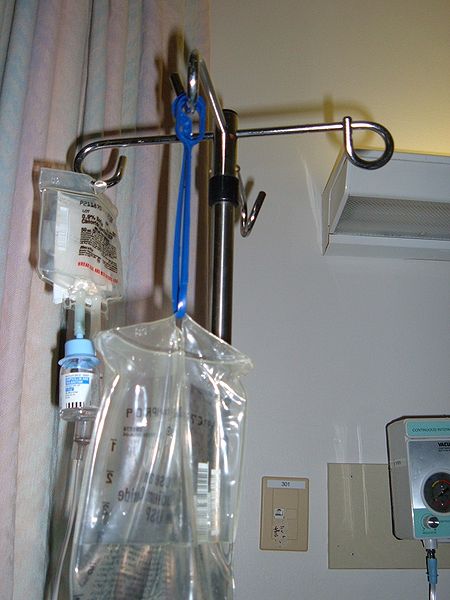
An additional potential disadvantage of administering medication via IV push when other fluids and/or medications are infusing is that the infusate can move backwards into the existing IV administration set if not performed correctly and thus reduce the amount of medication that reaches the client. For this reason, the nurse should pinch the existing tubing above the site of the hub in which the IV push medication is being administered.
In addition to leaching, many IV push medications require reconstitution to dissolve the medication powder into a fluid for administration. With reconstitution, there is a potential for nurse error in calculating total volume to be administered so the ordered dose reaches the patient.
The risk of patients experiencing speed shock with IV push medication administration is also a significant potential concern. Speed shock is characterized as an adverse systemic reaction when a foreign substance is introduced into the bloodstream. Speed shock may occur with IV push medication administration when the medication peaks very quickly. This sudden peak increases the risk of significant side effects. When medication is administered in a short period of time (typically in less than one minute), there is little opportunity to stop the medication if the client experiences an allergic response. Signs of speed shock include a systemic reaction such as tightness or pressure in the chest, irregular pulse, flushed skin, headaches, change in the level of consciousness, a feeling of impending doom, or cardiac arrest. Clients who have reduced liver and kidney function or those with cardiac problems are at increased risk of speed shock. If a nurse notes the signs of speed shock during IV push administration, they should immediately stop the infusion, maintain the IV line for emergency access, notify the provider, and begin CPR if indicated.
IV site complications are an additional disadvantage with IV push medication administration. Any time a medication or fluid is given into an IV site, there is increased risk for complications such as infiltration, extravasation, and phlebitis. Review information about these complications in Table 1.3a in the “Peripheral IV Access” section in the “Initiate IV Therapy” chapter.
See Table 2.2b for a summary of common advantages and disadvantages associated with the use of IV push medications.
Table 2.2b IV Push Medication Advantages and Disadvantages[7]
| Advantages | Disadvantages |
|---|---|
| Intravenous medications can deliver an immediate, fast-acting therapeutic effect, which is important in emergent situations, such as cardiac arrest or narcotic overdose. They are useful to manage pain and nausea by quickly achieving therapeutic levels, and they are more consistently and completely absorbed compared with medications given by other routes of injection. | Once an intravenous medication is delivered, it cannot be retrieved. When giving IV medications, there is very little opportunity to stop an injection if an adverse reaction or error occurs. IV medications, if given too quickly or incorrectly, can cause significant harm or death. |
| Doses of short-acting medication can be titrated according to patient responses to drug therapy. Medication can be prepared quickly and given over a shorter period of time compared to the IV piggyback route. | Any toxic or adverse reaction can occur immediately and may be exacerbated by a rapidly injected medication. |
| Minimal dilution is required for some medications, which is desirable for a patient’s fluid restrictions. | Infiltration and extravasation can cause tissue damage, nerve damage, and scarring. |
| There is minimal or no discomfort for the patient in comparison to receiving subcutaneous and intramuscular injections. | Not all medications can be given IV route. |
| Intravenous medications provide an alternative to the oral route for drugs that may not be absorbed by the GI tract. They are ideal for patients with GI dysfunction or malabsorption, as well as for patients who are NPO (nothing by mouth) or unconscious. | There is a high risk for infusion reactions, ranging from mild to severe because most IV medications peak rapidly (i.e., they have a quick onset of effect). A hypersensitivity reaction can occur immediately or be delayed and requires supportive measures. |
| IV push medication provides a more accurate dose of medication because none is left in the intravenous tubing. | The route for administering medications may damage surrounding tissues. There is an increased risk of phlebitis with highly concentrated medication, especially with small peripheral veins or a short venous access device. |
Safety Concepts
Checking Rights of Medication Administration
When administering IV push medications, it is essential for nurses to vigilantly check the rights of medication administration three times. What began as five rights of mediation administration has been extended to eight rights according to the American Nurses Association. These eight rights include the following[8]:
- Right patient: Check that you have the correct patient using two patient identifiers according to agency policy (e.g., name and date of birth).
- Right medication: Check that you have the correct medication and that it is appropriate for the client in the current context. Understand the purpose of the medication and why the client is receiving it.
- Right dose: Check that the dose is safe for the age, size, and condition of the client. Different dosages may be indicated for different conditions, and pediatric dosages are typically much lower than adult dosages. Be aware of the medication side effects, peak, and onset of action. The peak of the medication administration occurs when the medication is at the highest level in the client’s bloodstream. The onset of medication administration occurs when the action of the medication begins to take effect. It is important for nurses to be aware of both the peak and onset and of IV administration to help assess when client response to medication may start to be observed.
- Right route: Check that the route is appropriate for the client’s current condition. Is the medication available to be administered via IV push? Does it require dilution with a substance such as normal saline? Does it require reconstitution? Can it be administered via peripheral access, or does it require central line access into a larger size vein?
- Right time: Adhere to the prescribed scheduling of the IV medication. Additionally, the rate of administration of the IV medication and the post-procedure saline flush must be administered according to manufacturer recommendations in a drug reference.
- Right documentation: Always verify any unclear or inaccurate documentation prior to administering medications.
- Right reason: Verify this medication is being administered to this client at this time for the right reason. If signs and symptoms no longer warrant administration of the prescribed medication, notify the prescribing provider.
- Right response: After administering the IV push medication, the nurse must evaluate for expected outcomes with the time frame of expected onset and peak. The nurse must also evaluate for unanticipated adverse outcomes and notify the provider if expected outcomes are not achieved or adverse effects occur.
In addition to checking the eight rights of medication administration, it is important to collect any baseline assessment information and nursing implications for administration. For example, nurses may be required to have certain vital signs monitoring capabilities available when administering certain medications, a certain size vascular access device, or access into the central versus peripheral vascular system.
Additionally, it is important to consider the specific time frame for drug administration. Many IV medications must be infused over a period of time and cannot be pushed into the venous system rapidly due to potential adverse hemodynamic effects. Medications administered by direct IV route are commonly given very slowly per guidelines outlined in a drug reference guide. Nurses must routinely consult drug reference guides when administering IV push medications to check medication and fluid compatibilities and to ensure that medications are given at the correct rate to prevent complications.
Checking for Potential Incompatibilities
When administering medications via the intravenous route, it is also important to consider potential incompatibilities that may exist. Incompatibilities for the IV route are often organized into three different categories, including physical, chemical, and therapeutic issues.
- Physical: When one drug is mixed with other drugs or solutions, a product is produced that is unsafe for administration. An example would be mixing oil with a water base.
- Chemical: When a drug reacts with other drugs or solutions, resulting in alterations of the integrity and potency of the active ingredient. A cloudy or crystalline precipitate may form.
- Therapeutic: When agents are antagonistic to one another, resulting in an undesired pharmacological action in a patient. This is the largest class of incompatibilities.
It is critical that nurses administering IV push medications are aware of available reversal agents for that medication. For example, when administering an opioid such as fentanyl via IV push, the nurse must monitor for oversedation and respiratory depression. The nurse should have naloxone, the reversal agent, readily available and accessible if an adverse reaction occurs.
Checking Current Status of the Client
As with administration of any medication, nurses must ensure that the medication to be given is appropriate based on the client’s current condition. Therefore, associated physical assessment findings, vital signs, pain assessment, and laboratory results must be reviewed before administering IV push medications. For example, if administering morphine via IV push for pain management, the nurse should perform and document a detailed pain assessment prior to administration. Pre-assessment data guides the nurse in determining if morphine is appropriate to administer at this time or if a lower-tier pain medication is more appropriate. It also guides the nurse in determining if a medication should be withheld based on current signs and symptoms and the provider notified. Ultimately, if the medication is administered, the pre-assessment data will be used to compare post-administration data to determine the therapeutic effect of the medication.
The condition and appropriateness of the specific IV site that will be used for administration of IV push medication must be assessed prior to medication administration and monitored for signs of complications. If infiltration of a medication occurs at the site, there may be neutralizing agents that can be given to minimize the impact of the medication on the surrounding tissues. For example, phentolamine mesylate may be injected into the extravasation site of a vasopressor to prevent dermal necrosis. Furthermore, some medications have pH values that must be controlled with a buffering agent to create a more tolerable pH for infusion. Finally, medications that are more viscous may require larger IV cannula sizes to push the medication through the cannula. Medication administered via IV route should never be forced through the IV cannula line. Pushing medication forcefully through a blocked IV cannula may force a clot into the client’s circulatory system.
![]() Select an IV site with a large vein and IV cannula to use for IV push medication administration. Administration of medication through a large cannula allows for greater dilution and minimizes the chance of vascular irritation.
Select an IV site with a large vein and IV cannula to use for IV push medication administration. Administration of medication through a large cannula allows for greater dilution and minimizes the chance of vascular irritation.
Infection Control
Aseptic technique must be maintained throughout all IV push procedures, including preparing and maintaining equipment and administering IV push medications. Hand hygiene and aseptic non-touch technique (ANTT) must be performed when handling all IV equipment and accessing IV sites. These standards can be reviewed in the “Aseptic Technique” chapter in Open RN Nursing Skills. Cleansing techniques must be followed when accessing an IV site according to agency policy. Additionally, if a syringe becomes contaminated by contact with a nonsterile surface, it should be replaced with a new one to prevent introducing bacteria or other contaminants into the system.
- This work is a derivative of StatPearls by Herman & Santos and is licensed under CC BY 4.0 ↵
- Vallerand, A. H., & Sanoski, C. A. (2023). Furosemide. Davis’s drug guide for nurses (18th ed.). F.A. Davis. https://www.drugguide.com/ddo/view/Davis-Drug-Guide/51345/all/furosemide ↵
- “Stem-cells-iv-administration-dmd-ama-regenerative-medicine.jpg” by Alice Pien, MD is licensed under CC BY-SA 4.0 ↵
- Spencer, S., Ipema, H., Hartke, P., Krueger, C., Rodriguez, R., Gross, A. E., & Gabay, M. (2018). Intravenous push administration of antibiotics: Literature and considerations. Hospital Pharmacy, 53(3), 157–169. https://doi.org/10.1177/0018578718760257 ↵
- Institute for Safe Medication Practices. (2017, April 6). Two unsafe practices: Administration of a product with a precipitate and reuse of a saline flush syringe. https://www.ismp.org/resources/two-unsafe-practices-administration-product-precipitate-and-reuse-saline-flush-syringe#:~:text=If%20a%20precipitate%20is%20observed,organ%20failure%20or%20even%20death ↵
- “IV_pole_top_portion.JPG” by BrokenSphere is licensed under CC BY-SA 3.0 ↵
- This work is a derivative of Clinical Procedures for Safer Patient Care by British Columbia Institute of Technology and is licensed under CC BY 4.0 ↵
- American Nurses Association. (2021). ANA issue brief: Use of medication assistants/aides/technicians. https://www.nursingworld.org/~498e32/contentassets/a2ff1bd2d5ca467699c3bc764f7d9198/issue-brief-medication-aides-4-2021.docx ↵
A process of introducing a medication or fluid substance directly into the bloodstream via the venous system.
The action that occurs when a medication must be first metabolized or broken down prior to entering the blood.
An IV cannula that has been inserted into a vein and saline locked or clamped.
The formation of small crystals as the incompatible substances come in contact with one another.
An adverse systemic reaction when a foreign substance is introduced into the bloodstream.

